The Statistics
Severe sepsis is unfortunately common, expensive, and frequently fatal. More than 750,000 cases of sepsis occur annually in the United States, and its incidence continues to rise. The growth of the number of cases of sepsis is more than the growth of the U.S. population. Between the late 1970s and today, the American population increased by 35%; in the same period, the number of cases of sepsis increased by more than 350% (CDC, 2010). It has been estimated that between 28% and 50% of these people die—far more than the number of U.S. deaths from prostate cancer, breast cancer, and AIDS combined (NIGMS, 2013).
The increasing number of sepsis cases in the United States may be due to:
- An aging population
- The increased longevity of people with chronic diseases
- Greater use of invasive procedures which introduce microorganisms into the body
- Broader use of immunosuppressive drugs, chemotherapy, and transplantation
- The spread of antibiotic-resistant organisms
- Improved clinical awareness and diagnosis of sepsis
(NIGMS, 2013)
More than half of all patients diagnosed with severe sepsis are treated in an intensive care unit (ICU) and sepsis is one of the most common reasons for admission to ICUs throughout the world. In the United States, 2% to 3% of the hospitalized patients have severe sepsis, but those patients account for 20% of the hospitals’ ICU admissions (CDC, 2010).
During the past two decades, the incidence of sepsis in the United States has tripled and is now the tenth leading cause of death. In the United States alone, approximately 750,000 cases of sepsis occur each year and at least 225,000 (1/3) are fatal. Septic patients are generally hospitalized for extended periods, rarely leaving the ICU before 2 to 3 weeks. Despite the use of antimicrobial agents and advanced life support, the case fatality rate for patients with sepsis has remained between 20% and 30% during the past two decades (Marik, 2011).
The average sepsis survivor has received between 7 and 14 days of ICU care followed by an additional 10 to 14 days of hospitalization. In 2009 this care costs more than $22,000 per patient, and nationwide the cost was $17 billion. The national costs of sepsis are similar to the national costs of ischemic heart disease (coronary artery disease) (CDC, 2010; Lagu et al., 2011).
While the number of cases of sepsis is increasing, the mortality rate is declining due to improvements in early diagnosis and effective treatments. Nonetheless, the death rate is still very high. Approximately 1 of every 4 patients with severe sepsis and 1 of every 2 patients with septic shock will die within 30 days of their diagnosis. Overall, sepsis contributes to almost 30% of all U.S. deaths and almost 40% of the deaths of Americans older than 85 years (Munford, 2008; CDC, 2010).
Test Your Knowledge
The increase in the number of sepsis cases may be due to:
- Recent changes in the definition of sepsis.
- An increase in international travel.
- Greater use of invasive medical procedures.
- Increases in sexually transmitted diseases.
Apply Your Knowledge
Q: If sepsis is the tenth leading cause of death, what are the first two most common causes of mortality in the United States?
A: cardiovascular disease, cancer and medication errors (CDC, 2016).
Answer: C
Susceptible Populations
Anyone at any age can get sepsis, but it is more common in infants, elders, and those who are ill or weakened. About 2 of every 3 patients who develop sepsis already have another significant illness. It can be caused by simple infection such as an insect bite, urinary tract infection, or pneumonia. People with chronic health conditions such as diabetes, cancer, kidney and liver disease; those with suppressed immune systems (from chemotherapy, AIDS, long-term steroid use); and patients with implanted devices or endotracheal tubes are at increased risk of developing sepsis (Neviere, 2013a). A recent study reported that septic shock is the most common cause of death in noncoronary intensive care units, and the tenth leading cause of death overall in high-income countries (Schulte et al., 2013).
Test Your Knowledge
Sepsis tends to strike:
- Unsuspecting healthy young adults.
- Infants and elders.
- Overweight middle-aged adults.
- Pet owners.
Apply Your Knowledge
What nursing actions can you do to decrease the risk of infection in your facility? How well do you don and take off isolation gowns/gloves between patients? How well do you wash your hands between patients? What special bundles are you using for ventilated patients (eg, VAP protocol)?
Answer: B
Incidence and mortality from sepsis increase with a patient’s age. Two-thirds of the patients who develop severe sepsis are older than 65 years, and the likelihood of getting sepsis increases dramatically thereafter.
U.S. Hospitalizations for Sepsis by Age Group (2000–2007)
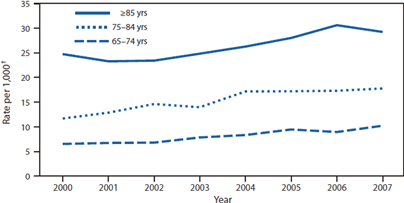
Hospitalizations per 1000 Americans for sepsis in three different age groups, during the years 2000 to 2007. Comparing the three lines, the risk of getting sepsis increases with age: people older than 85 years are 5 times more likely to be hospitalized for sepsis than are people aged 65–74 years. Source: CDC, 2010.
The Surviving Sepsis Campaign
Because of the high incidence of sepsis and poor clinical outcomes, national and worldwide healthcare systems have petitioned for guidelines. The Surviving Sepsis Campaign (SSC) is a global effort to improve the care of patients with severe sepsis and septic shock. The campaign was launched in 2002 by the Society of Critical Care Medicine, the European Society of Intensive Care Medicine, and the International Sepsis Forum, with their latest update in 2015. The objective of the campaign was to develop and disseminate evidence-based guidelines so that the knowledge obtained from clinical trials could be applied to bedside practice. The goal was to reduce death from severe sepsis and septic shock by 25%.
Historically, invasive management and aggressive resuscitation of the septic patient occurred in the intensive care unit (ICU); however, sepsis is now recognized as an overwhelmingly time-critical disease, requiring early initiation of care in the emergency department (ED), with subsequent transfer to the ICU (Perman et al., 2012).
The Surviving Sepsis Campaign developed guidelines known as early goal directed therapy (EGDT) to increase sepsis awareness and to direct treatment. Recommendations are classified into three groups: (1) those directly targeting severe sepsis, (2) those targeting general care of the critically ill patient and considered high priority in severe sepsis, and (3) pediatric considerations. The guidelines are intended to be best practice guidelines and not definitive standards of care (Buckman, 2013). In addition, in 2015 the Centers for Medicare and Medicaid Services (CMS) presented a new inpatient reporting program called SEP-1, requiring hospitals to report the bundle measures to help hospital staff focus on these disease progression-halting measures (Schorr, 2016).
Treatment begins with 3-hour and 6-hour windows (bundles) involving the infusing of large quantities of intravenous crystalloid fluids, stabilizing ventilation and circulation, beginning diagnostic studies, administering antibiotics, and searching for the source of infection. When this initial work is done and patients have stabilized, they are given supportive critical care. If the patient has not improved or continues to deteriorate, treatment must be re-evaluated quickly. The average patient who has sepsis spends 2.5 to 4 weeks in a hospital. Even with experienced care, approximately 1 in 5 septic patients die. The mortality rate is worse for severe sepsis and for septic shock.
Although it has been shown that adherence to the EGDT protocol saves lives, consistent implementation has been challenging. Noncompliance with 3- and 6-hour sepsis bundles has been demonstrated to increase in-hospital mortality for septic patients, while compliance with the resuscitation bundle, even if extended from the recommended time frame, decreases mortality (LaRosa et al., 2012).
3-hour bundle
- Measure the patient’s lactate level.
- Obtain blood cultures before antibiotic administration.
- Administer broad-spectrum antibiotics.
- Administer 30 mL/kg crystalloid for hypotension or a serum lactate of 4 mmol/L or higher.
6-hour bundle
- Give vasopressors to keep MAP >65 mm Hg (if hypotension doesn’t respond to fluid resuscitation).
- Reassess volume status and tissue perfusion if hypotension persists and MAP is <65 mm Hg.
- Re-measure lactate level if the initial level was elevated.
Test Your Knowledge
The Surviving Sepsis Campaign developed guidelines known as early goal directed therapy (EGDT). Recommendations were classified into three groups. Which one of the following is not one of the groups?
- Those directly targeting severe sepsis.
- Those targeting general care of the critically ill patient with severe sepsis.
- Those targeting pediatric patients.
- Those targeting the elderly.
Apply Your Knowledge
Q: In our earlier scenario, what components of the 3- or 6-hour bundle actions were taken?
A: None of the 3-hour bundle recommendations were completed because the diagnosis was simple pneumonia. Due to the delay in arriving to a med/surg floor, the antibiotics were not started until 5 hours later and no blood culture was completed prior to the first dose.
Answer: D
