In 2005 the Joint Commission added the goal of “reducing the risk of patient harm resulting from falls” to its 2005 JCAHO National Patient Safety Goals (NPSG). The goals state that Joint Commission-accredited healthcare organizations must:
- raise awareness about falls
- establish an interdisciplinary falls injury prevention team
- use a standardized, validated tool to assess risk factors for falls
- implement interventions to reduce the risk of falls based upon the resident’s assessed risk
- standardize practices and interventions
- conduct post-fall evaluations
- report and analyze contributing factors
- continue to reassess each patient (Joint Commission, 2015)
A number of professional organizations have also recommended that older adults be assessed for fall risk. The American Geriatrics Society (AGS) encourages healthcare providers to ask all older adult clients about falls at least once a year. If an older adult patient has fallen within the last year, a gait and balance assessment is recommended. Those who cannot perform or who perform poorly on a standardized gait and balance test should be given a multifactorial fall risk assessment. The multifactorial fall risk assessment should include a focused medical history, physical examination, functional assessments, and an environmental assessment (USPSTF, 2018).
The World Falls Guidelines Task Force was created following discussions in 2019 between 14 international experts to consider whether new guidelines on falls prevention were needed to reflect new evidence and clinical service challenges. A systematic review identified gaps in, and inconsistencies between, the existing guidelines developed nationally or by specialist international bodies and concluded that a new set of clinical practice guidelines should be created to address these issues and that the guidelines should incorporate an international perspective. The world’s population is aging. Falls and related injuries are increasingly common, making their prevention and management a critical global challenge. Key points from the task force include (Montero-Odasso., et al, 2022):
- Many falls can be prevented. Fall and injury prevention needs multidisciplinary management.
- Engaging older adults is essential for prevention of falls and injuries: understanding their beliefs, attitudes and priorities about falls and their management is crucial to successfully intervening.
- Managing many of the risk factors for falls (e.g. gait and balance problems) have wider benefits beyond falls prevention such as improved physical and mental health, functioning, and quality of life.
- Estimates of risk of future falls can be done by trained clinicians with simple resources.
- Multidomain interventions (i.e., a combination of interventions tailored to the individual), when delivered, are effective for reducing the rate of falls in high-risk community-dwelling older adults.
- In care homes and hospital settings all older adults should be considered as high risk and a standard comprehensive assessment followed by multidomain interventions should be considered.
- Vitamin D supplementation to prevent falls should be reserved for those at risk of vitamin D deficiency.
- Modification to the approaches for assessment and interventions is needed for older adults with certain medical conditions associated with an increased likelihood of falling.
The Joint Commission has launched a Long Term Care Accreditation Program. When this voluntary program is fully implemented, accredited nursing homes will be required to comply with Joint Commission safety standards, including those related to prevention of falls.
5.1 Screening
Screening is a method for detecting dysfunction before an individual would normally seek medical care. Screening tests are usually administered to individuals without current symptoms but who may be at high risk for certain adverse outcomes. The purpose of screening is early diagnosis and treatment. Screening tools that address fall risk have been developed for use in various populations, including hospitalized older adults, adults in residential care, and community-dwelling older people.
Screening is an effective tool for quickly identifying patients at high risk for falling. But just as there is confusion about how to define a fall, finding an agreed-upon definition for “screening” is also fraught with problems. For example, some clinicians consider a check box on a form to be an adequate screen.
As an example of how the requirement to screen patients for specific behaviors or risks can create confusion, Medicare recently instituted a requirement that patients be screened for smoking. There are no parameters for how long, when, or what “smoking” means in this screen. The reason for the smoking screen is to provide education and, if warranted, to expand the examination based on the patient’s answer to the question.
The same problem occurs when screening for fall risk—if a patient is asked “Have you fallen in the last year?” and the answer is no, the screen leads nowhere, even in the case of an older adult patient who has real risk factors for falls. So it is important to observe the patient and have a screening tool that is quick and easy but also provides guidance about fall risk.
In fall intervention studies, age and history of falls are the two risk factors most commonly used to define high risk. Also considered are gender, impaired balance and gait, visual impairment, and use of multiple medications. A number of studies have indicated that a history of falls, use of certain medications, and gait and balance impairment are important indicators of the likelihood of future falls in older adults (USPSTF, 2018).
A practical approach for screening high-risk persons is to ask and assess: ask about history of falls, frequency and circumstances of falls, and mobility problems, then assess performance using a quick test such as a Timed Up and Go (TUG) test. The TUG test is performed by observing the time it takes a person to rise from an armchair, walk 10 feet, turn, walk back, and sit down again. The average healthy adult older than 60 years can perform this task in less than 10 seconds (USPSTF, 2018).
Recently a registered nurse received a comprehensive physical exam at a local clinic. Although she is 68 years old and is in the age category for fall risk, she was not asked about falls. There was a checkbox on the intake form asking “Have you fallen over the past year?” The patient answered no, even though she has fallen twice in the last year. Although she was examined by a doctor and a nurse practitioner, neither asked about falls. In this case, the checkbox on the intake form stopped the doctor from inquiring further even though the patient is in the age category for high risk and has two other risk factors: cataracts and stiff knees. When a clinician considers a checkbox on a form to be an adequate screen for fall risk a gap is created. In this case it failed to lead to some sort of action—patient education, a referral, or further assessment.
5.2 Brief Fall Risk Assessment
The Morse Fall Scale (MFS) is a brief fall risk assessment tool used widely in acute care settings. The MFS (Table 1) assesses a patient’s fall risk upon admission, following a change in status, and at discharge or transfer to a new setting. Prevention interventions are based on the Morse Fall Scale score (Table 2). Note that Morse herself said that the appropriate cut-points to distinguish risk should be determined by each institution based on the risk profile of its patients.
Table 1. Morse Fall Scale | |
|---|---|
| No = 0 Yes = 25 |
| No = 0 Yes = 15 |
| None, bed rest, wheel chair, nurse = 0 Crutches, cane, walker = 15 Furniture = 30 |
| No = 0 Yes = 20 |
| Normal, bed rest, immobile = 0 Weak = 10 Impaired = 20 |
| Oriented to own ability = 0 Forgets limitations = 15 |
Table 2. Recommendations Based on Morse Fall Scale | ||
|---|---|---|
Risk factor | MFS score | Action |
No risk | 0–24 | None |
Low risk | 25–50 | Initiate standard fall prevention interventions |
High risk | >51 | Initiate high risk fall prevention interventions |
5.3 Multifactorial Assessment
The multifactorial assessment is an assessment tool that offers a comprehensive look at fall risk. If, during a quick screening, an older adult has difficulty with balance or has unsteady gait, a multifactorial fall risk assessment should be completed. The multifactorial fall risk assessment should include a focused medical history, physical examination, functional assessments, and an environmental assessment.
Multifactorial interventions include an initial assessment of modifiable risk factors for falls and subsequent customized interventions for each patient based on issues identified in the initial assessment. The initial assessment could include a multidisciplinary comprehensive geriatric assessment or an assessment using a combination of various components, such as balance, gait, vision, postural blood pressure, medication, environment, cognition, and psychological health (USPSTF, 2018).
Nursing staff usually performs the assessment, and a number of different professionals perform subsequent interventions, including nurses, clinicians, physical therapists, exercise instructors, occupational therapists, dieticians, or nutritionists. Intervention components vary based on the initial assessment and could include group or individual exercise, psychological interventions, nutrition therapy, education, medication management, urinary incontinence management, environmental modification, physical or occupational therapy, social or community services, and referral to specialists (USPSTF, 2018).
Interventions for falls prevention can include:
- Modifying home environment
- Withdrawal or minimization of psychoactive or other medications
- Management of postural hypotension
- Management of foot problems and footwear
- Exercise (particularly balance), strength, and gait training
Mary Tinetti refers to the multifactorial assessment as an intervention that flows out of a fall risk screening. It is meant to put parameters around the issue of fall risk and is part of a continuum going back to the simple check box.
An older adult who does not have a history of falling, or who had a single non-severe fall and no gait or balance problems, is deemed as being at low risk. Since low risk does not mean "no risk at all", primary prevention is recommended for these older adults. This "low risk" group should be reassessed annually. Older adults who had a single non-severe fall but also have gait and or balance problems, should be considered as being at "intermediate risk" and would benefit from a strength and balance exercise intervention since evidence shows that this type of exercise is effective in reducing falls risk. Finally, those at "high risk" include older adults with a fall and one or more of the following characteristics: (i) accompanying injury, (ii) multiple falls (≥2 falls) in the previous 12 months, (iii) known frailty, (iv) inability to get up after the fall without help for at least an hour and (v) accompanied by (suspected) transient loss of consciousness (Montero-Odasso et al., 2022).
5.4 Medicare OASIS Fall Risk Assessment
The Centers for Medicare and Medicaid Services (CMS) requires Medicare-certified home health agencies to collect and transmit Outcome and Assessment Information Set (OASIS) data for all adult home health patients receiving skilled services, whose care is reimbursed by Medicare and Medicaid. The OASIS directs home health agencies to assess fall risk in all patients over the age of 65. The multifactorial assessment includes items such as falls history, use of multiple medications, mental impairment, toileting frequency, general mobility/transferring impairment, and environmental hazards (OEI, 2023). The purpose is to promote falls risk assessment across disciples and across healthcare settings.
CMS began collecting OASIS data for a new home health quality measure—the percentage of each home health agency's patients that experienced a fall with major injury—as part of its Home Health Quality Reporting Program in 2019. This quality measure helps a home health agency assess their efforts at improving patient care and safety and provides information for patients and their families as they select an agency (OIG, 2023).
Data analysis identified 39,900 falls with major injury and hospitalization among Medicare home health patients that had a matching OASIS assessment conducted between July 1, 2020, and June 30, 2021. Home health patients experienced the following major injuries because of these falls: 85% of falls resulted in a bone fracture, 9% resulted in a subdural hematoma, 11% resulted in a head injury with altered consciousness, and 1% resulted in a joint dislocation (OIG, 2023).
An assessment of data provided to CMS by U.S. home health agencies found that fifty-five percent of falls identified in Medicare claims were not reported in associated OASIS assessments as required. Falls reporting on OASIS assessments was worse among younger home health patients (compared to older patients) and patients who identified as Black, Hispanic, or Asian (compared to White). Reporting was also lower among for-profit HHAs as compared to nonprofit and government-owned agencies (OEI, 2023).
The Office of the Inspector General has recommended that CMS take steps to ensure the completeness and accuracy of the home health agency-reported OASIS data used to calculate the falls with major injury quality measure and use data sources, in addition to OASIS assessments, to improve the accuracy of the quality measure related to falls with major injury. They further recommend that CMS ensure that home health agencies submit required OASIS assessments when their patients are hospitalized and explore whether improvements to the quality measure related to falls can also be used to improve the accuracy of other home health measures (OIG, 2023).
5.5 Fall Risk Assessment in Nursing Homes
Falls are common in nursing facilities. Of the 1.6 million residents in U.S. nursing facilities, approximately half fall annually. About 1 in 3 of those who fall will fall two or more times in a year (AHRQ, 2017).
A falls management program includes two primary approaches to the management of falls and injuries. The first is assuring an immediate response to residents who fall. When a fall occurs, careful evaluation and investigation, along with immediate intervention during the first 24 hours, can help identify risk and prevent future incidents. The second approach is long-term management (AHRQ, 2017).
Screening at admission, quarterly, annually, and when a change of condition occurs are key in identifying residents at high risk of a fall. In both approaches, a comprehensive falls assessment should be used to develop individualized care plan interventions. Staff should monitor and manage the resident's response, making care plan revisions as needed. While both approaches are key to a comprehensive program, the burden on staff in terms of increased time and paperwork due to the high number of resident falls is significant. Facilities that master the fall response process can shift from crisis management to proactive reduction of fall risk and related injuries (AHRQ, 2017).
A Canadian study involving 137 nursing homes in the province of Ontario asked about what fall risk assessment tools were being used and tried to identify commonalities across the assessment tools. The most commonly used fall risk assessment tools were the Morse Fall Scale and the Performance-Oriented Mobility Scale. Across all facilities the common domains assessed included:
- Intrinsic factors
- Treatment-related or extrinsic factors
- Mobility status
- Cognitive status
- Sensory status
- History of falls
- Behaviors and attitudes (Wagner, 2011)
A particular barrier for quality improvement programs is that many do not fully address the ways in which staff duties overlap when attempting to address fall risk among their patients. Complex syndromes such as fall risk result from multiple risk factors and require multifactorial, interdisciplinary interventions to improve outcomes. Reducing multiple risk factors may be difficult because it requires many staff members to have strong connections that permit effective information flow and problem solving from varied perspectives; thus, an intervention is needed to help staff establish a working relationship and improved communication to support the new practices introduced by fall-reduction programs (Anderson et al., 2012).
5.6 Fall Classification Using a Mobile Phone
A novel way of documenting patient falls is through the use of mobile phones; most smart phones are equipped with accelerometers that can be used to detect when patients fall with exceptionally high accuracy. Falls are generally high-impact events, making detection simpler than identifying other daily activities. Automatically detecting falls can allow rapid response to potential emergencies; in addition, knowing the cause or manner of a fall can be beneficial for prevention studies or a more tailored emergency response.
A Rehabilitation Institute of Chicago study sought to demonstrate techniques that not only reliably detect a fall but also automatically classify the type. Fifteen subjects simulated four different types of falls—left and right lateral, forward trips, and backward slips—while wearing mobile phones and accelerometers. Nine subjects also wore the devices for ten days, to provide data for comparison with the simulated falls. Researchers were able to identify a fall with 98% accuracy and classify the type of fall with 99% accuracy (Albert, 2012).
Types of Falls Measured and Axes of Measurement
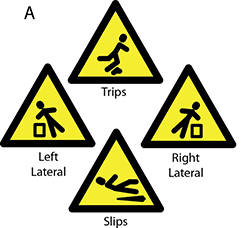


(A) Four different types of simulated falls, positioned according to direction of the fall. (B) The G1 android mobile phone that was used for recording, and the placement of the phone on the back of subjects. (C) The axes of the accelerometer. The phone was placed on the back of the subject so that the three axes pointed up, left, and to the back of the subject. Source: Albert, 2012. Used with permission.
This work demonstrates how current machine-learning approaches can simplify data collection as well as improve rapid response to potential injuries due to falls (Albert, 2012).
Back Next