Cause of HIV
HIV Virus
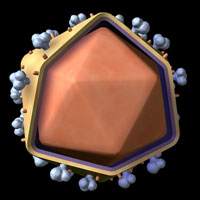
The physical structure of HIV is characterized by a protein shell encapsulating the genetic information and enzymes of the virus; a lipid membrane that circles the protein capsule; and glycoproteins that dot the surface of the virus, which aid in processes such as entry into macrophages and T-helper cells of the host. Illustration provided by 3DScience.com.
The human immunodeficiency virus kills or impairs the cells of the immune system and progressively destroys the body’s ability to protect itself. Over time, a person with a deficient immune system (immunodeficiency) may become vulnerable to infections by disease-causing organisms such as bacteria or viruses. These infections can become life-threatening.
The term AIDS stands for “acquired immunodeficiency syndrome,” and it refers only to the most advanced stage of HIV infection. Medical treatment can delay the onset of AIDS, but HIV infection eventually results in a syndrome (combination) of symptoms, diseases, and infections. The diagnosis of AIDS requires evidence of HIV infection and the appearance of some specific additional conditions or diseases. Only a licensed medical provider can make an AIDS diagnosis.
Surveillance Case Definitions (rev. 2008)
In December 2008, the Centers for Disease Control and Prevention (CDC) published Revised Surveillance Case Definitions for HIV Infection Among Adults, Adolescents, and Children Aged <18 Months and for HIV Infection and AIDS Among Children Aged 18 Months to <13 Years.
For adults and adolescents (people 13 years or older), the surveillance case definitions for HIV infection and AIDS were revised into a single case definition that includes AIDS and incorporates a system for staging HIV-infection. In addition, the HIV case definition for children over 13 years old and the AIDS definition for children aged 18 months to 13 years were revised.
No changes were made to the HIV classification system, the 24 AIDS-defining conditions for children older than 13 years, or the AIDS definition for children over 18 months of age (CDC 2013, CDC 2008).
A confirmed case meets the laboratory criteria for diagnosis of HIV infection and one of the four HIV infection stages (stage 1, stage 2, stage 3, or stage unknown).
- HIV infection, stage 1: No AIDS-defining condition and either CD4+ T-lymphocyte count of ≥500 cells/µL or CD4+ T-lymphocyte percentage of total lymphocytes of ≥29.
- HIV infection, stage 2: No AIDS-defining condition and either CD4+ T-lymphocyte count of 200–499 cells/µL or CD4+ T-lymphocyte percentage of total lymphocytes of 14–28.
- HIV infection, stage 3 (AIDS): CD4+ T-lymphocyte count of <200 cells/µL or CD4+ T-lymphocyte percentage of total lymphocytes of <14, or documentation of an AIDS-defining condition. Documentation of an AIDS-defining condition supersedes the laboratory definitions here.
- HIV infection, stage unknown: No information available on CD4+ T-lymphocyte count or percentage and no information available on AIDS-defining conditions (CDC 2013, CDC 2008)
AIDS-Defining Conditions
- Bacterial infections, multiple or recurrent*
- Candidiasis of bronchi, trachea, or lungs
- Candidiasis of esophagus†
- Cervical cancer, invasive§
- Coccidioidomycosis, disseminated or extrapulmonary
- Cryptococcosis, extrapulmonary
- Cryptosporidiosis, chronic intestinal (>1 month’s duration)
- Cytomegalovirus disease (other than liver, spleen, or nodes), onset at age >1 month
- Cytomegalovirus retinitis (with loss of vision)†
- Encephalopathy, HIV related
- Herpes simplex: chronic ulcers (>1 month’s duration) or bronchitis, pneumonitis, or esophagitis (onset at age >1 month)
- Histoplasmosis, disseminated or extrapulmonary
- Isosporiasis, chronic intestinal (>1 month’s duration)
- Kaposi sarcoma†
- Lymphoid interstitial pneumonia or pulmonary lymphoid hyperplasia complex*†
- Lymphoma, Burkitt (or equivalent term)
- Lymphoma, immunoblastic (or equivalent term)
- Lymphoma, primary, of brain
- Mycobacterium avium complex or Mycobacterium kansasii, disseminated or extrapulmonary†
- Mycobacterium tuberculosis of any site, pulmonary,†§ disseminated,† or extrapulmonary†
- Mycobacterium, other species or unidentified species, disseminated† or extrapulmonary†
- Pneumocystis jirovecii pneumonia†
- Pneumonia, recurrent†§
- Progressive multifocal leukoencephalopathy
- Salmonella septicemia, recurrent
- Toxoplasmosis of brain, onset at age >1 month†
- Wasting syndrome attributed to HIV
* Only among children aged <13 years. (CDC. 1994 Revised classification system for human immunodeficiency virus infection in children less than 13 years of age. MMWR 1994;43[No. RR-12].)
† Condition that might be diagnosed presumptively.
§ Only among adults and adolescents aged >13 years. (CDC. 1993 Revised classification system for HIV infection and expanded surveillance case definition for AIDS among adolescents and adults. MMWR 1992;41[No. RR-17].)
Source: CDC, 2008.
HIV enters the bloodstream and seeks out T-helper lymphocytes, white blood cells essential to the functioning of the immune system. One of the functions of these cells is to regulate the immune response in the event of attack from disease-causing organisms such as bacteria or viruses. When the virus infects the T-helper lymphocyte, the cell sends signals to other cells, which produce antibodies. This T-helper lymphocyte cell is also called the T4 or the CD4 cell.
HIV Entry into T Cell
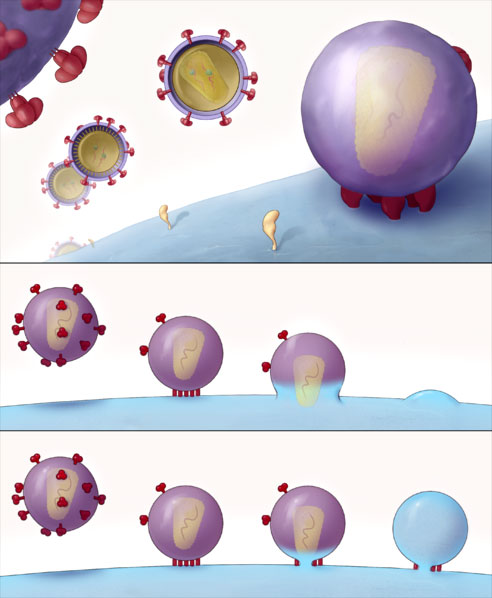
The top panel shows the HIV virion finding and attaching to a T cell. The second and third panels show HIV viruses (dotted with red glycoproteins) attaching to the T cell and depositing the HIV virus particle into it. Source: Image courtesy of Sougrat et al., 2007; PLoS Creative Commons Attribution 2.5 license.
A person with untreated HIV infection experiences several stages of infection:
- Viral transmission
- Primary HIV infection—lasting 1 to 2 weeks as the virus establishes itself in the body.
- Seroconversion—the point when antibodies to the HIV virus produced by the immune system are able to be identified by laboratory test.
- Asymptomatic HIV infection—a person is infectious but looks and feels healthy. The virus is active and continuing to damage the immune system.
- Symptomatic HIV infection—symptoms such as skin rash, night sweats, mouth ulcers, weight loss, and fungal infections appear.
- AIDS—the CDC defines AIDS as an HIV-positive person who has a CD4+ T-lymphocyte count of <200 cells/µL or CD4+ T-lymphocyte percentage of total lymphocytes of <14, or documentation of an “AIDS-defining condition.”
These stages are sometimes called the “natural history” of disease progression. The natural history of HIV infection has been altered dramatically in developed countries because of new medications. In countries where there is no access to these expensive medications, or in cases where people do not become aware of their HIV infection until very late, the disease progresses as described above (WSDOH, 2007).
HIV is a relatively fragile virus, which is not spread by casual contact. HIV is not easy to “catch”—it must be acquired. In order for HIV to be transmitted, there must be:
- An HIV source.
- A sufficient dose of virus.
- Access to the bloodstream of another person.
One of the predictors of the infectious level of an HIV-positive person is viral load—how much HIV is present in the bloodstream. Studies show a clear connection between higher viral load in the blood and increased transmissibility of HIV.
HIV is transmitted through:
- Unprotected anal, vaginal, and oral intercourse
- Sharing needles or other injection equipment
- A mother passing the virus to her baby either before or during birth
- An infected woman breastfeeding her infant
- Accidental needlestick injuries, or infected body fluid coming into contact with the broken skin or mucous membranes of another person (as with healthcare workers)
- A transfusion prior to 1986 of HIV-infected blood or blood products
In extremely rare cases, HIV can be transmitted by sharing razors or toothbrushes, if infected blood from one person was deposited on the toothbrush or razor and the blood entered the bloodstream of another person.
In settings such as hospital operating rooms, other fluids—cerebrospinal fluid, synovial fluid, pleural fluid, pericardial fluid, amniotic fluid—may be considered infectious if the source is HIV-positive. These fluids are generally not found outside the hospital setting. Therefore, the most common body fluids considered potentially infectious for HIV are blood, semen, vaginal secretions, and breast milk.
HIV transmission may occur during practices such as tattooing, blood-sharing activities such as “blood brother” rituals or any other type of ritualistic ceremonies where blood is exchanged, or when unsterilized equipment contaminated with blood is shared. HIV transmission may also occur in occupational settings.
People Unaware of Their Positive Status
People who are infected with HIV come from all races, countries, sexual orientations, genders, and income levels. Globally, most of the people who are infected with HIV have not been tested and are unaware that they are living with the virus. The CDC estimates that, in 2009, 18% of those in the United States who had HIV were unaware that they were living with the virus. This is a decline from the 25% measured in 2003 and is a positive sign because research shows that most individuals who know they are infected with HIV will reduce behaviors that could transmit the virus (CDCNPIN, 2012).
It is important to note that the great majority of people with HIV infection do not transmit HIV to others. The CDC estimates that in 2006 there were 5 transmissions per 100 persons living with HIV infection. This means that at least 95% of those living with HIV infection did not transmit the virus to others that year. This represents an 89% decline in the estimated rate of transmission since the peak level of new infections in the mid-1980s. It is believed that the decline is due to effective prevention efforts and the availability of improved testing and treatments for HIV (CDCNPIN, 2012).
Pregnant Women
An HIV-infected woman may transmit the virus to her baby during pregnancy, during the birth process, or following pregnancy by breastfeeding. One of the predictors of how infectious the woman will be to her baby is her viral load (how much HIV is present in her bloodstream). Women with new or recent infections or people in later stages of AIDS tend to have higher viral loads and may be more infectious.
HIV is transmitted from an HIV-infected woman to her baby in about 25% of pregnancies if intervention with antiretroviral medications does not occur. The perinatal transmission rate has dropped dramatically in the United States due to the widespread use of AZT by HIV-infected pregnant women. When a woman’s health is monitored closely and she receives a combination of antiretroviral therapies during pregnancy, the risk of HIV transmission to the newborn drops below 2%.
In some pregnancies, cesarean section (C-section) may be recommended to reduce the risk of transmission from woman to baby. Advice about medications and C-section should be given on an individual basis by a medical provider with experience in treating HIV-positive pregnant women. Most states, including Florida, require pregnant women to be counseled regarding risks around HIV and offered voluntary HIV testing.
