The fragile skulls and developing brains of infants and young children make them highly susceptible to serious injuries from violent shaking, blunt force trauma, or both. In preverbal children, diagnosis is further complicated by the patient’s inability to say what happened. Diagnosis must be a multidisciplinary effort, gathering clues from the child’s psychosocial environment, noting risk factors within the family, and assessing the consistency (and likelihood) of the adult’s report of the cause.
2.1 Symptoms and Types of Pediatric Injuries
A confident diagnosis must be able to stand up to legal scrutiny; thus, it is important to realize how common unintentional injuries are, and how they present. Unintentional injuries, in which abuse plays no role, are the most common cause of death among children the world over (Li et al., 2024).
One of the most common childhood injuries is limb fracture, with an especially high incidence among children with learning disabilities, attention deficit hyperactivity disorder (ADHD), or executive function deficits (Rosenblum et al., 2022).
ThinkFirst National Injury Prevention Foundation is a nonprofit advocacy organization founded by neurosurgeons to prevent brain, spinal cord, and other traumatic injuries. According to ThinkFirst, symptoms may include (Wilson et al., 2021):
- lethargy
- poor suckling or swallowing
- poor feeding or eating
- irritability
- difficulty staying awake
- vomiting
- rigidity
- tremors
- inability to lift head
- pale or bluish skin
- difficulty breathing
- paralysis
- coma
Children do get bruised from playing, though bruises on an infant who is not independently mobile should be considered suspicious. Toddlers and older children commonly have bruises that are not related to abuse on the front part of their bodies, especially bony areas like the knees, shins, elbows, and forehead. Even small bruises can indicate a serious injury. A child with a minor bruise on the belly could be suffering a liver laceration from being punched in the stomach. Bruises on the ears could be a clue that the child has suffered a head injury due to abuse (Norton Children’s, 2022).
2.2 Mechanism of Injury
The baby’s head is large and heavy. The baby’s brain is not fully developed and is fragile. It has the consistency of very soft tofu. Babies have weak neck muscles. When a baby is violently shaken, the head moves around a lot, causing the brain to move vigorously back and forth inside the skull. This can lead to brain damage.
Tanya Minasian, 2021
Shaking is extremely violent. It can be as damaging as a high-speed automobile accident.
Shaken baby syndrome does not result from gentle bouncing, playful swinging, tossing a child in the air, or jogging with a child. Nor is it very likely to occur from accidents such as falling off chairs or accidentally being dropped from a caregiver's arms. The adult perpetrator usually holds the child under the arms and shakes, causing the head to flex, extend, and rotate on the body at a high rate of speed, with both hyperflexion and hyperextension. The violent movements of the brain within the skull can easily rupture the delicate system of veins in the brain (Laurent-Vannier, 2022).
The brain’s venous system drains the capillary network that supplies the brain, removing waste products like carbon dioxide and allowing the circulation of fresh blood throughout the body. Even minor trauma or abrupt deceleration can damage some of these veins, resulting in a subdural hematoma (Hufnagle and Tadi, 2025). Because the lower part of the brain regulates breathing and heart rate, victims of abusive pediatric head trauma may suffer from lifelong cognitive and physical health problems.
Reported injuries are most likely when the baby was shaken and then its head struck something. The perpetrator is thus able to point to the wound and defer attention from the internal damage due to shaking.
Even hitting a soft object, such as a mattress or pillow, may be enough to injure newborns and small infants. Children's brains are softer, their neck muscles and ligaments are weak, and their heads are large and heavy in proportion to their bodies. The result is a type of whiplash, like what occurs in some auto accidents (MedlinePlus, n.d.).
2.3 Falls
While short falls may cause fractures and, less commonly, even serious head injuries, clinicians can differentiate abusive head trauma from accidental head injury. Common features of accidental head trauma are swelling and bruising in the scalp, epidural hemorrhage, and isolated skull fracture. Common features of abusive head trauma often include clusters of seizures, intracerebral hemorrhage without skull fracture, and multiple hemorrhages, including subdural and mixed density hemorrhages (Hung, 2020).
One study of children who died after falling 1 to 4 feet found co-existent evidence of abuse. Though retinal hemorrhage is common in both accidental and abusive head trauma, abuse more frequently causes bilateral hemorrhage, while accidents are more likely to cause a hemorrhage in only one eye (Hung, 2020).
Abusive Head Injury in an Infant
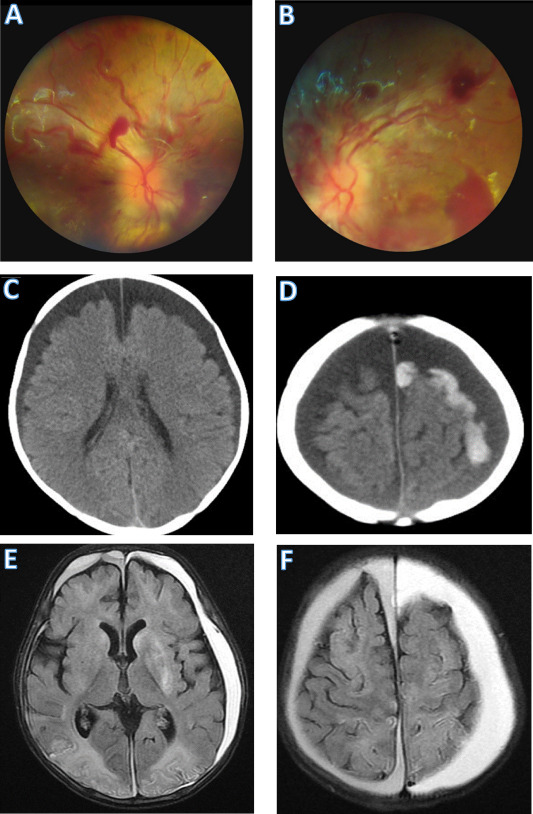
Fig. 1. Abusive head injury in a 1-year-old female infant. (A) Right eye ground, (B) left eye ground shows diffuse intraretinal and preretinal hemorrhages. (C) Initial non-contrast CT demonstrated bilateral chronic subdural effusion, plus (D) acute left subdural hematoma. MRI (E) and (F) taken 2 weeks after bilateral subdural drainage showed asymmetric subdural fluid, as well as several parenchymal ischemic changes over frontal lobes, basal ganglia (more on left), and posterior lobes (Hung, 2020).
In the United States, accidental falls are the leading cause of nonfatal injury among children 0 to 14 years old. They account for about 2 million emergency department visits and more than 30,000 hospitalizations each year. They are the leading cause of traumatic brain injury in children, responsible for 90% of TBIs in zero- to 4-year-olds and 42% of TBIs in children from 5 to 14 (Omaki et al., 2023).
Most of the injuries from falls are treated and released, but 2.7% result in hospitalization. Children who fall from a caregiver’s arms are more than twice as likely to be hospitalized as children who fall from another source, like beds or other furniture (Omaki et al., 2023).
