The ugly reality is that dementia often manifests as a relentless and cruel assault on personhood, comfort, and dignity. It siphons away control over thoughts and actions, control that we take for granted every waking second of every day.
Michael J. Passmore
Geriatric Psychiatrist, University of British Columbia
Brain disease comes in many different forms and has many different causes. Because the brain is so important, any damage to the brain can have a profound impact on our ability to manage daily affairs, communicate effectively, and live independently.
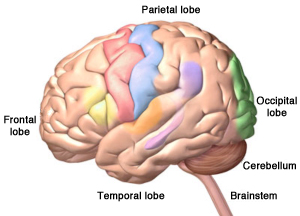
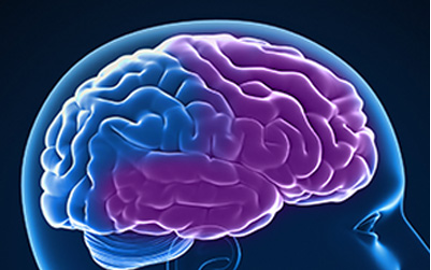
An illustration of the cerebrum, cerebellum, and the brainstem. The outer surface of the cerebrum is made up of a thin layer of nerve cells called the cerebral cortex. Source: Zygote Media. Used with Permission.
The largest part of the human brain, the cerebrum, has four lobes: the frontal, temporal, parietal, and occipital lobes. The most recognizable and devastating effects of dementia occur because of damage to nerve cells on the outer surface of the lobes—the cerebral cortex.
Common Types of Dementia
Dementia is a syndrome, a collection or grouping of symptoms—the result of progressive deterioration and loss of brain cells and brain mass. Different types of dementia affect different parts of the brain. Some dementias start in a part of the brain that controls a specific function such as short-term memory or emotion. Other dementias affect the entire brain—or more than one part of the brain—causing other symptoms.
Although a small percentage of people experience early-onset dementia, in general, dementia develops in later adulthood. Aging is a risk factor for developing dementia but nevertheless dementia is not considered a normal part of aging.
Although Alzheimer’s disease is the most common cause of dementia, it isn’t the only cause. Frontal-temporal dementia—which begins in the frontal lobes and accounts for 5-10% of dementias—is a relatively common type of dementia in those under the age of 60. Vascular dementia and Lewy body dementia are other common types of dementia (see table). Dementia associated with Parkinson’s disease shares a common etiology with Lewy body dementia.
In all, nearly twenty different types of non-Alzheimer’s dementia have been identified. Determining if someone has dementia is important because some types of cognitive decline may be treatable or even reversible if the underlying cause is identified and treated (Sönke, 2013).
Some Common Types of Dementia | |||
|---|---|---|---|
Dementia subtype |
Characteristic symptoms |
Neuropathology |
% of cases |
*Alzheimer’s disease (AD) |
|
|
60%–80% |
Frontal-temporal dementia |
|
|
5%–10%, prevalence thought to be underestimated |
*Vascular dementia |
|
|
20%–30% |
Dementia with Lewy bodies (closely related to Parkinson’s disease dementia) |
|
|
~5%-10% |
Did You Know. . .
For some time now, we have used the term “Alzheimer’s disease and related dementias” to describe dementia and to make it clear that there is more than one kind of dementia. The term neurocognitive disorder is now recognized in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) as a new term for dementia.
Alzheimer’s Dementia
Alzheimer’s disease (AD) is an irreversible, progressive, age-related brain disorder that affects as many as 5 million Americans age 65 and older. It is the most common type of dementia and is responsible for 60-80% of all cases. Worldwide, more than 50 million people live with dementia and because people are living longer this number is expected to triple by 2050 (ADI, 2019).
In Florida, there are 580,000 residents currently living with Alzheimer’s disease (Alzheimer’s Association, 2020a). By 2025, this number is expected to increase by more than 200,000.
Memory problems are a common early symptom of Alzheimer’s dementia although language difficulties, apathy, depression, and vision and spatial difficulties can also be early symptoms. Although more than twenty types of dementia have been identified, Alzheimer’s dementia is the most frequent (and most studied) cause of dementia in older adults. In general, executive functions are more impaired in Alzheimer’s disease than in other types of dementia.
Did You Know. . .
Worldwide more than 50 million people live with dementia and this number is expected to double by 2030 and triple by 2050.
The exact cause of Alzheimer’s dementia is still unknown. In Alzheimer’s disease, and likely in other forms of dementia, damage within the brain is thought to be due to the formation of beta-amyloid plaques, the formation of neurofibrillary tangles, and degeneration neurons in the cerebrum.
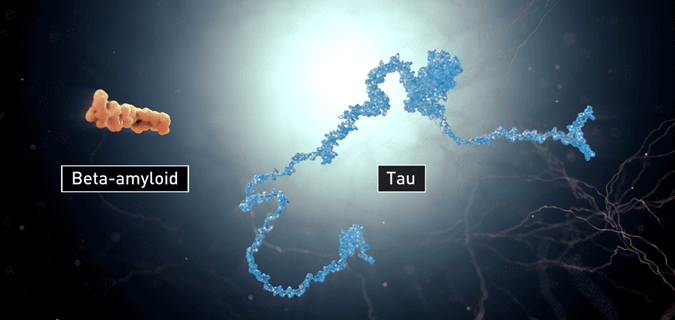
Beta-amyloid plaques and neurofibrillary tangles (tau). Source: Image courtesy of the National Institute on Aging/National Institutes of Health.
Brain imaging techniques such as MRIs as well as autopsies show that Alzheimer’s causes the brain to shrink, that connections between nerves weaken and nerve cells are damaged and lost. Once a healthy nerve cell begins to deteriorate, it loses its ability to communicate with other neurons, with devastating results.
Degeneration of Cerebral Neurons
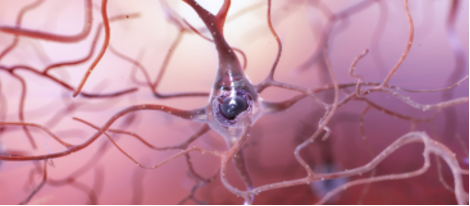
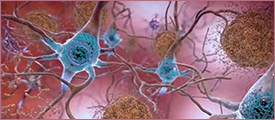
Left: A healthy neuron with many connections to other cells. Right: A dying nerve cell showing the nerve connections weakening and the main body of the cell deteriorating due to the presence of amyloid plaques and tau tangles. Source: Image courtesy of the National Institute on Aging/National Institutes of Health.
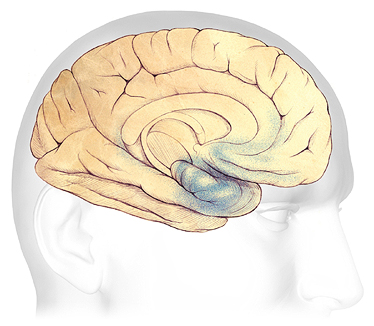
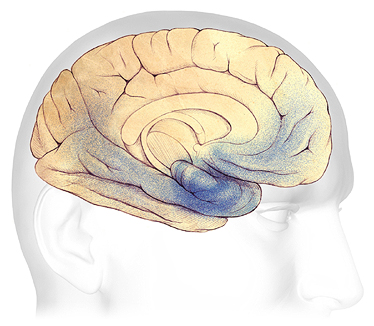
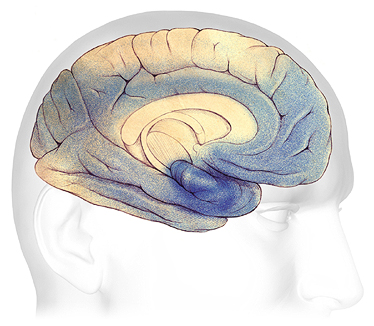
In Alzheimer’s, the progressive brain damage attributed to the formation of unwanted beta-amyloid plaques and neurofibrillary tangles is illustrated in the drawings below, which show the formation and spread of plaques and tangles (in blue). The blue areas represent damaged and dying nerve cells.
In Alzheimer’s disease, plaques and tangles first appear in an area of the temporal lobe called the hippocampus, where new memories are formed (A). As the disease progresses, plaques and tangles spread to the front part of the brain, affecting judgment and other high-level cognitive functions; symptoms begin to be obvious at this stage (B). In the severe stage (C), plaques and tangles are found throughout the brain. Damage eventually affects memory, emotions, communication, spatial awareness, safety awareness, logical thinking, recognition of loved ones, and the ability to care for oneself.
The Progression of Alzheimer’s Disease
|
A |
B |
C |
A: Plaques and tangles (shaded in blue) are beginning to form within the hippocampus. B: As the disease progresses, they spread towards the front and rear of the brain. C: In severe Alzheimer’s, plaques and tangles cause widespread damage throughout the brain. Source: The Alzheimer’s Association. Used with permission.
Vascular Dementia and Vascular Cognitive Impairment
Vascular dementia is one of the most common forms of dementia after Alzheimer’s disease, thought to be the cause of approximately 20-30% of the dementia cases worldwide (ADI, 2019). Vascular dementia usually has a stepwise onset, meaning symptoms can stay the same for a long period of time, then suddenly worsen. Memory may be less affected than in Alzheimer’s disease while fluctuations in mood are more common. Cognitive impairment is often “patchy” because of small vessel damage throughout the brain.
Vascular dementia is a general term used to describe changes in cognition resulting from impaired blood flow to the brain. It can be caused by a stroke or a series of small strokes or any condition that causes brain damage or reduces blood flow to the brain. Generally, vascular dementia doesn’t affect memory as much (or in the same way) as Alzheimer’s, at least in its early stage. Symptoms are related to the part of the brain experiencing reduced blood flow.
Vascular dementia can cause mood changes that are stronger than the mood changes you might see in someone with Alzheimer’s. It can also affect judgment—but not as strongly as in someone with frontal-temporal dementia. It can be difficult to differentiate vascular dementia and Alzheimer’s dementia because they can occur together. Cognitive changes can be gradual or occur in noticeable steps downward from a person’s previous level of function.
Risk factors for developing vascular dementia include diseases or disorders that damage the vessels supplying blood to the brain. The risk of developing dementia from vascular damage can be significant even when individuals have suffered only small strokes or minor damage to the blood vessels (NINDS, 2020). Risk factors associated with vascular dementia include hypertension, heart rhythm irregularities, diabetes, high cholesterol, smoking, sleep-disordered breathing, and a sedentary lifestyle (UCSF, 2020).
Frontal-temporal Dementia
Frontotemporal dementia begins in the frontal and temporal lobes of the brain. It is believed to start at an earlier age than Alzheimer’s disease and is a relatively common type of dementia in those under the age of 60. New research, however, is showing that frontotemporal dementia can start in older age. It is thought to be responsible for 5-10% of all cases of dementia (although its prevalence is likely underestimated). There is no single pathology attributed to frontal-temporal dementia—it is considered a “family” of neurodegenerative disorders.
Behavioral and personality changes associated with frontal-temporal dementia can be striking. This is because the frontal lobes are responsible for many of the traits and behaviors that mediate human behaviors. Damage to this part of the brain can lead to mood swings, disinhibition, inappropriate touching, loss of social decorum, loss of empathy in addition to language difficulties and problems with spatial orientation.
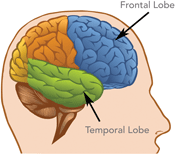
Damage to the brain’s frontal and temporal lobes causes forms of dementia called frontotemporal disorders. Left source: National Institute on Aging. Right source: Alzheimer’s Association, 2020 Used by permission.
Frontal-temporal dementia is usually categorized under three subtypes:
- Behavior variant frontotemporal dementia (bvFTD)—changes in personality and behavior that can affect people in their early 50s and 60s. Affects judgement, empathy, foresight, and planning.
- Primary progressive aphasia (PPA)—usually begins before the age of 65. Affects language skills, reading, writing, and comprehension.
- Disturbances of motor function, muscle weakness or wasting, without behavioral or language problems. (Alzheimer’s Association, 2020c)
Because frontotemporal dementia can also affect the hippocampus and because of the many variations found in the disease, it is often difficult to tell the difference between frontotemporal dementia and Alzheimer’s disease. It can also be confused with other psychiatric conditions such as late-onset schizophrenia.
Dementia with Lewy Bodies
Dementia with Lewy bodies (DLB) is another common type of progressive dementia. It accounts for up to 20-30% of all autopsy-confirmed dementias in older adults (Vermeiren et al., 2015).
DLB is caused by the build-up of abnormal proteins called Lewy bodies inside nerve cells in areas of the brain responsible for certain aspects of memory and motor control. It is not known exactly why Lewy bodies form or how Lewy bodies cause the symptoms of dementia (NINDS, 2019).
The similarity of symptoms between dementia with Lewy bodies, Parkinson’s disease, and Alzheimer’s disease can make diagnosis difficult. It is possible that either Lewy body dementia is related to these other causes of dementia or that an individual can have more than one type of dementia at the same time. Lewy body dementia usually occurs in people with no known family history of the disease. However, rare familial cases have occasionally been reported (NINDS, 2019).
Parkinson’s Disease Dementia
Mild cognitive impairment is common in the early stages of Parkinson’s disease and a majority of people with Parkinson’s disease will eventually develop dementia. The time from the onset of movement symptoms to the onset of dementia symptoms varies greatly from person to person.
Although Parkinson’s disease is initially associated with progressive difficulties with movement (slowed movement, postural instability, resting tremors), about 80% of people with Parkinson’s disease will eventually experience behavioral and cognitive changes. Symptoms are mild in the early course of the disease, then progressively worsen. This condition is closely related to Lewy body dementia—both diseases are caused by the build-up of alpha-synuclein proteins, which clump together, causing damage to nerve cells in the brain.
Lewy body dementia and Parkinson’s dementia are now recognized in the Diagnostic and Statistical Manual of Mental Disorders, where they are respectively coded as “Major and Mild Neurocognitive Disorder with Lewy Bodies” and as “Major and Mild Neurocognitive Disorder due to Parkinson’s Disease” (Donaghy and McKeith, 2014).
Post-Stroke Dementia
The risk for cognitive impairment or decline is increased by a history of stroke. As many as two-thirds of stroke patients experience cognitive impairment or cognitive decline following a stroke and approximately one-third go on to develop dementia. The risk for developing dementia may be 10 times greater among individuals with stroke than those without. Mortality rates among stroke patients with dementia are 2 to 6 times greater than among stroke patients without dementia (Teasell et al., 2014).
Functional Impairments
Dementia impairs judgment, alters visual-spatial perception, and decreases the ability to recognize and avoid hazards (Eshkoor et al., 2014). It also affects short-term memory and is thought to impair working memory, a type of memory that promotes active short-term maintenance of information for later access and use. The decline in working memory also affects language comprehension and visuospatial reasoning (Kirova et al., 2015).
When cognitive impairment is mild, studies indicate that lower attention/executive function or memory function may lead to a decline in gait speed. This is especially apparent when a person is walking and doing another task at the same time such as walking and talking, walking and crossing a busy street, or walking and carrying groceries—called “dual-task walking”. Slow gait speed may indicate deficits in the cognitive-processing speed or in executive and memory functions. The decline in cognitive function in people with mild cognitive impairment is not uniform, but rather depends on the type of cognitive impairment (Doi et al., 2014).
Because of these visual and perceptual changes, walking on a busy street can be dangerous, driving is no longer safe, and navigating around obstacles such as curbs, breaks in the sidewalk, stairs, and pets is a challenge. Visual and spatial difficulties also affect reading, comprehension of form and color, peripheral vision, and the ability to see contrast. This can make it difficult to accurately detect motion and process visual information (Quental et al., 2013).
Changes in Vision - Teepa Snow | MedBridge [3:11]
https://www.youtube.com/watch?v=iaUsRa5kNyw
Vascular dementia can cause impaired decision-making and judgment; mood changes are also common. Symptoms often begin suddenly and progress in a “step-wise” manner. This means the symptoms stay the same for a period of time, and then suddenly get worse, usually as a result of additional small strokes or other vascular damage. Mental impairment often seems “patchy,” because of the many different areas of the brain that are affected.
In the early stages of frontotemporal dementia, judgment and decision making are more affected than memory. There is a progressive change in behavior (mood changes, apathy, and disinhibition*), difficulties with language, and weakness or slowing of movement. People with frontotemporal dementia gradually lose control of their impulses—their behavior is often referred to as “odd,” “socially inappropriate,”, and “schizoid.”
*Disinhibition: a loss of inhibition, a lack of restraint, disregard for social convention, impulsiveness, poor safety awareness, an inability to stop strong responses, desires, or emotions.
The impulsive behavior and lack of judgment seen in people with frontotemporal dementia can cause inappropriate behaviors such as stealing, falling prey to internet or phone scams, excessive shopping, indecent exposure, and obsessive-compulsive behaviors such as pacing and hoarding.
Functional impairments associated with dementia with Lewy bodies include progressive cognitive decline, “fluctuations” in alertness and attention, visual hallucinations, and parkinsonian motor symptoms, such as slowness of movement, difficulty walking, or rigidity (stiffness) (NINDS, 2019). Nearly half of those with DLB also suffer from depression (Vermeiren et al., 2015).
Difficulty sleeping, loss of smell, and visual hallucinations can precede movement and other problems by as long as 10 years. Because of this, DLB can go unrecognized or be misdiagnosed as a psychiatric disorder until its later stages (NINDS, 2020).
Functional impairments associated with Parkinson’s disease dementia include the onset of Parkinson-related movement symptoms followed by mild cognitive impairment and sleep disorders, which involves frequent vivid nightmares and visual hallucinations (NINDS, 2020). Cognitive issues such as impaired memory, lack of social judgment, language difficulties, and deficits in reasoning can develop over time. Autopsy studies show that people with Parkinson’s dementia often have amyloid plaques and tau tangles similar to those found in people with Alzheimer’s disease, though it is not understood what these similarities mean.