Client Education
Asthma self-management education provides clients with the skills necessary to control asthma and improve outcomes; it should be integrated into all aspects of asthma care and it requires repetition and reinforcement. To be effective, asthma education should:
- Begin at the time of diagnosis and continue through followup care.
- Involve all members of the healthcare team.
- Introduce, assess, and reinforce key concepts for control at every visit.
Negotiate agreements about the goals of treatment, specific medications, and the actions clients will take to reach the agreed-upon goals to control asthma.
A team approach to care is a useful technique for delivering health education. Recent studies have focused on the use of specially trained nurse educators to provide asthma education. Three randomized controlled trials (RCT) and three observational studies used advanced practice nurses trained in asthma care to deliver self-management education to adults in outpatient settings.
In one RCT, a hospital-based nurse specialist delivered self-management education during three sessions (Levy et al., 2000). Compared to clients receiving usual care, the educated clients significantly increased use of ICS for control, decreased need for SABA for rescue, achieved higher mean and less variable PEF, and had significantly lower symptom scores, doctor visits, and urgent care visits for asthma after 6 months. The reduction in asthma morbidity in this study may have been related to the strong emphasis, during the educational sessions, placed on improving asthma self-management skills during exacerbations.
In another RCT, self-management education with peak flow monitoring and a written asthma action plan—individualized to the client’s severity—was delivered in one session that was then reinforced in two subsequent visits (Janson et al., 2003). Compared to the control condition (monitoring only), self-management education significantly improved adherence to ICS medications, quality of life, and perceived control of asthma.
In an attempt to reduce high hospitalization rates and healthcare utilization, yet another RCT (Urek et al., 2005) examined the effectiveness of three educational interventions in adults: asthma school, an educational booklet, and individual verbal instruction. Asthma school, which included three 4-hour sessions of group education, produced the most significant improvement in quality of life, while individual verbal instruction produced the best overall response in terms of both asthma control and quality of life.
Hopman and colleagues (2004) used nurse specialists to educate children and adults who had asthma through a standardized 2-hour asthma education program given across seven clinical centers in a large, multi-site observational study. The program resulted in significant improvements (decreases) in hospital utilization and missed activity days over 6 months. Two other observational studies of adults who had asthma, in which clients were taught and cared for by specially trained asthma nurses (Lindberg et al., 2002), showed significantly reduced symptoms and days of activity limitation as well as significantly decreased markers of airway inflammation (Janson et al., 2001).
Respiratory therapists also provide asthma education in hospital, emergency department, and clinic settings, and may direct clinical pathways and algorithms in hospital settings. An observational trial of 60 pediatric clients who attended a special clinic focusing on inhaler technique demonstrated that MDI technique improved significantly after MDI demonstration, teaching, and reinforcement (Minai et al., 2004). Respiratory therapists also participate actively in clinical protocols or pathways that are implemented in acute care settings for management of acute exacerbations in hospitalized clients.
Pharmacists also have a role in client education and are in a unique position to advise both clients and clinicians when medication use is exceeding standard recommendations. They may also reinforce the need for a client to have a “clinical home” with a single provider or primary clinician directing care, even though this may involve use of specialists, for severe cases, and other members of the healthcare team to deliver specific components of care.
The primary goal in asthma care is to manage symptoms using the minimal amount of medication necessary to achieve good symptom control while avoiding adverse effects. In order to achieve this goal both the clinician and client must be in agreement regarding the client’s asthma control. Clients often do not understand or have sufficient awareness of their symptoms until they have experienced significant deterioration in their symptoms to the point that they require either emergency department care or hospitalization. Aside from the risks inherent in a severe exacerbation of asthma symptoms, the client is also potentially exposed to invasion by more serious pathogens when receiving hospital-based care.
Once the diagnosis of asthma has been confirmed, early education includes teaching regarding:
- Basic facts about asthma
- What defines well-controlled asthma and the client’s current level of control
- Roles of medications
- Skills (eg, inhaler technique, use of a valved holding chamber [VHC] or spacer)
- Self-monitoring
- When and how to handle signs and symptoms of worsening asthma
- When and where to seek care
- Environmental exposure control measures
Ongoing discussion about client perception of symptom control reinforces the need for clients to become the experts for their particular disease status. This allows the healthcare team to uncover discrepancies between objective measures of the client’s status and clients’ self-report of symptoms. Clients and their families should always be given support and positive reinforcement for changes they make in any of the variables that affect the course of the disease, even if these measures only party address desirable changes. With open communication established, the likelihood increases that the client will be a reliable and accurate reporter of all aspects that influence home management.
A further consideration in creating effective partnerships for care is inclusion of the client, parent, or caretaker in decision-making about asthma and asthma treatment, and identifying preferences and barriers to effective treatment. If clinicians and clients have different treatment goals, the partnership aspect of care is unlikely to succeed, with a decrease in satisfaction or an increase in frustration experienced by both parties, to the benefit of neither.
Choosing a treatment regimen that improves outcomes and addresses preferences that are important to the client and caregiver encourages adherence to the plan of care. However, education that provides information only—without skills training—improves knowledge but does not reduce hospitalizations, ED visits, unscheduled doctor’s visits, or lost work days. Nor does it improve lung function and medication use, which should be the focus of care. Therefore, a written asthma treatment plan is the best method for ensuring that both the client and clinician are clearly in agreement about treatment goals and the means to achieve them.
Reviewing the success of the treatment plan with the client or caregiver at each visit and making adjustments as needed allows clients to experience increased confidence in their ability to participate in management of their disease. Self-monitoring may be about recognizing symptom severity or it may be based on peak flow readings as part of a written asthma treatment plan.
Several standardized forms are available with a simple, yet comprehensive, set of instructions that enable the client to make decisions based on daily self-monitoring and provide criteria for recognizing and handling worsening asthma, including need for assistance. Written asthma action plans are particularly recommended for clients who have moderate or severe persistent asthma, a history of severe exacerbations, or poorly controlled asthma.
When self-management is the chosen method for maintaining asthma control, peak-flow-based is equivalent to symptom-based self-management, so long as there is a written plan with instructions on how to recognize and handle worsening asthma that includes self-adjustment of medications and followup guidelines.
Peak Flow Meters
A peak flow meter is a device that measures how well air moves out of lungs. During an asthma episode the airways of the lungs slowly begin to narrow. The peak flow meter may signal narrowing in the airways hours and sometimes even days before the client experiences any worsening of symptoms.
Peak flow meters are most helpful for clients who have to take medications every day. Clients are taught to use their peak flow meters to:
- Learn what makes their asthma worse (eg, triggers, environmental factors)
- Determine if their treatment plan is working well
- Decide when to add or stop medicine
- Decide when to seek emergency care
Two Peak Flow Meters
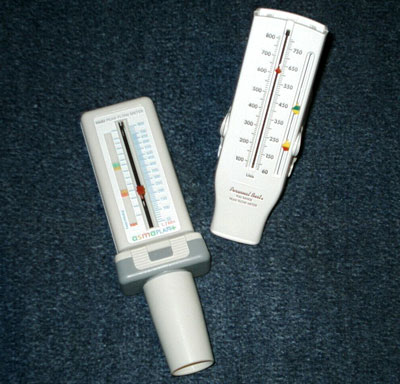
Source: Wikipedia Commons.
A “personal best” reading is needed to establish baseline. This differs from client to client depending on severity of the disease. During the two-week window when personal best is being calculated, the client checks by taking the following steps:
- Move the indicator (red arrow) to the bottom of the numbered scale.
- Stand up.
- Take a deep breath, filling the lungs completely.
- Place the mouthpiece in your mouth and close your lips around it. Do not block the hole with your tongue.
- Blow out as hard and fast as you can in a single blow.
Repeat steps 1 thru 5 for a total of three times and record the best of the three. Readings should be taken 2 to 3 times a day for two weeks with at least one rising and one afternoon reading. If a dose of SABA is taken, a measurement should be made 15 minutes later. Once a personal best is obtained, the client is instructed to add medications as indicated on the written plan.
Various standardized forms are available as templates for the asthma action plan. Some are free and can be reproduced free of charge. One example of such a form is available through the NIH at https://www.nhlbi.nih.gov/files/docs/public/lung/asthma_actplan.pdf.
The client is given medication instructions based on whether their readings place them in the “green” zone (80% of personal best) with additional instructions if the readings fall into the “yellow” (50%–79%) or “red” (below 50%) zones. The form may have additional instructions regarding trigger avoidance as well as emergency help instructions.
Correctly used, information and management based on a peak flow meter can be effective in helping the client to identify early declines in pulmonary functioning—but it is not necessarily superior to symptom based self-monitoring strategies, especially if the client is not compliant due to the time necessary to implement peak flow.
Symptom Based Self-Assessment
An additional method of self-management depends on the client’s ability to ascertain changes in respiratory status. This is typically done using some sort of validated questionnaire that quantifies symptoms experienced both initially and at follow-up visits.
Initial assessment includes questions designed to elicit the following history:
- In the past four weeks, how much work, school, ADLs missed due to symptoms?
- In the past four weeks, how many nights awakened due to cough, symptoms?
- Do you believe your asthma is well controlled?
- What was the highest number of puffs on your SABA per day in the past four weeks?
A number is assigned and the client is then given a written asthma action plan based on symptoms. Examples of validated instruments that can be used for symptom-based management include:
- Asthma Control Questionnaire (Juniper et al., 1999)
- Asthma Therapy Assessment Questionnaire ( Vollmer et al., 1999)
- Asthma Control Test (Nathan et al., 2004)
- Asthma Control score (Boulet et al., 2002)
These can also be viewed by going to the NIH website referenced above.
Additional Considerations to Reinforce Partnership
As already noted, whether peak flow monitoring or the symptom based self-assessment is used to quantify symptoms, a written asthma plan must be provided with specific instructions regarding medication changes, trigger avoidance, and emergency measures.
To educate effectively, the healthcare team must be aware that assumptions regarding the client’s literacy status can lead to misunderstandings that do little to promote good symptom control. Literacy can refer both spoken and written instructions. Providers should use simple and direct language to elicit information from clients at each visit, avoiding words understood only by the medical professional.
In general, written instructions can be assumed to be understandable if they are written at a fifth-grade level, but this varies depending on cultural and developmental factors; however, even if the literacy level appears to be lower than fifth grade, the client can still be educated. Using pictures and demonstration with return demonstration can also be highly effective. Group teaching sessions may be appropriate for some individuals and have an added benefit of providing peer support.
Regardless of which methodology is used, the partnership will be more effective and mutually satisfying if the clinician remembers to start each visit by asking the client or caretaker what specific concerns and/or goals they would like addressed. In the course of the visit further emphasis is given to asthma control, overall treatment goals, medications being used, and quality of life.
The partnership aspect of care, which is client-focused and addresses client responsibility as an active team member, is also reinforced by asking such questions as:
- What worries you most about your asthma?
- What do you want to do that you can’t now because of symptoms?
- What improvement do you expect from medications?
Use of questions that focus specifically on client concerns is effective in emphasizing the need for clients to have continual awareness of the ways their life is being affected by asthma and thus to increase their willingness to adhere to the comprehensive plan of care.
Evidence is now abundant that asthma self-management education is effective in improving outcomes of chronic asthma. Specific training in self-management skills is necessary to produce behavior that modifies the outcomes of chronic illnesses such as asthma. Expert care, with regular review by health professionals, is necessary but not sufficient to improve outcomes. Clients must actively participate in their own care, which means consciously using strategies and taking actions to minimize exposure to factors that make asthma harder to control and adjusting treatments to improve disease control.
The ultimate goal of both expert care and client self-management is to reduce the impact of asthma on related morbidity, functional ability, and quality of life. The benefits of educating people who have asthma in the self-management skills of self-assessment, use of medications, and actions to prevent or control exacerbations, include reduction in urgent care visits and hospitalizations, reduction of asthma-related healthcare costs, and improvement in health status.
When our client Tom was seen for an unscheduled followup visit close to the time of his initial diagnosis, he was overusing his SABA to control symptoms related to environmental exposures. After becoming more knowledgeable about medications and the Step approach to managing medications, you determined that elimination of all triggers was not practical. You spoke to the primary care clinician about alternative approaches to treatment for Tom’s symptoms, which have been classified as moderate-persistent. With Tom’s participation and agreement, his medication was changed to a combined product containing ICS and LABA in the form of fluticasone/salmeterol.
Knowing that it would be a while before he could expect any degree of remission of cat dander allergy from the immunotherapy, Tom agreed to be extremely observant of measures to control his exposure to this particular allergen. Tom’s roommate has agreed to restrict the cat’s access only to areas not used communally. You have scheduled Tom to come to the office to focus on educational aspects of care to promote his ongoing ability to self-manage his symptoms. Being a student, he is eager to participate, especially as he wants to make sure he can continue to enjoy his school and social life. Therefore you plan on tailoring your educational interventions to include the following concepts in care.
Test Your Knowledge
When asthma has been diagnosed, education focuses on the following:
- The client’s primary responsibility for ensuring a positive outcome.
- The client’s becoming comfortable with handing over control to professionals.
- Basic facts about asthma, definition of control, role of medication, and self-monitoring.
- Differential diagnosis, need to manage co-morbidity, client’s use of the step approach to manage their own medications.
The best approach to ensure client adherence to treatment recommendations for asthma emphasizes the:
- eed for members of the healthcare team to take a primary role in monitoring client use of medications.
- Use of a partnership approach with an emphasis on support and effective communication to reinforce the client’s role as a team member.
- Need for the primary clinician to assign clear boundaries about the kinds of education delivered wherever the client might be seen.
- Need to turn most decision making regarding treatment over to the client.
Of the strategies available to promote client awareness of their symptoms, which of the following statements is true?
- The peak flow method is preferred because it is easy to use and provides objective data.
- A validated symptom-based self-management strategy is best because it makes clients responsible for managing their symptoms.
- Neither peak flow monitoring nor symptom-based self-management are effective because most clients don’t understand them.
- Either peak flow or symptom-based self-management can be used, but they must be accompanied by a written asthma plan.
A written asthma action plan is a necessary adjunct to client education because it:
- Prevents the client from over-utilizing office staff time asking questions.
- Clarifies measures to be taken at each level of severity, including the need for additional or emergency assessment.
- Lets the client know how poor their symptom control is.
- Reinforces that clients are capable of managing their symptoms with little help.
Answers: C,B,D,D
Tom elects to use a combination of a peak flow meter and his written asthma plan. He appreciates the acknowledgement needs will result in the best degree of symptom management. He reports that improved management of exposure to triggers, especially cat dander, along with the change in his medication, and in lifestyle to control his GERD, has resulted in his needing his SABA only once in the last month.
Tom understands that he must have symptom control at the same level for at least three months before a step down in his medication will be considered. He is able to demonstrate appropriate use of his MDI and verbalizes good understanding of changes to his therapy, including the possible need for additional intervention, outlined on his asthma action plan, should his symptoms become less stable. In summary, he has been an ideal client, the likes of which may never be seen again!
