Acquiring and integrating knowledge, attitudes, and skills is a key component of cultural competence. Acquiring skills allows a provider to communicate across cultures, address cultural differences in communication, and understand the needs, values, and preferences of their patients. Cultural differences in communication, such as preferences regarding how and when interactions take place, tone, eye contact, and other factors must be considered, even when using interpreters (HHS, 2022).
5.1 Cultural Competence Training
There is strong evidence that cultural competence training for healthcare professionals improves providers’ knowledge, understanding, and skills for treating patients from culturally, linguistically, and socio-economically diverse backgrounds (UW, 2020).
Cultural competence training focuses on developing skills and knowledge that value diversity, cultural differences, and raise awareness of providers’ and care organizations’ cultural norms. Trainings can provide facts about patient cultures or include more complex interventions such as intercultural communication skills training, exploration of potential barriers to care, and institution of policies that are sensitive to the needs of patients from culturally and linguistically diverse backgrounds (UW, 2020).
In recent years, improvements have been seen in cultural competence training, although problems remain, such as:
- lack of consensus on what should be taught
- timing of training
- lack of standard references
- limited and inconsistent formal evaluation of interventions (Gradellini et al., 2021)
5.1.1 Notes on Educational Approaches
For many white people, a single required multicultural education course taken in college, or required “cultural competency training” in their workplace, is the only time they may encounter a direct and sustained challenge to their racial understandings.
Robin DiAngelo
White Fragility
Cultural competence occurs when knowledge, attitudes, and skills are integrated into a person’s daily actions. It requires a self-examination of one’s own cultural and professional background and helps healthcare providers manage prejudices and stereotypes that may affect their behavior when interacting with someone from a different culture (Gradellini et al., 2021).
Training is effective when it is multipronged, when people work and train together, and when it is designed with context and professional identity in mind. Training in teams helps individuals feel comfortable sharing their biases and accepting their vulnerabilities. Training in this way enhances collaboration and openness and reinforces behavioral change (Sukhera, 2020).
In one study, students who practiced responding in non-stereotypical ways to members of other groups were better able to avoid activating negative stereotypes. Other studies have found that contact between members of different groups reduces prejudices and hostilities. Equality of status, social and institutional support, pleasant contact, and intergroup cooperation produce positive results (Brusa et al., 2021).
A short video modified the racial attitudes of White college students towards peers of color. In this study, students were assigned to two experimental groups: one group viewed a short documentary depicting the life of a Caucasian and a Black subject, followed by hidden cameras over the course of a day, the other group did not view the video. Researchers found that the experimental group showed reduced prejudicial attitudes and reduced fear of minorities compared to the control group as assessed by the Color-Blind Racial Attitudes Scale, the Psychosocial Costs of Racism to Whites scale, and the Quick Discrimination Index (Brusa et al., 2021).
A widely used tool for understanding and improving cultural sensitivity is Bennett’s Developmental Model of Intercultural Sensitivity. Milton Bennett, a professor at Portland State University in Oregon, developed the tool as a framework to explain how people experience and engage cultural difference. It provides a roadmap of how we move from an ethnocentric to an ethnorelative perspective and highlights stages of development with the goal of intercultural acceptance, adaptability, and integration. It nicely sums up the principles discussed in this course.
Learn more about this tool here.
5.1.2 Using Case Review as a Teaching Tool
In the example that follows, the failure of an organization to provide language assistance services (or the doctor’s failure to use available services) led to a frustrating experience for the doctor, the hospital, and the patient.
Example Case: Mr. Louis and His Granddaughter
Mr. Louis just celebrated his 70th birthday with his family and neighbors with lots of good food, music, and dancing. Mr. Louis kept everyone up late, telling stories about his childhood in Haiti. Mr. Louis was grateful to have so many loved ones close by, but he still misses Haiti after moving so many years ago.
Soon after his birthday, Mr. Louis visited his physician for a checkup. His physician sent him for additional testing, which showed the presence of prostate cancer. Let’s see what happens during Mr. Louis’ appointment with the oncologist, Dr. Emily Parker.
The Initial Appointment
Mr. Louis brought his granddaughter, Esther, to his oncology appointment at the hospital to help him speak with the oncologist. He knows some English, but he was worried that he would not understand everything that the doctor might say. Plus, Mr. Louis was nervous, he wanted his granddaughter there for support.
Once the appointment began, Dr. Parker and Esther did all the talking. Mr. Louis did not get a chance to speak, and he did not understand most of what Dr. Parker and Esther were saying. After a few minutes, Esther seemed to be arguing with Dr. Parker. This embarrassed Mr. Louis, and he stayed quiet.
After the First Appointment
After the appointment, Esther explained to her grandfather in French that, to treat his cancer, he would undergo a procedure the next week that would implant radioactive seeds. Esther told Mr. Louis that the procedure was simple, painless, and without side effects. She did not mention what else the doctor said or what she seemed they seemed to be arguing about during the visit.
Back at home, Mr. Louis began to worry about the procedure. He researched the procedure online and talked with his friends. He learned that the procedure did have side effects, including the possibility of incontinence. Remembering how Esther had argued with the doctor, Mr. Louis wondered if she had told him the truth about her conversation with Dr. Parker.
The Surgical Appointment
The next week, Mr. Louis and Esther arrived at the admissions office at the hospital. “No surgery,” said Mr. Louis firmly. The admissions clerk looked up in surprise, and Esther quickly started talking to her in English. She explained that Mr. Louis did not really understand the issue and that he really did want the surgery.
Esther asked to sign the papers for her grandfather, but the admissions clerk explained that without legal standing, Esther was not eligible to do so. Mr. Louis continued to quietly say, “No surgery.” The admissions clerk had no idea what to do. The surgical staff called to say that they were waiting for Mr. Louis. Esther glared at her grandfather.
The clerk spent almost half an hour trying to find a hospital staff member who spoke French, but no one was available. The surgery staff called again, saying that if Mr. Louis did not arrive shortly, they would have to reschedule his procedure.
Exasperated, Esther insisted that Mr. Louis undergo the procedure. She said, “The hospital has people ready to do this. All those people’s time will just be wasted. Come on, just sign the paper and we can get you upstairs.” Mr. Louis said again, “No surgery.” Esther had no choice but to take him home.
Mr. Louis’s Response
“I depended on my granddaughter to help me with my oncology appointment. But she did not tell me the truth about the surgery and my options to treat my illness. I am really angry that I came very close to having a surgery I did not want! It was so frustrating to not be able to communicate directly with my doctor. All I wanted was someone who could listen to me and explain my options.”
Mr. Louis’s Doctor Responds
“These days, I see a lot of patients who don’t speak English very well or at all. I’m used to communicating with a family member or friend instead of the patient. In fact, I ask patients to bring someone who can interpret for them. It’s so much easier that way!”
“But when I heard about Mr. Louis’ situation from our admissions clerk, I was shocked! I did not recommend the procedure that Esther scheduled for her grandfather. I actually suggested "watchful waiting" as Mr. Louis’ treatment option. But, during the consultation, his granddaughter insisted that Mr. Louis undergo the procedure. Now that I think about it, I didn’t speak much with Mr. Louis since Esther seemed to be in charge. I thought I was doing the right thing by speaking with the family member that Mr. Louis brought with him. Now, knowing that Mr. Louis did not want surgery scares me. I wish I had been able to speak directly with Mr. Louis without his granddaughter interfering.”
Conclusion
Offering language assistance services, including a competent medical interpreter, helps patients with limited English proficiency understand and make informed decisions about their medical care. Unfortunately, Mr. Louis almost had a surgery that he did not want, and the surgery could have caused side effects about which he had not been informed. Operating on a patient who did not want surgery or who was not aware of potential adverse effects could have serious liability implications for the doctor and the hospital.
Furthermore, the hospital had a surgery team and room sitting idle because a patient was scheduled for a procedure that he did not want. In this case, the cost of providing a trained interpreter would have been significantly less than the costs that the hospital incurred from this.
Think About It
- How would you feel if this happened to you or a family member?
- Could this happen at your organization?
- Does your workplace offer communication assistance?
Source: HHS, 2022
5.2 Promoting Collaboration on Healthcare Decisions
Healthcare providers recognize they have a special relationship with their patients that is based on trust, which is one of the pillars of the professionalism on which the healthcare relationship rests. When patients have an injury or disability, their increased vulnerability creates special challenges within the general population and within the healthcare system. Engaging patients in their care is a key component of good practice.
The World Health Organization describes collaborative practice as occurring when healthcare workers from diverse professional backgrounds work with patients and their families to deliver high quality care. The involvement of patients as central to healthcare is recognized as essential and differs fundamentally to traditional clinician-centered healthcare (Davidson et al., 2022).
Collaborative decision-making occurs when patients work together with their healthcare providers to make decisions about screening, treatments, and managing chronic conditions. Shared decision-making upholds person-centered care and allows people to take an active role in their healthcare decisions. With shared decision-making, the person’s individual preferences, beliefs, and values are considered when making health decisions (Jull et al., 2021).
Importantly, shared decision-making helps people understand the risks and benefits of different options through discussion and information sharing. In fact, shared decision-making has been called “the pinnacle” of person-centered care. A key feature of shared decision-making is the exploration of patient values and priorities, which can be facilitated by using evidence-based decision support tools and approaches (Jull et al., 2021).
“Decision-coaching” and decision aids encourage patients to take an active role in their healthcare decisions. Decision aids include booklets, videos, and online tools that help people clarify what matters to them. These tools help people feel more knowledgeable, better informed, and encourage them to take an active role in decision-making (Jull et al., 2021).
5.3 Developing Good Communication Tools
Data from the U.S. Census reveal a high degree of linguistic diversity, with more than 59 million residents speaking a language other than English at home. More than 25 million people live in linguistic isolation, a termed coined by the U.S. Census Bureau in which no one in a household over 14 years of age speaks English at least very well (NCCC, Nd).
In Oregon, 15% of residents speak a language other than English. The largest non-English language spoken in Oregon is Spanish, representing 9% of Oregon’s population. The next most-common non-English language is Chinese (Mandarin, Cantonese), followed by Vietnamese. As a comparison, New York City—with a population of over 8 million people—has more than 800 spoken languages (Data USA, 2023).
On August 11, 2000, the President signed Executive Order 13166, “Improving Access to Services for Persons with Limited English Proficiency”. The Executive Order requires Federal agencies to examine the services they provide, identify the need for services for those with limited English proficiency, and develop and implement a system to provide meaningful access to those services for people with limited English proficiency (NIH, 2022, August 31).
5.3.1 Good Communication is a Two-Way Dialogue
The intimate and sometimes overwhelming nature of health concerns can make communication challenging. Nevertheless, patient-centered communication is fundamental to ensuring good health outcomes, reflecting long-held values that care must be individualized and responsive to patient health concerns (Kwame and Petrucka, 2021).
Effective communication is a two-way dialogue between patients and care providers. In that dialogue, both parties speak and are listened to without interrupting; they ask questions for clarity, express their opinions, exchange information, and grasp entirely and understand what the others mean (Kwame and Petrucka, 2021).
Cultural competence has been linked to increased patient satisfaction and treatment adherence. By contrast, cultural and linguistic differences between healthcare providers and patients can cause significant miscommunication, decreasing patient trust and satisfaction. (Jongen et al., 2018).
If a provider lacks cross-cultural communication skills or if interpretation and translation services are not provided, the impact on a patient can be dire. Poor communication contributes to an incomplete and inaccurate health history, misdiagnoses, and the failure of a patient to understand their health condition and recommended treatment. This can lead to misuse of medications, repeat visits, and lack of informed consent (NCCC, nd).
Effective communication means providing information to an individual in an understandable and accessible way. The goal is to increase knowledge about prevention and maintenance of good health while positively influencing health behaviors and attitudes. This involves verbal, written, and nonverbal communication (HHS, 2022).
Studies have shown that a consistent communication-related barrier in nurse-patient interactions is miscommunication, which often leads to misunderstandings between nurses, patients, and their families. Additional communication-related barriers include language differences, poor communication skills, and a patient’s inability to communicate due to their health state, especially in ICU, dementia, or end-of-life care contexts (Kwame and Petrucka, 2021).
5.3.2 National CLAS Standards
Culturally and Linguistically Appropriate Services (CLAS) standards are a set of 15 action steps. The standards are intended to advance health equity, improve quality, and help eliminate healthcare disparities by providing a blueprint for individuals and healthcare organizations to implement culturally and linguistically appropriate services (OMH, 2022).
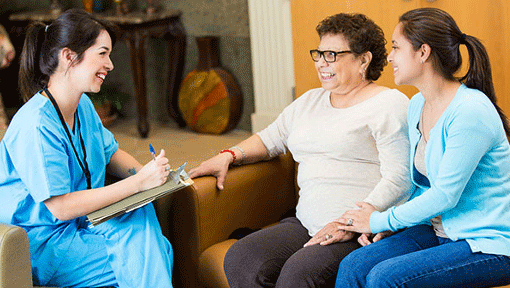
A bilingual doctor discussing health issues with a patient and her daughter. Source: HHS, public domain.
CLAS standards can improve the quality of services provided to all individuals, which will ultimately help reduce health disparities and improve health equity. CLAS standards encourage respect and responsiveness: respect the whole individual and respond to the individual’s health needs and preferences.
To reduce barriers to accessing quality and appropriate care for priority populations and advance health equity, the Oregon Health Authority expects all Oregon Health Plan enrolled providers and coordinated care organizations to provide services in support of OHA’s health equity goals, consistent with National CLAS Standards. This means all health services, including telemedicine services:
- Are culturally responsive.
- Provide meaningful access to language services.
- Are provided in an equitable and inclusive manner.
5.3.3 TeamSTEPPS
The TeamSTEPPS Limited English Proficiency program provides hospitals with the tools to develop and implement a plan to train interpreter and clinical staff in teamwork skills, specifically within the context of working with patients with limited English. The program includes train-the-trainer resources and instructional guides that include short case studies and videos (PSNET, 2019).
The success of TeamSTEPPS is well-documented and field testing concluded it was easy to implement and fostered staff learning. In addition to implementing the TeamSTEPPS program, hospitals are encouraged to: 1) foster a supportive culture for the safety of diverse patients, 2) adapt current systems to better identify medical errors among patients with limited English proficiency, 3) improve reporting of medical errors for patients with limited English proficiency, 4) routinely monitor patient safety for patients with limited English proficiency, and 5) address root causes to prevent medical errors among patients with limited English proficiency (PSNET, 2019).
5.3.4 Language Assistance Services
In the United States, healthcare organizations are required by law to provide interpretation services at no cost. Notification of communication and language assistance services allows organizations to avoid legal ramifications from miscommunications between provider and patient, which could potentially lead to malpractice and legal action against a provider and their organization.
Language assistance services such as oral interpretation, translation of written documents, signage, and wayfinding symbols greatly improve communication for patients with limited English proficiency and those who are deaf or hard of hearing. Healthcare organizations should notify patients that communication and language assistance services are available when scheduling an appointment. This helps patients (and their families) make better use of services and also helps them become more informed consumers of healthcare (HHS, 2022).
UC Davis nursing students reducing language barriers to improve health care [3:19]
https://www.youtube.com/watch?v=9pST-K1aS14
Source: Betty Irene Moore School of Nursing at UC Davis.
Providers might try to “get by” with the limited English skills of patients, their own inadequate foreign language skills, or unqualified interpreters, such as patients’ friends or family members or untrained staff. Examples of documented patient safety events due to a lack of language assistance include performing an x-ray on the wrong part of the body, falls due to the patient not knowing to ask for assistance, and inability to treat emergency room patients due to failure to obtain medical history or medication list (PSNET, 2019).
5.3.5 Working with Interpreters
In 2021, the Oregon Legislature passed House Bill 2359, requiring that all publicly funded healthcare providers hire only credentialed healthcare interpreters listed on a state registry. To obtain accreditation and entry onto the state’s registry, interpreters must pass language proficiency testing and meet other requirements. The bill was intended to make access to healthcare more equitable (Lund Report, 2022).
Using interpreters and translation services reduces disparities by bridging the communication gap between providers and patients with limited English proficiency. These services ensure that all parties understand a provider’s medical instructions and diagnoses and can also provide a more comfortable and trusting environment for patients.
Examples of language assistance services include oral interpretation, translation of written documents, signage, and wayfinding symbols. Individuals with language needs include those with limited English proficiency and those who are deaf or hard of hearing. Language assistance services should be provided at no cost to the patient (HHS, 2022).
Healthcare organizations should not use family members, children, other patients or visitors, or untrained staff as interpreters. Interpreters are communication professionals who will interpret everything that is said, maintain confidentiality, and provide a cultural context.
Interpreters and translators differ in their jobs. A translator works with the written word, translating from one language to another while an interpreter translates spoken information.
Interpreters’ and translators’ roles are diverse and include being a cultural broker, patient advocate, co-therapist, team member. and institutional gate keeper. It is often the provider’s responsibility to train interpreters and translators working under their supervision in procedures and ethics (Louw, 2016).
Healthcare providers are responsible for the actions of interpreters and translators, ensuring that they act ethically, which may not always be easy to implement. Interpreters and translators are required to show respect for all involved, respect confidentiality, interpret accurately, convey cultural information, and remain impartial (Louw, 2016).
Working with Interpreters [4:57]
https://www.youtube.com/watch?v=pVm27HLLiiQ
Source: Legal Services New Jersey.
5.3.6 Working with Cultural Brokers
Cultural brokers provide a link between a patient’s traditional health beliefs and practices and the healthcare system. Interpreters, community health workers, and patient navigators can play the role of a cultural broker by providing context and by serving as a partner for both the patient and provider (PSNET, 2019).
While a cultural broker’s role can vary depending on patient and provider need, cultural brokers must be knowledgeable about the cultural group they serve and be able to successfully navigate the healthcare system. An individual acting as a cultural broker should be a trusted and respected member of the community but does not need to be healthcare professionals (PSNET, 2019).
Incorporation of a cultural broker in the care team embraces the importance of cultural distinctions among patient groups. It also acknowledges that, particularly in very diverse communities, it is unrealistic for providers to have sufficient understanding of all the different cultures present in the patient population they serve (PSNET, 2019).
Test Your Knowledge
1. If a person asks for an interpreter, can I assume they won’t understand if I say something to a colleague in front of the patient?
Answer: It is not uncommon that a person who asks for an interpreter understands English quite well. Any comments you make to other providers or to the interpreter might be understood by the patient.
2. Today, I had a patient who I thought might need translation assistance, but the patient declined this service. I didn’t want to embarrass her by insisting—I assumed her refusal meant she would clearly understand everything we were going to discuss—so, I just dropped it.
Answer: If a patient refuses language assistance services, ask them to sign a form that says they understand that language assistance is available, and have chosen to decline these services. The form must be available and signed in the patient’s native language or completed orally if he or she is unable to read in their native language.
Document that the individual was notified about these rights and include the patient's preferences for utilizing language services in the future. Written documentation is needed to communicate with other providers and to indicate that language services are available and were offered.
Modified from Think Cultural Health: Working Effectively with an Interpreter
5.3.7 Working with Traditional Health Workers
Traditional Health Worker roles were defined in the original bill that created Oregon’s Coordinated Care Organizations (CCOs) in 2011, House Bill 3650. Now codified in ORS 414.665, there are five specialty types of Traditional Health Workers in Oregon (Li, et al., 2023):
- Community Health Workers
- Peer Wellness Specialists
- Peer Support Specialists
- Personal Health Navigators
- Birth Doulas
Traditional Health Workers are individuals from their local communities who provide person- and community-centered care by providing a bridge between communities and the health systems they serve. They can increase the appropriate use of care by connecting people with health systems, advocating for their clients, supporting adherence to care and treatment, and empowering individuals to be agents in improving their own health. As of October 2022, there were more than 4,400 Traditional Health Workers certified in Oregon (Li et al., 2023).
The effectiveness of Traditional Health Workers is enhanced when they have similar lived experience or are members of the same community as the patients they serve, have knowledge of health issues, and understand how to help patients navigate the health system. Traditional Health Workers help to assure the delivery of high-quality, culturally responsive care, which is instrumental in achieving the Oregon Health Authority’s goal to eliminate health inequities in Oregon by 2030 (Li et al., 2023).
5.3.8 Working with Traditional Medicine/Healers
American Indian and Indigenous peoples utilize traditional medicine/healing for health and well-being. Modern, Western-trained healthcare practitioners receive minimal training and education on traditional these healing practices and their application and integration into healthcare settings. Lack of knowledge and practice guidelines on how to navigate these two healthcare perspectives creates uncertainties in the treatment of American Indian and Indigenous peoples. Such conflicts can undermine patient autonomy and result in culturally incongruent practice (Esposito and Kahn-John, 2022).
One challenge Western-trained healthcare a provider may face is respecting a person’s autonomy by allowing them to choose and prioritize health and wellness interventions they feel best fit their physical, mental, emotional, and spiritual needs. These are valid concerns and must be considered, discussed, and explored to maintain optimal health and safety of patients (Esposito and Kahn-John, 2022).
For Western-trained healthcare providers, training in traditional medicine/healing and learning how to integrate Western medicine and traditional medicine is an important part of providing comprehensive, culturally inclusive, and effective care. Traditional medicine/healing education should be integrated on several levels of Western medical training (Esposito and Kahn-John, 2022).
5.4 Utilizing Data to Inform Clinical Practice and Health Equity
Collecting and utilizing data to inform clinical practice and improve health equity starts with defining the population and health equity issue you plan to address. The first step is to identify disparities by collecting and analyzing data on patient demographics, disease prevalence, and treatment outcomes.
Once disparities have been identified, the data is used to develop targeted interventions. For example, a healthcare organization may implement outreach programs to increase access to care for marginalized populations or create targeted treatment plans based on patient data.
Monitoring outcomes for effectiveness is the next step. This may involve collecting data on patient outcomes, patient satisfaction, and changes in health disparities over time. Engaging patients is a critical part of improving clinical practice. This can involve gathering patient feedback on their experiences with care and incorporating it into decision-making processes.
In Oregon, the Oregon Health Authority collects and analyzes data on health outcomes and health disparities, including race/ethnicity, language, income, and geographic location. The organization then identifies areas where health disparities exist and prioritizes interventions and initiatives aimed at reducing health disparities and improving health equity.
OHA has used this data to develop a series of culturally and linguistically appropriate outreach and education programs aimed at reducing disparities in chronic disease management among communities of color. They have also worked to increase the availability and use of health data in clinical practice, including implementing health information technology systems and training health providers in the use of data to inform patient care.
5.4.1 Institutional Culture and Health Equity
Institutional culture in healthcare refers to the shared beliefs, values, attitudes, and behaviors that are present within a healthcare organization. It encompasses all aspects of the organizational structure, from its mission and vision to its policies and procedures, to the interactions and relationships among staff members.
Healthcare organizations that prioritize health equity will typically have an institutional culture that emphasizes diversity and inclusivity, values patient-centered care, and supports ongoing training and education for healthcare providers. This type of institutional culture prioritizes community engagement and outreach, and supports policies and initiatives aimed at reducing disparities in health outcomes and access to care.
The governance structure of a healthcare organization can play a role in improving health equity. Addressing health inequities by recognizing and decreasing institutional racism and other forms of discrimination can have a significant impact on improving an organization’s culture (Browne et al., 2018).
5.4.2 Implementing Health Equity Interventions
Health equity interventions can be implemented at multiple levels within health organizations and at the level of clinical practice. Specific interventions can vary but are characterized by a common goal of closing the health equity gap with the aim of 1) improving the health of populations, 2) enhancing patient experience and outcomes, and 3) reducing per capita cost of care (Browne et al., 2018).
5.4.3 Health Disparities and Social Inequities
Unequal social practices create gaps in health. One example is redlining, a practice where lenders deny mortgages to eligible buyers solely because of their race. These practices assured that Black people and other people of color are denied the right of home ownership and upward economic mobility that millions of White people enjoy. Redlining has been succeeded by gentrification, whereby middle-class people move into urban areas and displace others who have lived in a neighborhood for years (Julian, Hardeman, and Huerto, 2020).
Both redlining and gentrification perpetuate poverty in communities of color in America’s cities. As such, many Black and low-income Americans live in communities where clean water isn’t guaranteed, and social distancing is nearly impossible in crowded homes. In this way, redlining and gentrification have impacted the racial inequities seen during the COVID-19 pandemic (Julian, Hardeman, and Huerto, 2020).
5.5 Collaborating with Community Resources
Collaborating with other stakeholders, such as public health agencies and community-based organizations, is critical to improving clinical practice related to health equity. These organizations provide valuable insights into the needs of marginalized populations and help healthcare providers develop targeted interventions that are effective and sustainable.
Black and Latino individuals—especially women—comprise an essential part of the healthcare workforce, often serving in support roles such as nursing assistants and dietary service staff. Compared to physicians and nurses, they are underpaid and undervalued. In many cases, these healthcare workers have closer relationships with their communities than other healthcare professionals, representing an untapped opportunity to improve workforce cultural competence. These workers often live in the same communities that they serve and have strong ties with community members. Many times, they share ethnicity, language, socioeconomic status, and life experiences with the community (Rivera-Núñez et al., 2022).
5.5.1 Developing Community Partnerships
Developing partnerships with local community organizations helps healthcare providers understand and meet the needs of different cultural communities. These organizations provide valuable insight into the needs of their communities and can help develop programs that address social determinants of health.
5.5.2 Increasing Access to Care
Increasing access to care and services in underserved communities can reduce cultural disparities in healthcare. This is achieved by reducing transportation barriers, increasing affordability, and providing more convenient hours to accommodate different work and family schedules.
5.5.3 Developing Culturally Relevant Programs
Developing culturally relevant programs reduces healthcare disparities by helping patients learn about preventive care and other healthcare services. These programs should be tailored to the needs and cultures of the community and should be designed to address health issues in a culturally appropriate way.
Health literacy is closely related to culturally relevant programs. One aspect of health literacy is training providers to communicate health information in a way that is easy for patients to understand by using clear language, avoiding medical jargon, and developing well-designed visuals and written materials helps patients understand their health status and treatment options.
