Selection and use of barriers and/or personal protective equipment (PPE) for preventing patient and healthcare worker contact with potentially infectious material.
[This section is taken from OSHA, 2012, 1991 and CDC, 2004.]
Personal protective equipment (PPE) includes barriers such as gloves, gowns, masks, goggles, and face shields. They protect patients and workers from exposure to bloodborne pathogens on the job. Use of PPE is part of Standard Precautions, used with all patients, and is required by OSHA.
Under OSHA’s General Duty Clause, PPE is also required for any potential infectious disease exposure. Employers must provide their employees with appropriate PPE and ensure its proper disposal. If reusable, it must be properly cleaned or laundered, repaired, and stored after use.
Selecting PPE
Selection of PPE—particularly the combination of more than one type of protective equipment—is determined by the category of the patient’s isolation precautions and the type of anticipated exposure. Touch, splashes or sprays, or large volumes of blood or bodily fluids might penetrate protective clothing. Anticipated exposure will affect whether PPE needs to be fluid resistant, fluid proof, or neither. When selecting protective equipment, consider its durability and appropriateness for the task.
Procedures that generate splashes or sprays of blood, body fluids, secretions, or excretions—such as open endotracheal suctioning, bronchoscopy, invasive vascular procedures—require either a face shield (disposable or reusable) or mask and goggles. The wearing of masks, eye protection, and face shields in specified circumstances when blood or bodily fluid exposures are likely to occur is mandated by the OSHA Bloodborne Pathogens Standard.
Types of PPE/Barriers
Personal protective equipment (PPE) is “specialized clothing or equipment worn by an employee for protection against infectious materials.” In addition to the familiar gloves and gowns, PPE includes a variety of barriers and respirators used alone or in combination to protect skin, mucous membranes, and airways from contact with infectious agents. The selection of PPE is based on the nature of the patient interaction and the likely mode of transmission.
Gloves
Wear gloves:
- When contact with blood, body fluid, mucous membranes or non-intact skin is anticipated
- When performing vascular access procedures
- For contact with contaminated items or surfaces (OSHA)
Always change gloves between patients!
- Always do hand hygiene following removal of gloves, in case of:
- Unsuspected holes in the gloves
- Contamination of the hands during glove removal
Gloves used in the healthcare setting are subject to FDA evaluation and clearance. Nonsterile disposable medical gloves made of latex or nitrile should be available for routine patient care.
In the non-surgical setting, the selection of glove type is based on the task to be performed, anticipated contact with chemicals and chemotherapeutic agents, latex sensitivity, sizing, and facility policies for creating a latex-free environment. For contact with blood and body fluids, a single pair of gloves generally provides adequate barrier protection.
There is considerable variability among gloves. Both the quality of the manufacturing process and type of material influence their effectiveness. While there is little difference in the barrier properties of unused intact gloves, studies have repeatedly shown that vinyl gloves have higher failure rates than latex or nitrile gloves when tested under simulated and actual clinical conditions. For this reason either latex or nitrile gloves are preferable for clinical procedures that require manual dexterity or will involve more than brief patient contact. Heavier, reusable utility gloves are indicated for non-patient care activities, such as handling or cleaning contaminated equipment or surfaces.
Proper Procedure for Donning Gloves
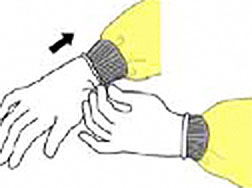
Extend gloves over isolation gown cuffs to provide a more reliable and continuous barrier for the arms, wrists, and hands. Source: CDC.
During patient care, transmission of infectious organisms can be reduced by adhering to the principles of working from “clean” to “dirty,” and confining or limiting contamination to surfaces that are directly needed for patient care. It may be necessary to change gloves during the care of a single patient to prevent cross-contamination of body sites. It also may be necessary to change gloves if the patient interaction involves touching portable computer keyboards or other mobile equipment that is transported from room to room.
Gloves must be changed between patients to prevent transmission of infectious material. They should never be washed and reused because microorganisms cannot be removed reliably from glove surfaces and continued glove integrity cannot be ensured. Glove reuse has been associated with transmission of MRSA and gram-negative bacilli.
When gloves are worn in combination with other PPE, put them on last. Gloves that fit snugly around the wrist are preferred for use with an isolation gown because they can cover the gown cuff and provide a more reliable continuous barrier for the arms, wrists, and hands. Gloves that are removed properly will prevent hand contamination. Hand hygiene following glove removal further ensures that the hands will not carry potentially infectious material that might have penetrated through unrecognized tears or that could contaminate the hands during glove removal.
Cover Garb: Gowns and Lab Coats
Wear a gown or fluid-resistant lab coat whenever soiling of skin or clothing is anticipated. Remember that a gown may be needed during the care of a patient on Standard Precautions.
Gowns are intended to protect your arms and exposed body areas and prevent contamination of clothing with blood, body fluids, and OPIM. The type of gown is chosen based on the nature of the patient interaction, including the anticipated degree of contact with infectious material and potential for blood and bodily fluid penetration of the barrier. Clinical and laboratory coats or jackets worn over personal clothing for comfort or purposes of identity are not considered PPE.
Gowns are always worn in combination with gloves, and with other PPE when indicated. Gowns are usually the first piece of PPE to be donned. Full coverage of the arms and body front, from neck to the mid-thigh or below, will ensure that clothing and exposed upper body areas are protected. Several gown sizes should be available in a healthcare facility to ensure appropriate coverage for staff members.
Gowns should be removed before leaving the patient care area to prevent possible contamination of the environment outside the patient’s room. Gowns should be removed in a manner that prevents contamination of clothing or skin. The outer, “contaminated” side of the gown is turned inward and rolled into a bundle, and then discarded into a designated container to contain contamination. Do not reuse gowns.
Masks
Masks by themselves are used for three primary purposes in healthcare settings: (1) to protect workers from contact with infectious material from patients, e.g., respiratory secretions; (2) to protect patients from exposure to infectious agents carried in the workers’ mouths or noses when they are engaged in procedures requiring sterile technique, and (3) to put on coughing patients, to limit potential dissemination of infectious respiratory secretions from the patient to others, as part of Respiratory Hygiene.
A mask may be worn without eye protection, but eye protection must be worn with a mask (OSHA). Masks should not be confused with respirators that are used to prevent inhalation of small particles that may contain infectious agents transmitted via the airborne route.
An N-95 Respirator

Note N-95 identifier in horizontal box at the bottom of the text. Source: 3M, 2014.
When Airborne Precautions are used, a respirator is required. It may be an N-95 respirator, which requires fit testing, or a positive air-purifying respirator (PAPR), which does not require fit testing. These are discussed in Element II in the section on tuberculosis.
There are many types of disposable particulate respirators, also known as air-purifying respirators because they protect by filtering particles out of the air as you breathe. These respirators protect only against particles—not gases or vapors. Since airborne biologic agents such as bacteria or viruses are particles, they can be filtered by particulate respirators. An N-95 respirator is an example of a particulate respirator; it must be fit-tested as required by OSHA to verify a good seal. Facial hair may interfere with a good seal, requiring use of a positive-pressure respirator that does not require a seal.
Face Shields and Goggles
Masks in combination with eye protection devices, such as goggles or glasses with solid side shields, or chin-length face shields, shall be worn whenever splashes, spatter, or droplets of blood or OPIM may be generated and eye, nose, or mouth contamination can be reasonably anticipated (OSHA).
Note: A mask always accompanies eye protection unless a face shield is used.
The eye protection chosen for specific work situations—for example, goggles or face shield—depends upon the circumstances of exposure, other PPE used, and personal vision needs. Personal eyeglasses and contact lenses are not considered adequate eye protection. Eye protection must be comfortable, allow for sufficient peripheral vision, and be adjustable to ensure a secure fit.
Indirectly vented goggles with a manufacturer’s anti-fog coating may provide the most reliable practical eye protection from splashes, sprays, and respiratory droplets from multiple angles. Newer styles of goggles may provide better indirect airflow properties to reduce fogging, as well as better peripheral vision and more size options for fitting goggles to various workers (see below). Many styles of goggles fit adequately over prescription glasses with minimal gaps. While effective as eye protection, goggles do not provide splash or spray protection to other parts of the face.
Safety Goggles
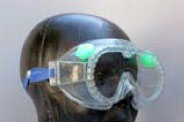

Goggles for splash or fine dust protection should have indirect venting. Source: CDC.
As compared with goggles, a face shield can provide protection to other facial areas in addition to the eyes. Face shields extending from chin to forehead provide better face and eye protection from splashes and sprays; face shields that wrap around the sides may reduce splashes around the edge of the shield. Removal of a face shield, goggles and mask can be performed safely after gloves have been removed and hand hygiene performed. The ties, ear pieces, and/or headband used to secure the equipment to the head are considered “clean” and therefore safe to touch with bare hands. The front of a mask, goggles, or face shield is considered contaminated.
Application of PPE
Personal protective equipment must fit the individual user, and it is up to the employer to ensure that all PPE are available in sizes appropriate for the workforce to be protected. Gloves should fit the user’s hands comfortably—they should not be too loose or too tight. They also should not tear or be easily damaged. If contamination of the arms can be anticipated, a gown should be selected. Gowns should fully cover the torso, fit comfortably over the body, and have long sleeves that fit snuggly at the wrist.
Masks should fit snuggly and fully cover the nose and mouth to prevent fluid penetration. For this reason, masks that have a flexible nose piece and can be secured to the head with string ties or elastic are preferable. Goggles provide barrier protection for the eyes and should fit snuggly over and around the eyes or personal prescription lenses. Personal prescription lenses do not provide optimal eye protection and should not be used as a substitute for goggles. Goggles with prescription lenses are available.
Before you use a respirator, your employer is required to have you medically evaluated to determine that it is safe for you to wear a respirator, to fit test you for the appropriate respirator size and type, and to train you on how and when to use a respirator. You are responsible for fit checking your respirator before every use to make sure it has a proper seal.
In addition to providing employees with appropriate PPE, employers are responsible for its proper disposal. If protective equipment is reusable it must be properly cleaned or laundered, repaired, and stored after use. Many types of PPE, such as latex gloves and disposable gowns, are used once and then discarded in an appropriate receptacle. Other types of PPE, such as cloth gowns or reusable heavy duty latex or nitrile gloves, can be cleaned and reused. If goggles or face shields are reusable, they must be placed in a designated receptacle for subsequent reprocessing. If they are not reusable they may be discarded in a waste receptacle.
PPE is a potential source of cross-contamination if not changed between patients. To avoid cross-contamination:
- Don PPE before contact with the patient, generally before entering the room.
- Use carefully—don’t spread contamination. Avoid touching the environment with soiled gloves.
- Remove and discard carefully, either at the doorway or immediately outside the patient room.
- Remove respirator outside the room.
- Immediately perform hand hygiene.
The use of personal protective equipment is not a substitute for safe work practices. Avoid contaminating yourself by keeping your hands away from your face and not touching or adjusting PPE. Also, remove your gloves if they become torn and perform hand hygiene before putting on a new pair of gloves. Avoid spreading contamination by limiting surfaces and items touched with contaminated gloves.
Back Next