In the U.S., there is an increase in suicides from age 15 to 54, a decrease until age 74, then an increase from age 75 to 85+ (SPRC, 2020). In Washington, suicide rates are highest among American Indian, Alaska Native, and White populations, consistent with national rates. But these broad demographic groupings can mask the impact of suicide in different subgroups. For example, the broad Asian population’s overall low suicide rate may hide the high impact of suicide in some Asian ethnic groups.
Most research studies are conducted in English and do not cover non-English speakers, so the viewpoints of non-English speakers are not captured. Lack of knowledge among mental health professionals on an ethnic group’s values, cultural traditions, and religious beliefs have been identified (Srinivasa et al., 2021).
2.1 American Indian and Alaska Natives
American Indian and Alaska Native (AI/AN) people are descendants of the original peoples of North, Central, and South America. The term AI/AN encompasses many ethnic and cultural groups, tribes, and traditions. In 2018, AI/AN populations comprised an estimated 1.3% of the U.S. population (SPRC, 2020).
American Indians and Alaska Natives face severe historical trauma, high rates of poverty and isolation, cultural taboos around death and suicide, and lack of access to mental healthcare (OMH, 2021, May 19). Among these populations, suicide rates peak during adolescence and young adulthood, and then decline through age 85+ (SPRC, 2020).
The suicide death rate for American Indian and Alaska Native populations is higher than that of the overall U.S. population for both males and females (SPRC, 2020). As in the U.S. overall, the suicide death rate for Native men is more than three times the rate for Native women (SPRC, 2020).
For youth aged 10 to 34 years, suicide is the second leading cause of death. The risk for co-occurrence of substance abuse, depression, and diabetes is over 12 times higher for American Indian and Alaska Natives than for Whites (Cwik et al., 2016).
Did You Know. . .
Suicide and suicide attempts are a significant problem in many American Indian and Alaska Native communities, especially among young men ages 15–24, who account for nearly 40% of all suicide deaths among natives (SAMSHA Tip 61, 2018).
While rates vary widely among tribes, some of the variables that seem to affect this elevated suicide rate include high rates of substance abuse, major psychiatric illnesses, and cultural alienation that can increase risk factors and lower protective factors for suicide. Geographically isolated reservations have limited educational and employment opportunities, as well as no easy access to mental health or substance abuse services (CSAT, 2017, latest available).
Suicide prevention and intervention efforts need to be tribe specific, emphasizing the cultural beliefs and practices unique to the tribe and recognizing the specific helping resources that are available and acceptable to that particular group. The involvement of the community in suicide prevention efforts is critical (CSAT, 2017, latest available).
2.2 White Populations
The age-adjusted suicide rate for White populations is higher than the overall U.S. suicide rate for both males and females. The pattern of suicide death rates among White populations increases from age 15 to 54, then declines. An increase occurs again from age 75 to 85+ (SPRC, 2020).
As in the overall U.S. population, the suicide death rate for White men is more than three to four times the rate for White women. Compared to the overall U.S. population, similar percentages of White adults reported past-year serious thoughts of suicide, a past-year suicide plan, or a past-year suicide attempt (SPRC, 2020).
Among White high school youth, the percentage of those who seriously considered attempting suicide and making a suicide plan is similar to the overall U.S. population. The percentages of White youth who attempt suicide requiring treatment is slightly less than the overall U.S. population (SPRC, 2020).
CDC data from 16 states show the most common circumstances around suicide for White men include mental and physical health problems, trouble in intimate relationships, alcohol dependence, and problems at work. Cultural taboos about seeking help and appearing vulnerable can isolate White men from both support systems and resources that could help (WSDOH, 2016).
2.3 Hispanic Populations
At 7.5 per 100,000, the 2020 age-adjusted suicide rate for Hispanic populations was significantly less than the overall U.S. suicide rate of 13.5 per 100,000. When Hispanic adults are compared to the overall U.S. population, similar percentages report past-year serious thoughts of suicide, a past-year suicide plan, or a past-year suicide attempt (SPRC, 2020).
Suicide rates remain somewhat steady starting at age 15 through the lifespan. This is a different pattern than is seen in the overall U.S. population, where suicide rates increase starting at in young and middle-aged adults, decline until age 74, and begin to increase at age 75. The suicide death rate for Hispanic men is more than four times the rate for Hispanic women (SPRC, 2020).
Among high school youth, a smaller percentage of Hispanic youth report seriously considering attempting suicide or making a suicide plan in the past year than the overall U.S. population. The percentage of youth who attempt suicide is similar to the overall U.S. population and a slightly higher percentage of Hispanic youth require treatment after attempting suicide (SPRC, 2020). Among youth and young adults, the prevalence of suicidal thoughts and behavior increases among Hispanics/Latinos who are more acculturated to mainstream American culture, particularly among females (CSAT, 2017, latest available).
2.4 Black Populations
In 2018 (latest available data), the suicide rate for Black/African Americans was 60% lower than that of the non-Hispanic White population. As in the overall U.S. population, the suicide rate for Black men was more than three times greater than for Black women (OMH, 2021, May 18).
Among Black/African American youth, suicide risk peaks in early twenties for males and late twenties for females. These patterns are very different from the age patterns of the White population and the whole population. In a study looking at suicide rates from 1983 to 2012 for African Americans, the risk of suicide in both genders showed a similar trend: the risk in males increased with age peaking at ages 20 to 24 years and then declined except for slight increases in older adults. For females, the risk increased with age until peaking at ages 25 to 29 years and then declined except for slight increases at middle age (Wang et al., 2016).
2.5 Asian Americans
The data classification for Asian Americans is very broad, creating huge gaps in the literature. There is lack of available data on risk factors, suicidal attempts, or incidence of suicides (Srinivasa et al., 2021).
Asians now make up about 7% of the U.S. population, and their numbers are projected to increase significantly over the next decades. The six largest Asian American subgroups in the U.S. are Chinese Americans, Indian Americans, Filipinos, and those who have roots in Vietnam, Korea, and Japan. These subgroups account for 85% of all Asian Americans in the United States (Pew Research Center, 2021).
Overall, the suicide rate for Asian Americans is about half that of the national rate. However, most national suicide mortality data combine people of Asian, Native Hawaiian, and other Pacific Islander descent into one group that is usually called Asian or Pacific Islander (SPRC, 2020).
Among Asian subgroups, Korean males had more than twice the frequency of death due to suicide (5%) compared to non-Hispanic Whites (2%), and suicide was ranked as the fifth leading cause of death, higher than every other Asian subgroup and non-Hispanic Whites. Mortality rates for suicide among Korean males were twice that of any other Asian subgroup (Hastings et al., 2015).
Depression is four times more likely to prompt suicidal behavior among Asian youths compared to other ethnic groups. Parental conflict is a major factor for suicidal attempts and suicide in Asian origin adolescents. In a study of Indian immigrants, it was reported that children 15 or older had higher incidences of suicide after they migrated to other countries than when they lived in India (Srinivasa et al., 2021).
2.6 Native Hawaiian/Pacific Islanders
People who are descended from any of the original peoples of Hawaii, Guam, Samoa, or other Pacific Islands are referred to as Native Hawaiian or Other Pacific Islander (SPRC, 2020). In 2019, suicide was the leading cause of death for Native Hawaiians/Pacific Islander young adults. Native Hawaiians/Pacific Islanders are less likely to receive mental health services or to receive prescription medications for mental health treatment as compared to non-Hispanic whites (OMH, 2021, May 20).
The Pacific Islands have some of the highest rates of suicide in the broader Western Pacific Region. These areas are experiencing complex and rapid societal change, including loss of culture and spiritual connectedness due to the impacts of climate change and Westernization. These external factors have been linked to helplessness, poor wellbeing, and suicidal behaviors (Mathieu et al., 2021).
The World Health Organization's recent global health estimates for 2000-2019 include age-standardized suicide rates for eight Pacific Islands, with Kiribati, Federated States of Micronesia, and Vanuatu having the highest rates, and several exceeding the current global age-standardized rate of 9.0 per 100,000 (Mathieu et al., 2021).
Overall, the most common methods for both suicide and suicide attempts were self-poisoning and suffocation/hanging. The higher prevalence of self-poisoning in suicides and suicide attempts in the Pacific Islands has been linked to access. Specifically, limited access to other means such as firearms may influence higher rates of hanging, and easy access to lethal pesticides in rural areas of the islands or prescription medications may influence the selection of these methods (Mathieu et al., 2021).
Young people are a vulnerable group across the Pacific Islands. This has been linked to social change, rapid urbanization and Westernization, and a rise in social disintegration. This disintegration has forced young people to navigate the complex divide between traditional roles and social structures. While other countries have higher suicide rates in older ages, the current findings are comparable with Indigenous peoples worldwide (Mathieu et al., 2021).
2.7 Suicide vs. Homicide
Suicides continue to outnumber homicides in America. For youth in the U.S. between the ages of 10 and 17, the number of suicide victims changed little in 2020 while the number of homicide victims increased 47%. The suicide rate increased for Black and Hispanic youth in 2020 but decreased for White youth (OJJDP, 2020).
In the U.S., firearms are involved in almost 80% of all homicides and more than half of all suicides. The increases in firearm homicide rates and persistently high firearm suicide rates in 2020, with increases among populations that were already at high risk, have widened disparities and heightened the urgency of actions that can have immediate and lasting benefits (Kegler et al., 2022).
2.8 Gender and Age Differences
Worldwide, about 80% of the nearly one-million suicide deaths recorded each year are among men (Seidler et al., 2021). Male deaths by suicide outnumber those by women in every country in the world. Although women make twice the number of suicide attempts, men are more likely to die by suicide (Richardson et al., 2021).
Men are more likely to use deadlier methods, such as firearms or suffocation while women are more likely than men to attempt suicide by poisoning (WSDOH, 2016). Unfortunately, among women, the rate for firearm-related suicide has increased since 2007. Firearm-related suicide became the leading means for women in 2020 (NCHS, 2022, March 3).
In men, signs of suicidal ideation include social withdrawal, anger, and reduced problem-solving capacity. Signs of suicide attempt include statements of suicidal intent, calmness, anger, apathy, hopelessness, risk-taking, and appearing “at peace.” Signs preceding death by suicide include desperation and frustration in the face of unsolvable problems, helplessness, worthlessness, statements of suicidal intent, and emergence of a positive mood state (Hunt et al., 2017).
Men 75 and older had the highest rate, while men 45 to 64 had the highest total number of suicides. External economic factors were involved in more than a third of suicides. For elderly men, contributing factors include economic insecurity, loss of significant relationships, loneliness, fear of being a burden, and the physical and mental stresses of aging (WSDOH, 2016).
Among young people in Washington, suicides have received a great deal of media and community attention, though suicide rates for adults are higher (Srinivasa et al., 2021). A 2023 Healthy Youth Survey in Washington that included 217,000 students in grades 6-12, indicated that a significant percentage of students reported feeling anxious, nervous, on edge, and unable to stop worrying (HYS, 2024).
Among 10th graders, 30% reported persistent depressive feelings, and nearly 15% reported contemplating suicide. While this is an unacceptable level of youth struggling with suicidal thoughts, it is also the lowest rate we have seen in Washington in 20 years (HYS, 2024).
Non-suicidal self-injurious behavior such as cutting, burning, hitting oneself, scratching oneself to the point of bleeding, or interfering with healing is a relatively frequent behavior in young people. The concern is that it these behaviors can become chronic and evolve into other forms of self-injurious behavior, such as suicide attempts (Grandclerc et al., 2016).
Because non-suicidal self-injurious behavior and suicidal behavior often occur together, it is important to consider the nature of the link between these two types of behavior. Some specialists see non-suicidal self-injurious behavior as a means of regulating negative emotions, while others argue that it is a factor in the emergence of suicidal ideation and attempts (Grandclerc et al., 2016).
Suicide Rates by Sex in the United States (2000–2020)
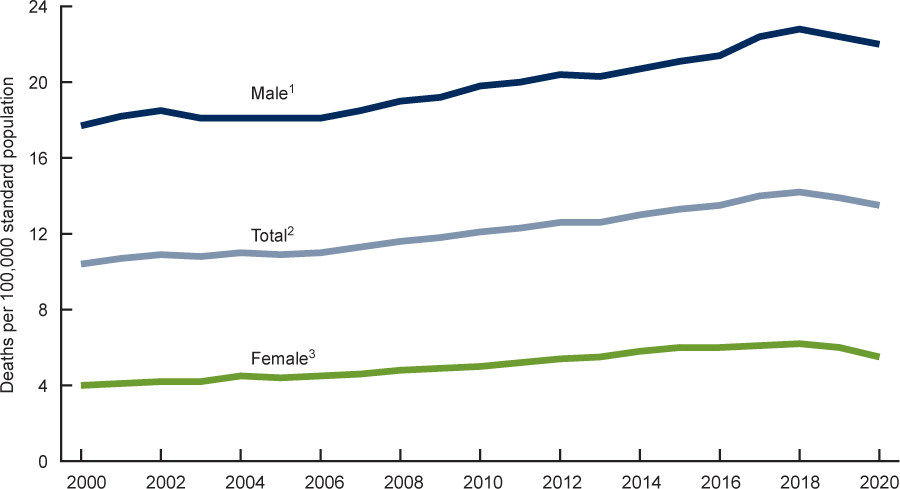
1Stable trend from 2000 through 2006, significant increasing trend from 2006 to 2018, stable trend from 2018 through 2020, p< 0.05. The rate in 2020 was significantly lower than the rate in 2018, p< 0.05.
2Significant increasing trend from 2000 through 2018, with different rates of change over time; significant decreasing trend from 2018 through 2020, p<0.05.
3Significant increasing trend from 2000 through 2015, with different rates of change over time; stable trend from 2015 through 2018; significant decreasing trend from 2018 through 2020, p<0.05.
Notes: Suicide deaths are identified using International Classification of Diseases, 10th Revision underlying cause-of-death codes U03, X60–X84, and Y87.0. Age-adjusted death rates are calculated using the direct method and the 2000 U.S. standard population.
Source: CDC, 2022, March 3.
