Managing symptoms and behaviors that arise in a person living with dementia requires patience and compassion, and sometimes, the skill of a detective. To successfully manage a challenging behavior, caregivers must try to understand what is causing the behavior. Very often, it is due to some sort of unmet need.
Good management means creating a safe and comfortable physical environment, learning how to divert the person’s focus to a meaningful activity, and encouraging regular physical activity and social engagement. For a person living with dementia, negative environmental influences, frustration, boredom, pain, or untreated medical or medication issues can lead directly to challenging behaviors.
2.1 Symptoms and Behaviors Associated with Each Stage of Dementia
A symptom is a noticeable change in the body or the mind. Symptoms change as a person’s dementia progresses, often leading to changes in a person’s behavior. For some people, symptoms associated with dementia worsen quickly, while for others, symptoms progress more slowly.
We associate certain symptoms and behaviors with stages. But keep in mind that the type of dementia, along with a person’s general physical and psychological health, can affect symptoms and behaviors as much as the stage of the person’s dementia.
2.1.1 Mild Dementia
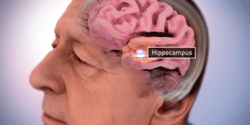
Location of the hippocampus. Source: Image courtesy of the National Institute on Aging/National Institutes of Health. Public domain.
In early, mild Alzheimer’s disease, plaques and tangles appear in the part of the brain responsible for memory and learning. This part of the brain is called the hippocampus. It converts recent, short-term memories into long term memories by storing, organizing, and retrieving memories.
Brain Changes in Mild Dementia
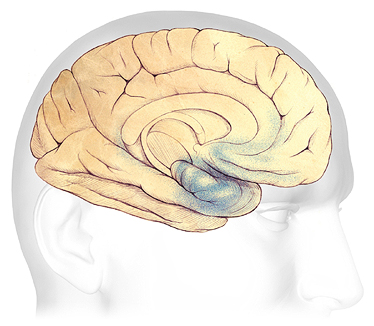
In early AD, sometimes before symptoms can be detected, plaques and tangles begin to form in and around the hippocampus (shaded in blue). Source: The Alzheimer’s Association. Used with permission.
The inability to recall something that just happened (short-term memory) is a common symptom in the early stage of Alzheimer’s disease and other types of dementia. A person can also have difficulty understanding where they are in relation to nearby objects (visual-spatial memory) and have trouble finding words (verbal memory). Logical thinking, language, and judgment are often mildly affected.
Even when symptoms are mild, a person’s behavior can begin to change, especially with Alzheimer’s disease and some other types of dementia. People often know something is wrong and may try to hide their mild confusion from friends, coworkers, and family. These changes can cause depression, stress, mood changes, and anxiety.
2.1.2 Moderate Dementia
As symptoms associated with dementia progress to the moderate stage, plaques and tangles spread forward to the areas of the brain involved with language, judgment, and learning. Many people are first diagnosed with Alzheimer’s or another type of dementia at this time.
During this stage, work and social life become more difficult. Damage affects the areas of the brain involved with:
- judgment and logical thinking
- speaking and understanding speech
- safety awareness
- planning and sequencing tasks
- ethical thinking
Because of memory problems and confusion, a person living with moderate dementia may find daily tasks more difficult and will very likely need help with personal finances, medications, and medical management.
Brain Changes in Moderate Dementia
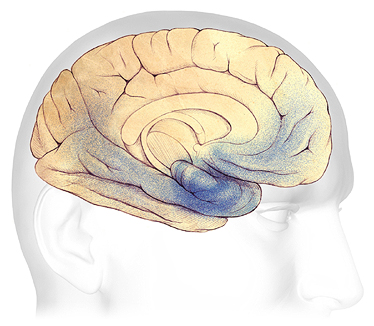
As symptoms progress from mild to moderate, plaques and tangles spread from the area of the hippocampus (dark blue) forward to the frontal lobes (shaded in light blue). Source: The Alzheimer’s Association. Used with permission.
In the moderate stage, behavioral changes become more obvious to caregivers. Some people may begin to repeat questions, call out, or repeatedly demand your attention. Sleep problems, anxiety, and agitation can develop.
A person living with moderate dementia is usually still able to walk. This is because the part of the brain that controls movement is not affected. A caregiver may need to provide more direct monitoring of daily activities and the person living with dementia may no longer be safe on their own.
2.1.3 Severe Dementia
For a person living with severe dementia, because so many areas of the brain are affected, the ability to care for oneself is severely affected. Confusion, indecisiveness, sleep disturbances, and emotional outbursts are very common.
Brain Changes in Severe Dementia
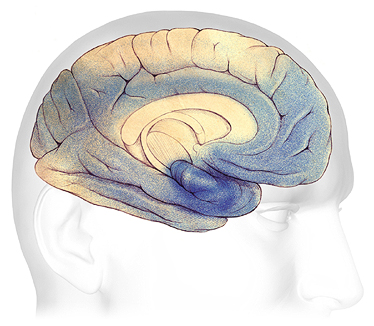
In advanced Alzheimer’s, plaques and tangles have spread throughout the brain (shaded in blue). Source: The Alzheimer’s Association. Used with permission.
Behaviors that emerged in the middle stage, when executive functioning and communication abilities typically decline, continue in the severe stage. In the severe stage, an individual living with dementia may become increasingly nonverbal, and mobility challenges can become more pronounced.
All sorts of challenging behaviors can occur at this stage, especially if caregivers (including professional caregivers) are poorly trained, easily frustrated, or highly stressed. A person living with severe dementia may wander, rummage, or hoard. Screaming, swearing, crying, shouting, loud demands for attention, negative remarks to others, and self-talk are common. These outbursts are often triggered by unmet needs such as frustration, boredom, loneliness, depression, cold, heat, loud noises, or pain.
A person experiencing severe dementia loses a great deal of independence, and around-the-clock care may eventually be needed. Caregivers will likely need to oversee and directly assist with eating, bathing, walking, dressing, and other daily living activities.
2.1.4 Symptoms and Behaviors at the End of Life
As a person living with dementia nears the end of their life, they may be completely dependent on caregivers. If they are unable to communicate their needs and desires using speech, caregivers must learn to recognize nonverbal cues. A person at this stage may be bedridden, or nearly bedridden.
Immobility, swallowing disorders, and malnutrition can occur. Because people at this stage are much less active than in earlier stages of dementia, there is an increased risk of developing acute conditions that can lead to illness or death. Pneumonia, a common cause of death in older adults living with Alzheimer’s or another type of dementia, is a particular concern.
At the end of life, it is likely that both short- and long-term memory are affected. Sensory changes such as loss of vision and hearing mean a person can be startled by loud noises and quick movements. Depending on the type of dementia, a person may experience agitation, psychosis,* delirium,** restlessness, and depression.
*Psychosis: loss of contact with reality.
**Delirium: a sudden, severe confusion that can be caused by infections, a reaction to medications, surgery, or illness.
2.2 General Problem-Solving Approach to Challenging Behaviors
Problem solving is an important skill for caregivers and healthcare providers to develop when working with a person living with dementia. Compassion, reassurance, and active listening can reduce or even prevent many challenging behaviors. These practices can also reduce the use of antipsychotics and other medications often used to manage challenging behaviors.
The “ABC” model emphasizes data gathering and problem-solving. This approach helps providers and caregivers understand when and how often a particular behavior occurs. It is particularly effective when successful strategies are shared by staff, caregivers, and family members.
The ABC Approach considers:
A (Antecedent) What caused the behavior?
B (Behavior): What is the behavior?
C (Consequence): What are the consequences of a behavior?
The ABC approach also encourages caregivers and healthcare providers to examine their own behaviors and responses. Understanding your own biases, frustrations, and triggers helps you approach a person struggling with dementia with patience and compassion.
Mrs. Washington
Mrs. Washington has moderate to severe dementia due to Alzheimer’s disease and lives in a nursing home. Tuesday is her shower day. A nursing assistant helps her undress in her room, covers her with a blanket, and wheels her to the shower room using a rolling commode chair. When they leave the room and enter the hallway, Mrs. Washington starts to fidget. As they move into the hallway, she begins to yell and protest. When she is rolled into the shower she screams, grabs the door, and tries to push her caregiver away.
Antecedent (what caused the behavior): In her room, the nursing assistant helps Mrs. Washington undress, then wraps her in a bath blanket. Unable to find a shower chair, she helps Mrs. Washington into a toilet chair. Mrs. Washington’s bottom is hanging out of the hole in the chair, which embarrasses her. She tries to stop the caregiver from wheeling her out into the hallway by grabbing at the doorway as they exit. She says “No! No!” but the caregiver tells her she is dirty and needs a shower, which embarrasses Mrs. Washington even more.
Behavior (what is the behavior): By the time Mrs. Washington reaches the shower room she is very upset. She slaps the nursing assistant and repeatedly grabs the shower room door. The nursing assistant manages to get Mrs. Washington into the shower room, but when she turns on the water, Mrs. Washington screams, grabs the shower hose, and pushes the nursing assistant away. She sprays water all over the nursing assistant and into the hallway.
Consequence (what are the consequences of the behavior): Mrs. Washington, staff members, and Mrs. Washington’s daughter are all upset. The situation was unpleasant for everyone and now Mrs. Washington is refusing to shower.
Discussion: Mrs. Washington’s daughter has told the nursing staff that her mother prefers to undress in the shower room and hates being wheeled half-naked down the hall. The nursing assistant bathing her today is new and hasn’t been told about Mrs. Washington’s preferences.
To address Mrs. Washington’s concerns, staff must communicate preferences such as these. Consider whether she needs to have a shower or if there are other ways of bathing that might be more acceptable to her. Use the proper equipment to take Mrs. Washington to the shower, rather than a toilet chair.
Find out how Mrs. Washington bathed earlier in life. Allow her to participate in her bathing even if it takes longer. Ask her if she wants a shower. Allow her to undress in the shower room rather than in her room. Talk with her during the procedure and get continual feedback from her. Ask her questions such as “Is this too hot?” “Do you want to wash your face?” “Are you cold?”
2.3 Strategies for Addressing Common Challenging Behaviors
Addressing common challenging behaviors in a person living with dementia requires training, strategies, communication, and techniques that change as a person’s symptoms and behaviors change. Because dementia is progressive, strategies that work with mild dementia may not work in the later stages of dementia.
Although not a comprehensive list, certain behaviors are common in people living with dementia. This includes agitation, aggression, psychosis, wandering, rummaging, hoarding, and sleep disturbances.
2.3.1 Agitation and Aggression
Agitation, aggression, and psychosis are labels on behaviors that are often caused by environmental or personnel approaches rather than being due entirely to the person’s brain changes. These reactions should be viewed as an expressive communication of a possible unmet need.
Teepa Snow, STOP Treating Behaviors with Restraining Medications
Agitation and aggression are among the most common and challenging symptoms in older adults living with dementia. These behaviors worsen a client’s daily functioning, increase the chance of injury, and increase the likelihood of hospitalization and long-term care placement. They also impose a significant burden on caregivers and healthcare systems (Lichwala et al., 2026).
Agitated behaviors can include:
- Irritability and worry
- Restlessness, inability to settle down
- Pacing
- Confusion
- Loud demands, shouting
- Obscene language
Aggressive behaviors can include:
- hitting, punching, kicking, pushing
- throwing objects or using objects to hit or lash out
- engaging in inappropriate sexual advances or touching
- resident-to-resident aggression, especially verbal aggression
Agitated and aggressive behaviors often occur during personal care tasks involving close contact. A person may feel threatened or feel their personal space is being violated. Depending on the type and severity of a person’s cognitive changes, agitated and aggressive behaviors can become more pronounced as a person’s dementia progresses.
To manage aggressive behaviors, staff and caregiver training are essential. Psychosocial and environmental interventions, and recognition of personal habits and patterns, can reduce or even eliminate agitated or aggressive behaviors.
When you encounter agitated and aggressive behaviors, take a deep breath, slow your movements, and be respectful of personal space. Always introduce yourself before entering a person’s room. When you approach a person who is agitated:
- Speak calmly and actively listen to their complaints or frustrations.
- Reassure the person that they are safe.
- Try to distract the person by offering an activity or chore.
- Try to reduce noise and clutter.
- Consider physical and medical causes of a person’s agitation.
Antipsychotic medications are often used to treat agitated and aggressive behaviors in people living with dementia. They should be used for the shortest possible time and only as a last resort.
Charles Lashes Out at Frances
Frances, a physical therapist working in a skilled nursing facility, was helping Charles go from his room to the activities room. Charles, seated in his wheelchair, was at first quiet and relaxed as they moved down the hall.
Antecedent (what caused the behavior): In the hallway outside the activities room, Frances was stopped by two co-workers who engaged her in a conversation about another resident. All three were standing behind Charles, talking animatedly. Frances placed her hand on Charles’s shoulder to try to include him in the conversation.
Behavior (what is the behavior): When Frances touched Charles, he angrily pushed her hand away, yelling in a loud voice “Stop that!” When one of Frances’s co-workers tried to calm him down, Charles yelled “Stop that! Stop that!” and tried to hit the coworker.
Consequence (what are the consequences of the behavior): Charles was upset, Frances was upset, and the co-worker almost got hit in the face. Frances and her co-workers could have avoided this incident entirely. Instead of ignoring Charles and talking over him, the physical therapist should have stopped, kneeled beside Charles, made eye contact, offered her hand, and introduced her colleagues. She should have asked Charles if she could talk for a moment with her co-workers and included him in the conversation. Better yet, she could have asked her colleagues to wait until she and Charles finished what they were doing and continued the conversation after Charles was seated at the activities table.
Discussion: This is a situation that didn’t need to agitate Charles. Talking over and ignoring someone can be extremely upsetting. If Frances and her co-workers had been respectful of Charles and validated his needs and preferences, they could have avoided upsetting him and modeled good practice for their co-workers.
2.3.2 Dementia-Related Psychosis
Dementia-related psychosis occurs when a person experiences symptoms such as delusions, paranoia, or hallucinations. A delusion is a false belief or a misinterpretation of a situation. For example, a person living with dementia might confuse her daughter with her mother or she might accuse someone of stealing an item that was simply misplaced.
Paranoia is a type of delusion in which a person may believe—without a good reason—that someone is lying to them, being unfair, or are “out to get me.” This can cause a person to become suspicious, fearful, or jealous of other people. Paranoia often includes people close to the person living with dementia (caregivers, family members, or friends).
Hallucinations occur when a person hears, tastes, smells, sees, touches, or feels something that is distorted or not there. For example, a person may see shadows, cats running through the room, or images of threatening people or things (Fischer, 2022).
Visual hallucinations can occur in the moderate to severe stage of dementia and are particularly common in people with Lewy body dementia.* For a person living with Lewy body dementia, antipsychotic medications can make hallucinations worse.
*Lewy body dementia: a type of dementia with cognitive decline, “fluctuations” in alertness and attention, visual hallucinations, and slowness of movement, difficulty walking, or rigidity (stiffness).
The first step in the management of delusions and hallucinations is to rule out delirium or another acute medical cause. Observing a person’s behavior and listening to what they have to say often helps caregivers uncover the root cause of the delusion or hallucination.
For a person with new onset of visual hallucinations, the number one cause is medication side effects. For this reason, all medications the person is receiving should be regularly and carefully reviewed.
Acute health issues such as urinary tract infections or environmental factors such as poor lighting or sensory overload can contribute to delusions and hallucinations. Brain changes can also contribute to hallucinations, especially changes related to sensory awareness.
When communicating with someone who is experiencing paranoia or delusions, remember that the delusion is very real for that person. Do not argue or try to correct the person. Explaining the truth of the situation does not work. Do not agree or validate the paranoia or delusion—try to respond to the person’s emotion. For hallucinations, it is often helpful to decrease auditory and visual stimuli. It is also important to evaluate the person for a visual or hearing impairment.
What Do You Think?
Consider that the claims by the person living with dementia may be real. Complaints of strangers entering several resident rooms and stealing items at a Florida nursing home were attributed to dementia, hallucinations, and paranoia by healthcare providers (including nurses and physicians). As the complaints mounted, managers decided to install cameras in the alley next to the facility. It turned out that several of the sliding glass doors facing the alley had broken locks. The cameras showed that people were indeed entering rooms at night and rummaging through residents’ drawers and closets. There truly were people entering resident rooms and stealing items!
2.3.3 Wandering
Wandering and exploring are activities we all enjoy. It can occur at any stage of a person’s dementia. Symptoms can vary depending on the person and the type of dementia. But, because a person living with dementia might be at risk for falls or injury, providers and caregivers often see wandering as a problem and try to control or prevent this behavior. However, preventing a person from safely wandering creates other problems, such as boredom, loss of social interaction, stigma, loss of conditioning, pain and discomfort, and even skin breakdown.
Wandering can involve moving to a specific location, lapping or circling along a path, pacing back and forth, or wandering at random. People may wander out of habit or because they are convinced something needs to be done. They may think they need to return home after work, cook dinner, walk the dog, exercise, or search for something they think they have misplaced. The most important goal is to prevent a person from wandering into unsafe areas, other residents’ rooms, or eloping* from a facility.
*Eloping: When a person wanders away or leaves a facility or home unsupervised or unnoticed.
Wandering is a common problem seen in people living with almost all types of dementia. Nearly 60% of people living with dementia will wander during the course of their disease. Wandering can happen at home or in the community. In institutional settings, wandering occurs in about 40% of clients (Anu et al., 2024).
Wandering is more common in someone who experienced stressful events throughout their life or a person who responds to stress by engaging in physical activities. People with an outgoing personality, who enjoy music, and who were socially active throughout their life are more likely to wander than less active, introverted people.
Managing wandering behaviors in a person living with dementia requires a thoughtful and creative approach. Understanding the reasons for wandering should include regular review of medications to make sure wandering is not the result of medication side effects, overmedicating, or drug interactions.
Address wandering by:
- Redirecting a person to a purposeful activity
- providing safe, looping wandering paths with interesting rest areas
- installing rails and grab bars
- providing regular exercise
- offering to wander with the person.
Engaging a person in simple chores such as folding laundry or assisting with dinner can give them a sense of purpose and fulfillment. Electronic devices attached to the person’s ankle or wrist alert staff or family members when someone has wandered out of a designated area. Subjective barriers such as grid patterns on the floor in front of exit doors, camouflage, and concealment of doors and doorknobs, have been shown to discourage a wanderer from exiting a building.
Did you Know. . .
To protect people who wander away from their home or care facility, Florida maintains a Silver Alert program for cognitively impaired older adults who become lost while driving or walking. The Silver Alert program broadcasts information to the public so they can assist in the rescue of the endangered person and notify law enforcement with helpful information. For more information, contact the Silver Alert information line, local law enforcement, or the Florida Department of Law Enforcement either online or by phone at 888 356 4774.
The Wanderer
Elena is a resident in a five-story nursing home in Miami. She has moderate dementia and although she is non-ambulatory, she is very good at propelling her wheelchair with her feet. After breakfast in her room, an aide wheels her to the activities room and leaves her alone at a table with a jigsaw puzzle. After about 15 minutes Elena gets bored with the puzzle, exits the activities room, and heads down the hall. She is stopped twice by staff members, who turn her back toward the activities room with a reprimand.
When the staff members are out of sight, Elena turns back and continues in the direction she was headed. She stops near an elevator, where she sits for a while watching people come and go. Several more staff members pass by and gently remind her not to get on the elevator. Each time she is left in the same place next to the elevator. Finally, when no one is looking, Elena wheels into the elevator.
Antecedent (what caused the behavior): Elena is curious and used to like walking around Miami, exploring the different neighborhoods. She was never one to sit around doing nothing. She was bored with the jigsaw puzzle and wanted to do something more interesting. She rolls out into the hallway and stops near an interesting door that opens and closes with a satisfying swoosh sound. The people going in and out of the door smile at her.
Behavior (what is the behavior): The door to the elevator is an interesting visual cue and Elena enjoys seeing people coming and going. People talk to her—and she likes the interaction—but she doesn’t understand what they are saying. She sits for a while watching people come and go and as the opportunity arises, she enters the elevator. When the door opens on the ground floor, she wheels out of the elevator, heads to the front door and out onto the street. Her behavior is consistent with her personality and her previous habits.
Consequence (what are the consequences of the behavior): Once she gets into the elevator, Elena’s lack of safety awareness puts her at risk. Fortunately, someone sees her wandering down the middle of the street and helps her return to the nursing home.
Discussion: Large nursing homes are busy places, often understaffed, and often poorly designed for people living with dementia. Nevertheless, caregivers and healthcare providers should try to understand the reason for Elena’s wandering and come up with activities that are appropriate for her. Regular medications reviews will help staff understand if Elena’s behavior is related to medication side effects, overmedicating, or drug interactions.
To keep Elena out of the elevator:
- Redirect her to a purposeful activity.
- Provide places where she can wander safely.
- Schedule regular exercise.
- Offer simple, meaningful chores.
- Attach an electronic device that alerts caregivers when she has wandered out of a designated area.
- Place a plastic PVC pole on the back of her wheelchair and a horizontal pole across the entrance to the elevator so that she is physically stopped from entering the elevator.
- Take her for regular outings outside the building.
- Allow her to keep a bird or pet in her room.
- Provide safe, meaningful outdoor activities.
2.3.4 Rummaging and Hoarding
Rummaging and hoarding are behaviors in which a person gathers, hides, or puts away items in a secretive and guarded manner. Memory loss, poor judgment, and confusion contribute to rummaging and hoarding. Rummaging and hoarding are not necessarily dangerous or unsafe, but these behaviors can be frustrating for caregivers.
Rummaging and hoarding are obsessive/compulsive behaviors. A person who feels a strong need to rummage or hoard can be remarkably persistent and secretive, making it difficult for caregivers to address these behaviors. Hoarding is associated with insecurity, fear, anger, and the desire to hold onto possessions and memories from the past. A person who hoards may fear losing money or possessions. They may feel a lack of control or a need to “save for a rainy day.”
Rummaging through familiar items can create a sense of safety and security. Confusion can lead to rummaging through another person’s belongings, which can be particularly frustrating for other people.
To address rummaging and hoarding behaviors, try to determine what triggers the behavior and look at the consequences, if any. Look for patterns and carefully observe the person’s hiding places. The reason for rummaging and hoarding may not be clear to you but there may be a perfectly good reason why someone living with dementia is engaging in these behaviors.
The rummaging impulse might be satisfied by creating a rummaging room or a bag or drawer of items that the person can pick through. Rummaging through another person’s belongings can be prevented by installing locks on drawers and closets. Restricting all rummaging and hoarding can be frustrating for a person who enjoys these activities.
In facility settings, reduce clutter and label cabinets, doors, and closets (with words or pictures). Poisonous items should be stored away from common areas in locked cabinets.
2.3.5 Sleep Disturbances
More than half of people living with dementia experience some sort of sleep disturbance due to comorbid medical conditions and environmental factors. Common sleep problems include insomnia, fragmented sleep, obstructive sleep apnea*, rapid eye movement sleep behavior disorder**, and restless legs syndrome. Individuals may have trouble falling asleep or staying asleep due to altered circadian rhythms*** and increased confusion during the night (Mukherjee et al., 2024).
*Obstructive sleep apnea: a syndrome caused primarily by the collapse of the upper airway during sleep.
**Rapid eye movement sleep behavior disorder: a sleep disorder in which individuals physically and/or vocally act out vivid, often unpleasant dreams and sudden, involuntary arm and leg movements during REM sleep.
***Altered circadian rhythms: disruption in the body’s sleep-wake cycle.
Comorbid medical conditions that can affect sleep in older adults living with dementia include:
- cardiovascular disease
- diabetes
- depression and anxiety
- thyroid disorders (hypothyroid and hyperthyroid)
- untreated or poorly treated pain
In 2024, the Center for Medicaid and Medicare Services (CMS) published guidelines that require non-pharmacologic interventions for sleep disturbances must be tried and documented before using sedatives or psychotropic medications in a person living with dementia (CMS, 2024).
Non-pharmacologic treatments can include (Mukherjee et al., 2024; CMS, 2024):
- cognitive-behavioral therapy for insomnia
- minimizing environmental disruptions (reducing nighttime noise and excessive light).
- avoiding stimulating activities close to bedtime
- encouraging good sleep hygiene (a regular bedtime routine and a warm comfortable sleeping environment)
- restricting caffeine, nicotine, and alcohol
In addition to affecting the health and quality of life of the person living with dementia and their caregivers, sleep disturbances can contribute to some challenging behaviors. CMS requires that sleep disturbances be evaluated when a person exhibits agitation, anxiety, wandering, or changes in cognition. This includes looking for potentially treatable causes such as pain and discomfort, hunger and thirst, the need to urinate, infections, and adverse drug reactions.
Sleep disturbances can lead to “sundown syndrome,” a set of symptoms or behaviors that emerge in the late afternoon or early evening. Managing sundown syndrome involves a combination of environmental, behavioral, and medical interventions. A consistent daily routine, regular physical activity, soothing and familiar activities in the late afternoon, and a calm and a comfortable environment can improve sleep and decrease sundowning (Mukherjee et al., 2024).
Benzodiazepines, which have a hypnotic sedative effect are currently the most widely prescribed medications for sleep disorders in older adults. Despite their widespread use, concerns remain regarding their potential for tolerance, dependence, and adverse effects such as cognitive impairment (especially in older adults) (Chavez-Mendoza, 2025).
Benzodiazepine dependence has been associated with severe depression and anxiety and impaired cognitive and psychosocial function. In older adults, increased sensitivity to benzodiazepines can increase the risk of confusion, disorientation, and falls (Chavez-Mendoza, 2025).
Recently, non-benzodiazepine hypnotics, commonly known as Z-drugs, have been suggested as effective alternatives due to their similar mechanism of action. They may improve sleep quality, lower dependency risks, and reduce adverse effects compared to benzodiazepines (Chavez-Mendoza, 2025).
Treating sleep disturbances involves looking for potentially treatable causes. This includes treating pain and discomfort, hunger and thirst, the need to urinate, infections, and adverse drug reactions.
2.4. Physical and Chemical Restraints
When—if ever, in the eternal dementia care merry-go-round of staff shortages, budget limitations, regulatory approvals, mandates, or penalties—will we focus on the people we are supposed to be serving without turning first to medications.
Teepa Snow, STOP Treating Behaviors with Restraining Medications
The Omnibus Budget Reconciliation Act of 1987 (OBRA 87) established a resident’s right to be free of physical or chemical restraints in nursing homes when used for the purpose of discipline or convenience and when not required to treat the resident’s medical symptoms. Uncooperativeness, restlessness, wandering, or unsociability are not sufficient reasons to justify the use of a restraint (GovTrack, 2020).
A facility must ensure that the resident is free from physical or chemical restraints imposed for purposes of discipline or convenience and that are not required to treat the resident's medical symptoms. When the use of restraints is indicated, the facility must use the least restrictive alternative for the least amount of time and document ongoing re-evaluation of the need for restraints. A facility must not use verbal, mental, sexual, or physical abuse, corporal punishment, or involuntary seclusion (FL Statutes, 2024).
The use of a restraint must include care planning, staff monitoring, and periodic review by a physician. The use of chemical restraints is limited to prescribed dosages of medications authorized by the resident’s physician and must be consistent with the resident’s diagnosis. Residents who are receiving medications that can serve as chemical restraints must be evaluated by their physician at least annually to assess (FL Statutes, 2024):
- the continued need for the medication
- the level of the medication in the resident’s blood
- the need for adjustments in the prescription
A patient assessment is used to determine whether the use of less restrictive measures poses a greater risk than the risk of using a restraint. The comprehensive assessment should identify medical problems that may be causing behavior changes. For example, temperature elevations, hypoxia (low levels of oxygen), hypoglycemia (low blood sugar), electrolyte imbalances, drug interactions, and drug side effects may cause confusion, agitation, and combative behaviors. Addressing these medical issues may eliminate or minimize the need for the use of restraints or seclusion (FL Statutes, 2024).
2.4.1 Physical Restraints
A physical restraint is any manual method, physical or mechanical device, material, or equipment attached to or adjacent to a person’s body that the individual cannot remove easily and which restricts freedom of movement or normal access to one’s body. Forced isolation (such as locking a person in their bedroom), threats, using force, or restricting a person’s movement are also a type of restraint.
Physical restraints can include:
- belts
- mittens
- soft wrist and ankle restraints
- vest and jacket restraints
- bedrails
- geriatric chairs and recliners
- wheelchair safety bars
- lapboards
Use of physical restraints often causes agitation, confusion, and can lead to deconditioning, pressure ulcers, strangulation, and even death. Restraints affect a person’s sense of well-being, causing feelings of low self-worth, depression, withdrawal, humiliation, and anger.
Restraints are often applied without understanding their risks. Bed rails prevent falls but can trap a person trying to get out of bed, especially for a person living with dementia. Restraint belts secure a person to a chair or bed but often cause discomfort, helplessness, agitation, and anxiety. Restraint belts can also lead to severe complications such as pressure ulcers or impaired circulation if not monitored correctly. Fixed seating devices provide support but can restrict mobility and independence (Tao et al., 2025).
Restraints should not be considered a routine part of a falls-prevention program. There is no evidence that the use of physical restraints (including raised side rails) will prevent or reduce falls. Additionally, falls that occur while a person is physically restrained often result in more severe injuries. In fact, in some instances reducing the use of physical restraints decreases the risk of falling (CMS.gov, 2024).
2.4.2 Chemical Restraints
The term chemical restraint refers to the use of antipsychotic, antianxiety, antidepressant, or sedative medications for the purpose of controlling or restricting a person’s behavior or movement. Unfortunately, a decrease in the use of physical restraints has been linked to the increased use of chemical restraints (Cain et al., 2023).
In 2023, the American Geriatrics Society Beers Criteria for Potentially Inappropriate Medication Use in Older Adults stressed the need to avoid antipsychotics and other medications for behavioral problems of dementia and delirium because their use is frequently associated with harm (AGS, 2023).
Between 2011 and 2019, psychotropic drugs* were prescribed to about 80% of nursing home residents. Higher use of psychotropic drugs was associated with nursing homes with lower ratios of registered nurse staff to residents. Nursing homes with a higher percentage of low-income residents were also associated with higher use of these drugs (OIS, 2022).
*Psychotropic drugs: antipsychotics, anticonvulsants, mood stabilizers, and central nervous system agents.
Behavioral interventions are the preferred management strategy for treatment of challenging behaviors associated with dementia. The decision to use or not use a chemical restraint should always be made in collaboration with the patient and family members (AGS, 2023).
A provider may choose to prescribe an antipsychotic medication when symptoms are severe, dangerous, or cause significant distress to the patient. These medications may be effective in some cases. However, the provider must disclose to the patient and family that the medication is being used off label* meaning a drug has not been approved by the Food and Drug Administration (FDA) for treatment of behavioral symptoms of dementia. The provider must obtain permission from the patient or family member to use these drugs for behavioral symptoms of dementia.
*Off label: prescribing medications for an unapproved indication, age group, dose, or form of administration.
2.4.3 Alternatives to Restraints
There are many alternatives to the use of physical and chemical restraints. Some alternatives enhance safety and comfort for all residents, such as increasing staffing levels, removing hazards, providing safe areas for walking, and training staff on how to identify and respond to unmet needs (CANHR, 2025).
Other alternatives include adapting and tailoring chairs to improve comfort and safety, using pads and pillows to support comfortable and safe body positions, providing therapy and restorative care to improve a resident’s ability to move about safely, adjusting care and caregiver assignments to a resident’s preferences, and using low beds and floor padding to safeguard against harmful falls from bed (CANHR, 2025).
Establishing a routine, including a toileting schedule, prevents mad dashes to the bathroom that increase the risk of falls. Regular exercise, a comfortable place to rest, and a schedule for napping can also help. On a regular basis:
- Address hunger, thirst, and discomfort.
- Review medications for adverse effects.
- Treat all underlying causes, including pain.
- Assess hearing and vision.
- Relieve impaction.
An uncluttered environment can reduce the need for physical restraints. Hallways, common areas, and resident rooms should be free of equipment and obstacles. Providing wall rails, grab bars, and transfer poles in rooms, bathrooms, hallways, and common areas promotes independence reduces caregiver stress and worry.


Transfer poles and grab bars support independence and safety. Source: Author.

A seated walker with large wheels and a wide base. Source: Author.
Wheeled walkers with a wide base, easy-to-use brakes, and built in seats provide a safe place to rest. If a person uses a wheelchair to get around, most chairs can be lowered so a person can easily propel the chair with their feet. Wheelchair seating systems provide pressure reduction and postural support.
Restraint-reduction programs can greatly reduce the use of physical restraints. As with managing challenging behaviors, the best ideas are those that are shared among staff and family.
