In this course we explain how dementia affects the brain and how Alzheimer’s disease differs from other types of dementia. We review behaviors you might see in people with mild, moderate, and severe dementia and describe communication issues you will encounter at different stages. We offer techniques to address behavioral issues, and tools to promote independence in all activities. Finally, we will discuss how to work with family members and caregivers who are caring for a person with dementia.
What Is Dementia?
Dementia is a collective name for the progressive, global deterioration of the brain’s executive functions. Dementia occurs primarily in later adulthood and is a major cause of disability in older adults. Although almost everyone with dementia is elderly, dementia is not considered a normal part of aging.
Dementia is caused by damage to a part of the brain called the cerebrum. The cerebrum fills up most of our skull and is divided into four lobes (one on each side of the head):
- Frontal
- Temporal
- Parietal
- Occipital
The cerebrum is what makes us human—it allows us to think, make plans, talk, and understand. It controls our memories and emotions. It helps us reason, make decisions, and tell right from wrong. It also controls our movements, vision, and hearing. Many of these areas of the cerebrum are damaged by dementia.
The Human Brain
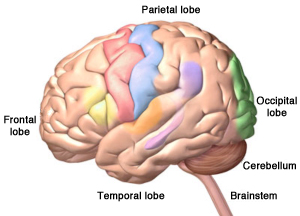
The four lobes of the cerebrum, plus the cerebellum and the brainstem. Alzheimer’s disease starts in the temporal lobe, an area of the brain associated with memories and emotions. Copyright, Zygote Media Group, Inc. Used with permission.
Dementia is a group of symptoms impacting cognitive functions such as memory, judgment, reasoning, and social skills as well as interfering with the ability to function in daily life. Dementia is progressive, meaning it gets worse over time. It is a terminal illness, meaning it will eventually lead to death. Alzheimer’s disease (AD) is the most common kind of dementia.
When someone has dementia, their thinking becomes less clear. Decisions are more difficult and safety awareness declines. People also get tired more easily. Emotions are also affected—that’s why people with Alzheimer’s disease and other types of dementia sometimes have difficulty controlling their emotions.
For people between the ages of 65 and 75, only about 5% will get any sort of dementia. For people over the age of 85, about 40% will experience some form of dementia. Even so, dementia is not considered a normal part of aging.
How the Brain Works
The brain is the most complex organ in the human body. This three-pound mass of gray matter contains more than 90 billion nerve cells with about 150 trillion connections. The brain is at the center of all human activity—it regulates the body’s basic functions, allows us to interpret and respond to everything we experience, and shapes our thoughts, emotions, and behaviors (NIDA, 2020).
A nerve call (neuron) has three major parts: (1) the cell body—the part of the nerve cell that contains the nucleus and other organelles, (2) the axon—an elongated process that carries the nerve impulse away from the cell body, and (3) dendrites—which receive nerve impulses from neighboring nerves and transmit them to the cell body.
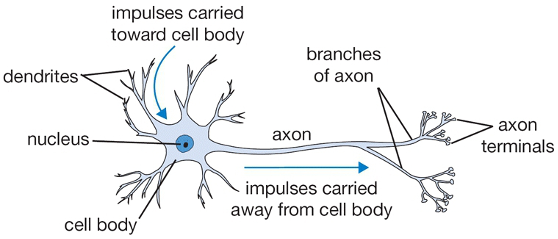
How brain cells communicate. An illustration of a healthy neuron showing the nucleus, cell body, dendrites, and axons. Source: WPClipArt.com. Used with permission.
A healthy nerve cell. Source: ADEAR, 2014. Public domain.
In healthy people, all sensations, movements, thoughts, memories, and feelings are the result of signals transmitted via billions of nerve cells, or neurons, in the brain. Neurons constantly communicate with each other through electrical charges that travel down axons, causing the release of chemicals across tiny gaps to neighboring neurons. Other cells in the brain, such as astrocytes and microglia, clear away debris and help keep neurons healthy (NIA, 2017).
[Healthy nerve cell image is from https://www.wpclipart.com/medical/anatomy/nervous_system/neuron/neuron.png.html.]
Most neurons in the human brain are myelinated. Myelin, also called white matter, is a fatty substance that surrounds the axon and increases the speed and efficiency of the nerve impulse. Myelin insulates the axon, preventing leakage of the electrical impulse into the surrounding fluid as well as providing structural support for the axon. Multiple sclerosis is an example of a disease in which immune system cells attack myelin, causing scar tissue to form, interrupting the smooth transmission of nerve impulses in the brain, spinal cord, and optic nerves.
How Does Dementia Affect the Brain?
In a person with Alzheimer’s disease, the most common form of dementia, toxic changes in the brain destroy healthy tissue. These changes may occur years, even decades, before the first signs of dementia appear. This process involves two proteins called tau and beta-amyloid, which accumulate in the brain, forming plaques and tangles.
Tau proteins accumulate inside neurons while beta-amyloid proteins slowly build up in the areas between neurons. As the level of amyloid reaches a tipping point, there is a rapid spread of tau throughout the brain.
But tau and beta-amyloid may not be the only factors involved in Alzheimer’s. Other changes that affect the brain may also play a role:
- The vascular system may fail to deliver sufficient blood and nutrients to the brain.
- The brain may lack the glucose (sugar) needed to power its activity.
- Chronic inflammation sets in as microglial cells* fail to clear away debris, and astrocytes react to distressed microglia.
*Microglial cells: cells of the brain that regulate brain development, maintenance of neuronal networks, and injury repair.
Eventually, neurons lose their ability to communicate. As neurons die, the brain shrinks, beginning in the hippocampus, a part of the brain important to learning and memory. People may begin to experience memory loss, impaired decision-making, and language problems. As more neurons die throughout the brain, a person with Alzheimer’s gradually loses the ability to think, remember, make decisions, and function independently (NIA, 2017).
Normal Brain Contrasted with AD Brain
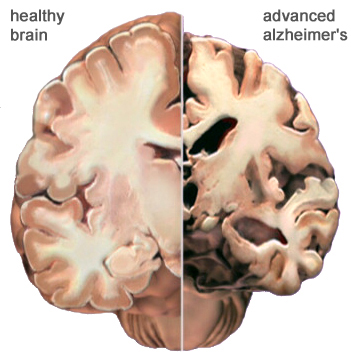
A view of how Alzheimer’s disease changes the whole brain. Left side: normal brain; right side, a brain damaged by advanced AD. Source: Courtesy of The Alzheimer’s Association. Used with permission.
Because dementia causes damage to the part of the brain that processes visual input, is can affect visual acuity, the size of a person’s visual field, and visual-spatial perception, affecting a person’s ability to see objects and the distance between those objects. It also impairs working memory, a type of memory that promotes active short-term maintenance of information for later access and use. The decline in working memory also affects language comprehension and visuospatial reasoning (Kirova et al., 2015).
Normal Age-Related Changes
We all experience changes as we age. Some people become forgetful when they get older. They may forget where they left their keys. They may also take longer to do certain mental tasks. They may not think as quickly as they did when they were younger. These are called age-related changes. This is a normal part of aging—it not dementia.
People experiencing age-related changes can easily do everything in their daily lives—they can prepare their own meals, manage their finances, safely drive a car, go shopping, and use a computer. They understand when they are in danger and know how to take care of themselves. Even though they might not think or move as easily or quickly as when they were young, their thinking is normal—they do not have dementia.
In some older adults, memory problems are a little bit worse than normal age-related changes. This is known as mild cognitive disorder. Mild cognitive disorder isn’t dementia. You won’t generally see personality changes, just a little more difficulty than is normal with thinking and memory. For some people, mild cognitive impairment gets worse and develops into dementia.
However, mild cognitive impairment does not always lead to dementia (Pandya et al., 2017). Recent research has looked into the possibility that a person with mild cognitive impairment may remain at this level or even revert back to normal cognition under certain circumstances.
Reversion rates from mild cognitive impairment to normal cognition among individuals aged 65 years and older were approximately 16% over one year in a clinic-based study and 28% to 55% in population-based studies over a two- to 12-year period. Reasons for these varying rates of reversion are likely due to differences in evaluation criteria, inclusion of participants with transient medical or comorbid neuropsychiatric symptoms, length of follow-up, and diagnostic accuracy (Pandya et al., 2017).
The table below describes some of the differences between someone who is aging normally and someone who is experiencing the effects of dementia.
Normal Aging vs. ADRD | |
|---|---|
Normal aging | AD or other types of dementia |
Occasionally loses keys | Cannot remember what a key does |
May not remember names of people they meet | Cannot remember names of spouse and children—don’t remember meeting new people |
May get lost driving in a new city | Get lost in own home, forget where they live |
Can use logic (for example, if it is dark outside it is nighttime) | Is not logical (if it is dark outside it could be morning or evening) |
Dresses, bathes, feeds self | Cannot remember how to fasten a button, operate appliances, or cook meals |
Participates in community activities such as driving, shopping, exercising, and traveling | Cannot independently participate in community activities, shop, or drive |
Stages of Alzheimer’s Disease and Other Types of Dementia
Alzheimer’s disease typically starts in an area of the brain called the hippocampus—the part of the brain responsible for new, short-term memories. This can cause a person with dementia—particularly someone with Alzheimer’s disease—to forget something that happened just a moment ago. Although most types of dementia start in one part of the brain, eventually the entire brain will be affected.
It is common to describe Alzheimer’s disease, as well as other dementias, as progressing in “stages”. The stages can be described as mild, moderate, and severe or early, middle, and late. Even though disease progression differs from person to person and varies depending on the type of dementia, we nevertheless associate certain symptoms and behaviors with these stages. The type of dementia, along with a person’s general health, co-morbid conditions, and family support can affect how fast and how far the dementia progresses.
Did You Know. . .
The National Institute on Aging and the Alzheimer’s Association have published guidelines aimed at improving current diagnosis, strengthening autopsy reporting of Alzheimer’s brain changes, and promoting research into the earlier detection of Alzheimer’s disease. These guidelines describe three stages of AD: (1) preclinical AD, (2) mild cognitive impairment, and (3) dementia due to Alzheimer’s disease:
- Preclinical AD: the stage in which changes have begun to appear in the brain but no cognitive or emotional symptoms are present.
- Mild cognitive impairment (MCI): a decline in cognitive function that falls between the changes associated with typical aging and changes associated with dementia.
- Dementia due to Alzheimer’s disease: a period in which symptoms become more obvious and independent living becomes more difficult.
Alzheimer’s Association, 2023
Mild Dementia
Brain Changes in Mild Dementia
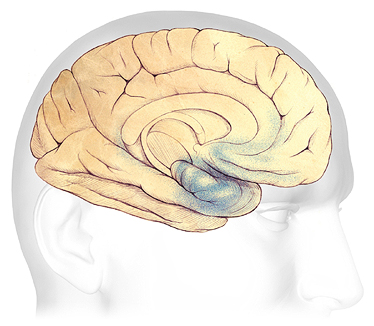
In the earliest stages of Alzheimer’s disease, before symptoms can be detected, plaques and tangles form in and around the hippocampus, an area of the brain responsible for the formation of new memories (shaded in blue). Source: The Alzheimer’s Association. Used with permission.
In the early, mild stage of dementia due to Alzheimer’s disease, plaques and tangles begin to cause damage within the temporal lobes, in and around the hippocampus. The hippocampus is part of the brain’s limbic system and is responsible for the formation of new memories, spatial memories and navigation, and is also involved with emotions.
Mild cognitive changes, which have likely been developing for several years, affect memory, decision-making, and complex planning. A person with mild dementia can still perform all or most activities of daily living such as shopping, cooking, yardwork, dressing, bathing, and reading. They may even continue to work but will likely begin to need help with complex tasks such as balancing a checkbook and planning for the future.

Trouble remembering recent events is a common symptom of mild Alzheimer’s disease. Source: NIA. Public domain.
Moderate Dementia
Brain Changes in Moderate Dementia
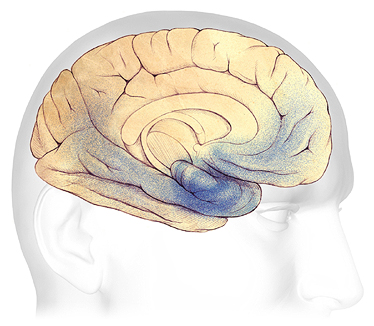
In mild to moderate stages, plaques and tangles (shaded in blue) spread from the hippocampus forward to the frontal lobes. Source: The Alzheimer’s Association. Used with permission.
As Alzheimer’s disease progresses from the mild to moderate stage, plaques and tangles spread to the areas of the brain involved with language, judgment, and learning. Work and social life can become more tiring and challenging. Speaking and understanding speech, the sense of where your body is in space, executive functions such as planning, logical thinking, safety awareness, and ethical thinking are affected. Many people are first diagnosed with Alzheimer’s disease in this stage.
Severe Dementia
Brain Changes in Severe Dementia
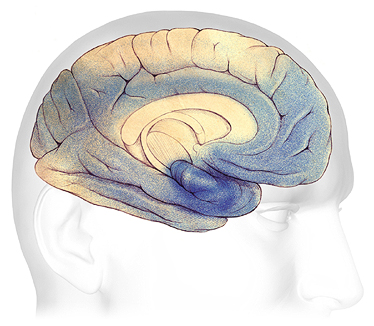
In advanced Alzheimer’s, plaques and tangles (shaded in blue) have spread throughout the cerebral cortex. Source: The Alzheimer’s Association. Used with permission.
In the later or severe stage, damage is spread throughout the brain. Because so many areas of the brain are affected, individuals may lose their ability to communicate clearly, to recognize family and loved ones, and to care for themselves.
People with severe dementia can lose all memory of recent events although they often still remember events from the past. They are easily confused, tire easily, are unable to make decisions, and cannot think logically. Speech, communication, and judgment are severely affected. Sleep disturbances and emotional outbursts are very common.
Stages of Other Types of Dementia
Although Alzheimer’s dementia worsens steadily over time, other types of dementia may progress differently. Because vascular dementia is caused by a stroke or series of small strokes, dementia may worsen suddenly and then stay steady for a long period of time—especially if the underlying cardiovascular causes are addressed.
In Lewy body dementia, which is often associated with Parkinson’s disease, symptoms—including cognitive abilities—can fluctuate drastically, even throughout the course of a day. Nevertheless, the dementia is progressive and worsens over time. In the later stages, progression is similar to Alzheimer’s disease.
Frontal-temporal dementia generally starts at an earlier age than Alzheimer’s disease. In the early stage—depending on which lobe of the brain is affected, there are changes in personality, behavior, emotions, and judgment. There may also be early changes in language ability, including speaking, understanding, reading, and writing. Motor decline can also occur as the disease progresses. This is characterized by difficulties with movement, including the use of one or more limbs, shaking, difficulty walking, frequent falls, and poor coordination.
