Carefully designed activities can have a positive effect on depression, confusion, and challenging behaviors. Activities should provide a positive experience, be meaningful, and be challenging.
Telenius et al., 2022
Meaningful activities are based on a person’s interests, preferences, personhood, and perceived value (Yous et al., 2023). Meaningful activities help people living with dementia maintain a sense of identity, autonomy, and engagement. This includes adapting tasks to match the person's current abilities, modifying the environment to reduce barriers, and motivating a person to encourage involvement. Participation is not just about doing tasks—it's about being part of life in a way that has meaning for the person (Galof, 2025).
4.1 Individual Activities
Successful individual activity programs are based on a person’s likes, dislikes, and interests. This means learning about a person’s history and understanding their capabilities and preferences.
Determine whether they can still read, write, or use a computer and what they are physically capable of doing. Individual activities that stimulate the senses, such as cooking, singing, exercise, going for a drive, gardening, and aromatherapy, are encouraged at all stages of dementia.
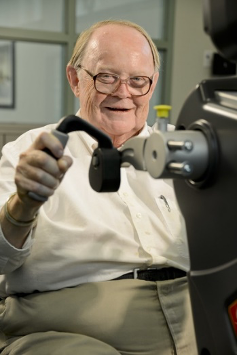

Left: A man using an upper extremity bike to exercise. Source: CDC, public domain. Right: A man enjoying a familiar activity. Southeastern Veterans Center licensed under CC BY-NC-ND 2.0.

Pet therapy at a skilled nursing facility. Source: CDC.
Some organizations that serve older adults, such as the Eden Alternative, encourage pets in their facilities. Pets provide companionship, promote relationships, and provide meaningful activity and exercise. Taking care of an animal gives a sense of purpose and companionship and is a key component of person-centered care.
Some people may refuse to participate in activities. Be on the lookout for signs of frustration and agitation and address these behaviors immediately.
Individual Activities at Different Stages of Dementia |
||||
|---|---|---|---|---|
Activity |
Mild |
Moderate |
Severe |
End of Life |
Word games |
Word searches, crossword puzzles. Card/computer games. |
Simple word searches, simple crossword puzzles. Simple computer games. |
Discuss a simple topic. Listen to others. |
Read to the person. |
Letter writing |
Write a letter. Send an email. Send email, use Facebook, social media. |
Dictate a letter or email. Use Facebook with help. |
Listen to a letter or email being read by caregiver. Respond to letters or email with direct supervision. |
Listen to an email or letter read by caregiver. Dictate a letter or text with caregiver assistance. |
Art/Music/ Reading |
Take photos. Create a photo album. Draw, play an instrument. Select and listen to books on tape. Select programs to listen to on the radio or TV. |
Take photos with supervision. Maintain a photo album. Draw, sing along with others. Listen to books on tape with headphones. Listen to the radio with headphones. Watch preferred TV programs. |
View photos Listen to music. Sing along to familiar songs. Listen to books on tape with headphones with caregiver assistance. Listen to the radio with headphones with caregiver assistance. |
Listen to music at low volume. Look at photos and pictures. Listen to TV, radio, or books on tape with direct assistance. |
Sewing |
Use sewing machine with help. Plan and complete projects with assistance. |
Use simple tools with supervision. Assist with projects. |
Use sewing cards, activity blankets or aprons with buttons, snaps, ties, Velcro, and zippers, watch projects |
Provide simple tools and templates. |
Gardening |
Garden in raised beds. Help plan the garden and harvest. |
Garden in raised beds with supervision. Perform specific gardening tasks with supervision. Eat food grown in garden. |
Sit in garden. Eat food grown in garden. Participate as able. |
Visit garden. Watch others garden. Watch gardening shows. |
Crafts |
Knit or crochet. Plan and complete art, sewing, painting, or woodworking. |
Knit using large needles. Choose colors, roll balls of yarn. Use simple tools with supervision. Engage in simple art, painting, sewing or woodworking projects with setup and assistance. |
Use simple activity boards with bolts, screws with setup and assistance. Choose colors, use the items that are created. Offer templates. |
Provide simple tools such as dry-erase pens. Provide direct setup and supervision. Observe projects completed by family members or caregivers. |
Home activities |
Help with laundry. Put clothes away. Assist with housekeeping. Assist with meal preparation. Select TV shows. Select radio shows. |
Sort and fold laundry. Assist with meal preparation as able. Assist with housekeeping as able. Assist with selection of radio and TV shows. |
Fold laundry. Assist with meal prep with close supervision. Listen to quiet music. |
Listen to quiet music. |
Shopping |
Go along to store, help with purchasing decisions. Help put groceries away. |
Go along to store, help as able with shopping decisions. Help put food away. |
Go along to store, sit in car with supervision or shop with wheelchair or electric cart. |
Go along to store if able. |
Meditation/ religious activities Support groups Reminiscence |
Attend church. Pray. Meditate. Attend a support group. Reminisce. |
Attend church, meditate, or attend a support group with a caregiver. Participate in an online support group with caregiver assistance. Reminisce. |
Pray or meditate at home with caregiver. Participate in an online support group or religious group with caregiver assistance. Reminisce. |
Listen to religious or spiritual music. Visit with someone from their religious community. Reminisce. |
Exercise |
Walking. Dancing. Stretching. Yoga. Stationary bicycle. Resistive exercise. Balance exercises. |
Walking. Stretching. Seated exercises. Stationary bicycle. Balance exercises with assistance. |
Walking with assistance. Seated exercises. Self-propelling a wheelchair. Assisted exercise in bed. |
Gentle bed exercises. Reaching and stretching with assistance. Rolling and turning in bed. Gentle touch. |


The author’s mother helps with gardening in her front yard. Source: Author.
4.2 Group Activities
Cognitive impairment isolates us from other people, causing anxiety, depression, withdrawal, and decreased self-confidence. Meaningful group activities help all of us maintain a sense of self-worth.
Small groups of 5 to 6 people allow more personal attention, although well-planned large-group activities can also be successful. Keep in mind that, as a person’s dementia progresses, group activities can become more challenging and individual activities may be preferred.
Group Activities at Different Stages of Dementia |
||||
|---|---|---|---|---|
Activity |
Mild |
Moderate |
Severe |
End of Life |
Singing |
Choose songs. Plan singing events. Sing with others. |
Choose songs. Sing with others. Sing familiar songs. |
Listen and sing along as able. |
Listen and sing along if able. |
Cooking |
Help plan meals. Bake cookies. Prepare a snack plate for others. Assist with cleanup after cooking. |
Help plan meals with assistance. Participate in making cookies. Assist with cleanup. |
Communicate food preferences. Help decorate cookies that are already baked. Eat the cookies. |
Communicate food preferences (may be nonverbal communication). Watch food preparation. |
Nature |
Outings to parks or nature areas. Group gardening. Group picnics. Group walks. |
Shorter walks. Drive to parks or nature areas with caregiver supervision. |
Escorted walk or wheelchair outside/ Attend picnic with direct supervision if able. |
View the outside. Watch nature shows on TV or computer. Go outside in wheelchair if able. |
Outings |
Group shopping. Eat out. Theater and music events, museum visits, library visits, attend sporting events. |
Same as mild with some adaptation and more supervision. Set up a store where the resident can purchase items. |
Watch movies. Participate in group outings as able with direct supervision. |
May be unable but offer outings with direct supervision if able. |
Group Exercise |
Choose/plan an exercise program. Go to gym with caregiver. Participate in Yoga, Tai Chi, Feldenkrais. Participate in balance activities. Participate in seated and standing group exercise. |
Attend organized exercise programs. Participate in Yoga, Tai Chi, Feldenkrais. Participate in balance activities. Participate in seated and standing group exercise. |
Attend organized exercise programs. Participate in seated and standing group exercise as able with direct assistance. Exercise and stretch in bed with direct supervision. |
Gentle stretching and movement in bed with direct assistance. Passive manual stretching. Weight shifting, rolling, moving in bed with direct assistance. |
An innovative group exercise program developed at the University of California at San Francisco integrates principles from several well-established traditions including Feldenkrais Method, Rosen Method, Tai Chi, and yoga, with elements from occupational therapy, physical therapy, and dance movement therapy (Chao et al., 2021).
The program, Preventing Loss of Independence through Exercise (PLIÉ), was specifically designed to address the needs of people living with cognitive impairment using seven guiding principles (Chao et al., 2021):
- Repetition with variation (to promote procedural learning while maintaining engagement).
- Progressive, functional movement (to support basic functional movements such as standing safely from a seated position).
- Slow pace and step-by-step instruction (to enable participants to participate fully, experience feelings of success, and minimize cognitive demands).
- Participant-centered goal orientation (a goals assessment is performed at the beginning of the program, and instructors tailor content to address the personal interests and goals of participants).
- Body awareness, mindfulness, and breathing (to bring nonjudgmental awareness to the body in the present moment).
- Social interaction (participants sit in a circle, and many movements involve reaching across the circle to touch hands or elbows or standing in a circle holding hands and moving together to facilitate social connection).
- Positive emotions (participants are encouraged to move in ways that feel good, personally meaningful music is incorporated, and all classes end with sharing of appreciations and things that bring joy).
4.3 Virtual Reality
There has been a great deal of research done in recent years on the use of virtual reality (VR) programs for older adults (with and without dementia). VR programs are designed to reduce loneliness, improve physical activity, and engage older adults in activities such as virtual travel.
Virtual reality offers a multisensory experience that can be attractive for people living with dementia because it stimulates multiple senses. VR may be helpful in improving memory, dual tasking,* and visual attention. For some people living with dementia, it can reduce anxiety, improve feelings of well-being, and increase use of coping strategies (Stasolla et al., 2024).
*Dual tasking: doing two things at once, such as walking and talking or cooking dinner while watching television.
Although the use of virtual reality is often user-friendly and well-accepted by older clients, side effects can occur. The most common reported side effects associated with virtual reality use include cybersickness (nausea, dizziness, disorientation, postural instability, and fatigue). Some people have reported delusions, strong negative emotional responses, upsetting memories. Adverse effects can also include vestibular-related side effects, physical experiences, and psychological impacts (Woo and Lee, 2023).
Some older virtual reality study participants reported issues with the head-mounted device, including that it was too heavy; caused general discomfort, disorientation and imbalance; and caused feelings of being trapped, confined, afraid, or anxious (Healy et al., 2022).
For a person living with Lewy body dementia, cognition can fluctuate from day to day. A person’s response to the use of a virtual reality device can be good one day and cause confusion, hallucinations, and panic the next day. To prevent cognitive overload* and hallucinations—especially in clients with Lewy body dementia—the virtual reality experience needs to be tailored to the user’s own capabilities. Keeping the programs simple and providing close monitoring can reduce or prevent these adverse reactions.
*Cognitive overload: when the brain tries to process too much information all at once.
