In 2020, the national rate of unintentional fall deaths for adults aged 65 and over was 65.6 deaths per 100,000 population. About 37% of these falls required medical care and restricted activity for at least a day (CDC, 2023, September 6). Among older adults, lacerations, hip fractures, or head traumas occur in about a quarter of people who fall, and falls are the most common cause of hospital admissions for trauma.
Rates ranged widely across the United States. Wisconsin had the highest rate, while Alabama had the lowest—a more than sixfold difference in rates between the highest and lowest jurisdictions. From 2000 through 2020, rates for all age groups increased, with rates increasing the most for adults 85 and over for both men and women. Men had rates that were higher than women for all age groups, a difference that was largest in the 65–74 age group and narrowed with increasing age (Garnett et al., 2022).
Unintentional Fall Deaths in the United States, 2020
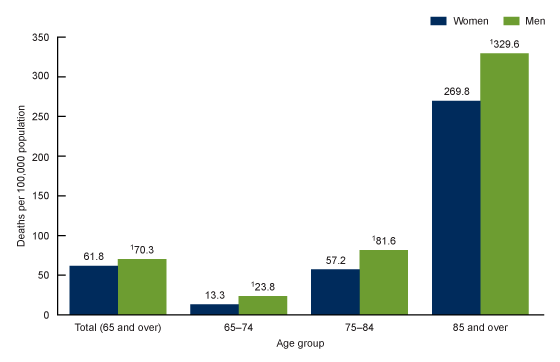
Rate of unintentional fall deaths for adults aged 65 and over, by age and sex: United States, 2020. Source: Garnett et al., 2022.
2.1 Hip Fractures
In adults over the age of 65, falls are the cause of more than 95% of hip fractures. Injuries such as these can cause severe health problems and lead to reduced quality of life and even premature death. Within a year after sustaining a hip fracture, an elderly nursing home resident has a 40% risk of death and a 6% to 12% risk of another hip fracture (CDC, 2016, September 20).
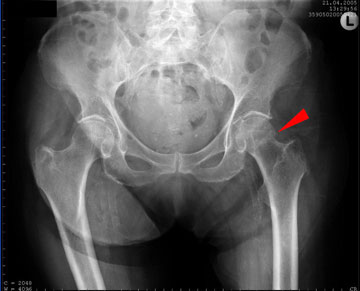
Medial hip fracture in a 92-year-old woman. Source: Wikimedia Commons.
On average, older adults with hip fractures are hospitalized for about one week. About one-quarter of adults who lived independently before their hip fracture will stay in a nursing home for at least a year after their injury.
In both men and women, hip fracture rates increase with age. People 85 and older are more likely to sustain hip fractures than are those age 60 to 65. Osteoporosis increases a person’s risk of sustaining a hip fracture because it weakens bones and makes them more likely to break.
2.2 Falls in Nursing Homes
About 1.6 million people 65 and older lived in nursing homes, representing about 5% of adults 65 and older. Falls are common and approximately half of residents fall annually. About 1 in 3 of those who fall will fall two or more times in a year (AHRQ, 2017).
Each year a typical nursing home with 100 beds reports 100 to 200 falls, although the number is probably much higher because many falls go unreported. About a third of fall injuries occur among residents who cannot walk.
2.3 Effects of Stroke on Fall Rate
Balance difficulties and falls are two of the serious medical complications for people who have experienced a stroke. During the first 6 months post stroke, falls are common compared with the annual fall rate in the general older adult population.
Studies that focus on post stroke safety and complications have identified an increased fall risk during acute hospitalization, which extend the length of the acute hospital stay. Approximately 5%–38% of patients fall at least once during their hospital stay (Inoue et al., 2023). Rates of falls remain high following discharge from the hospital.
Falls are an important issue during the acute stay, and fall prevention should be addressed immediately upon admission. Stroke severity, specifically a National Institutes of Health Stroke Scale (NIHSS) score ≥8, can be used to identify stroke patients who are at greatest risk of falling. Those determined to be at risk for falls should have a fall prevention program initiated while they are still in the acute inpatient hospitalization period (Schmid et al., 2010).
In a Canadian study, a lower score on the Berg Balance Scale (see later section on Assessing Functional Mobility and Gait) was associated with greater falls for both stroke and control groups. Researchers found that people recently discharged from rehabilitation to home were at greater risk for falls in their home. This may be because, following a stroke, people spend more time at home or are more cautious when outside their home. This finding reinforces the importance of a home assessment, home safety education, and environmental modifications as part of discharge planning (Simpson, 2011).
2.4 Psychosocial Consequences of Falls
Psychosocial factors are those factors related to social and psychological behavior. Social factors include marital status, living situation, and engagement in social activities, among others. Psychological factors include anxiety, worry, fear of falling, psychological trauma, and depression. Psychosocial factors can become barriers to improved outcomes, particularly if a provider makes inaccurate assumptions about the patient’s ability to follow up on recommendations and willingness to adhere to a complicated regimen.
In a structured interview of 816 men and women in northeast England (the Newcastle 85+ Study), researchers found that falls had significant psychosocial consequences. Those who sustained a fall “worried about falling” (42.0%), expressed “loss of confidence” (40.0%), and reported “going out less often” (25.9%). “Fear of falling” was reported by 42% of the study participants. Psychosocial consequences of falls were significantly more common in women, which suggests the need for gender-specific interventions in older adults (Collerton, 2012).
2.41 Fear of Falling
Experiencing a fall often increases an older adult’s fear of falling, which of itself is associated with future falls. Fear of falling leads older adults with and without a history of falling to restrict activities, leading to a decline in physical function, deterioration in perceived health status, increased depression, and increased risk for admission to institutional care (Freiberger et al., 2022).
Fear of falling in community-dwelling older adults can be widespread among those who have a history of falls as well as those who had not yet experienced a fall. The main risk factor for developing a fear of falling is a previous fall. Fear of falling increases with age and is more prevalent in women than men.
Risk factors associated with a fear of falling included:
- Osteoporosis
- Female gender
- Living alone
- Comorbidities
- Depression
- Impaired physical performance (Freiberger et al., 2022).
Fear of falling may also contribute to changes in gait. Older adults who fear falling tend to walk at a slower pace and have higher levels of anxiety and depression compared with adults who do not fear falling (Shumway-Cook and Woollacott, 2016).
2.42 The Long-Lie Condition
The “long-lie” condition, in which a faller is unable to get up and remains on the ground for several hours, is a consequence of falling that has social and psychological overtones. Even if no injury has occurred, many people who fall are unable to get up off the floor without assistance. Long-lies are associated with social isolation, fear of falling, muscle damage, pneumonia, pressure sores, dehydration, and hypothermia (Bagala et al., 2012).
Half of the older adults who experience a long-lie die within 6 months, even if no direct injury from the fall has occurred. More than 20% of older adults admitted to hospital as a result of a fall experienced a long-lie as a result of the fall (Bagala et al., 2012).
2.43 Protective Factors
Certain factors have been shown to have a protective effect against fall risk. This incudes providing clients and their caregivers with information and training on management of falls. Regular assessment of medications that may cause dizziness or vertigo, examination of eyesight and hearing, and thoughtful environmental modifications can significantly reduce the risk of falls in olde adults. Additional protective factor include:
- Regular physical activity
- Living in current residence for 5 or more years
- Having private health insurance
- Having a higher level of life satisfaction
- Engagement in social activities
