Damage done by COPD to airways and the lungs is not reversible. Although currently there is no medical cure available for lung tissue damage, adopting regular medical care and consistent lifestyle changes can help slow the progression of the disease.
Goals of Management
The major goals of COPD treatment are:
- Relieve symptoms
- Slow the progression of the disease
- Improve exercise tolerance
- Prevent and manage complications
- Improve overall health
Patients with newly diagnosed COPD should have a followup appointment in 4 to 6 weeks to assess for adherence as well as any problems with the new medication. They should also be referred to a smoking cessation program, counseling, or support group. In every state, the 1-800-Quit-Now phone number is a helpful resource. At each and every visit the patient should be questioned about smoking cessation progress to either celebrate triumphs or be encouraged with resources to stop smoking.
A cardiopulmonary rehabilitation referral is also appropriate per practice guidelines at Stage II COPD. A quarterly visit for the first year is appropriate because the patient needs to be referred for an annual flu shot and education regarding inhalers, spacers, and equipment. Education by referral may be needed if it is not provided in the office of the primary care provider.
Initial Management
At patients’ initial visits, the healthcare provider should initiate a conversation about the possible causes for their clinical presentation. A simplified list of differential diagnoses can be shared with the patient before any diagnostic test is ordered. This lays the foundation for patients’ understanding that they are part of the healthcare team in making decisions about their own plan of care. Patients should be given the opportunity to share opinions and choices within the recommendations for the standard of care.
The current GOLD Standards are established by numerous research studies and the CDC, and include the following:
- The Global Initiative for chronic obstructive lung disease (GOLD) is the standard for diagnostic and treatment guidelines.
- General interventions are comfort measures based on the severity of the symptoms and causative factors.
- Smoking cessation should be mandatory because it is the number one causative factor. Smoking cessation should be discussed at every visit.
- The selection of inhalers depends on the age of the person.
- Nutrition management should be included because 25% of COPD patients are malnourished; eating competes with breathing so meals are limited. Encourage higher calorie supplements such as Ensure to deliver needed nutrients.
- Pharmacologic therapy is based on spirometry and stage of disease. For stage I, short-acting bronchodilators (SABA) are prescribed as needed for shortness of breath. For stage II, a SABA plus a long-acting bronchodilator (LABA) should be prescribed. The stage III patient should have a SABA, LABA, plus an inhaled glucocorticoid if the patient has frequent exacerbations. Stage IV patients need all given in stage III plus cardiopulmonary rehabilitation and possibly O2 delivery. All patients should receive an annual flu vaccine, one pneumonia vaccine after age 65 (and every 5–10 years for high risk patients) (Grossman & Porth, 2014).
Oxygen Use
Because the issue with COPD is decreased air flow, the main goal of therapy is to help the patient’s lungs provide sufficient oxygen to the body. If the patient is short of breath, hypoxemic,* or has obvious signs of heart failure, oxygen should be titrated to saturation levels ≥93% (Jarvis, 2015).
* Hypoxemia vs. hypoxia. Hypoxemia is abnormally low arterial oxygen tension (PaO2) in the blood (hence the -emia ending). Hypoxia a condition of under-oxygenation, which is an inadequate level of tissue oxygenation for cellular metabolism. Hypoxemia frequently results in hypoxia—but not always!
A concern is oxygen toxicity and vasoconstriction. Oxygen causes constriction of the coronary, cerebral, renal, and other key vasculatures. If perfusion decreases with blood hyper-oxygenation, the administration of oxygen may place tissues at increased risk of hypoxia. Hyperoxia reduces coronary blood flow by 8% to 29% in normal individuals and in patients with coronary artery disease or chronic heart failure.
Although oxygen supplementation is a modality used only in the end stages of COPD, it is still a fundamental intervention. Care must be taken when giving oxygen to patients with COPD because their drive for inhalation is based on carbon dioxide retention, which they become used to. If additional oxygen is given, it may decrease the drive to breathe and further complicate oxygenation.
Online Resource
Video [7:33]: Management and Treatment of COPD
https://www.youtube.com/watch?v=9-ErVE--vjM
Patient Education
It is essential that patients be taught about the possible cause of their COPD, and their own treatment plan, so they can understand the importance of being a member of the care plan team. Modification of triggers should be taught first—notably cessation of smoking, alcohol, and caffeine. Behavioral lifestyle changes include weight loss. Patients need to know that COPD is a chronic disease and there is no cure. Advance directives should be taught and put in place. The following actions are recommended:
- Give the patient a prescription for antibiotics to be filled upon worsening of symptoms, according to the GOLD standard.
- Teach patients to conserve their energy and plan for activity.
- Teach patients how to use a peak-flow meter at home to measure their breathing ability and to alert their provider if they reach the red target zone.
- Teach the COPD action plan and encourage them to become active participants in their own care. (Glass, 2014)
Therapeutic Lifestyle Changes
With commitment and perseverance, a person can significantly reduce the deterioration of respiratory function of COPD. The categories of therapeutic lifestyle changes that have been scientifically demonstrated to be good treatments for COPD—namely, smoking cessation, maintaining habits of healthy living that include eating a diet low in saturated fat and high in fruits and vegetables, exercising daily, and losing weight (if relevant).
The job of the healthcare team is to work with the patient to personalize these familiar recommendations. Healthcare providers must offer practical advice that the patient can reasonably follow and that the patient believes is worth following.
Smoking Cessation
Lifestyle changes begin with smoking cessation. Carbon monoxide and other poisons in cigarette smoke damage many types of cells in the body. Carbon monoxide also reduces blood oxygenation, stressing the oxygen-hungry heart. This stress is compounded by the nicotine in cigarette smoke. Nicotine constricts blood vessels and causes the heart to work harder, raising heart rate and blood pressure—two effects that increase the heart’s workload (Mitchell & Schoen, 2009).
Smoke-Free T-Shirt

Source: smokefree.gov.
Cigarette smoking accelerates coronary atherosclerosis in both sexes and at all ages, and increases the risk of thrombosis, plaque instability, MI, and death. In addition, it aggravates angina by increasing myocardial oxygen needs and reducing oxygen supply (NIH, 2016).
People who stop smoking reduce their risk of death from CAD from 35% to 50%; however, most people find it difficult to stop smoking. Clinicians can begin by telling patients that continued smoking increases their risk of serious heart problems and death, while quitting reduces this risk. They should then ask patients who smoke if they have thought about quitting. Whatever the answer, clinicians should follow with the offer, “When you would like to stop smoking, I’ll be happy to work with you to set up an effective program.”
Recommended Therapeutic Lifestyle Changes
- Less than 7% of daily calories should come from saturated fat. This kind of fat is found in some meats, dairy products, chocolate, baked goods, and deep-fried and processed foods.
- No more than 25% to 35% of daily calories should come from all fats, including saturated, trans, monounsaturated, and polyunsaturated fats.
- Cholesterol intake should be less than 200 mg a day.
- Foods high in soluble fiber help prevent the digestive tract from absorbing cholesterol. These foods include:
- Whole-grain cereals such as oatmeal and oat bran
- Fruits such as apples, bananas, oranges, pears, and prunes
- Legumes such as kidney beans, lentils, chick peas, black-eyed peas, and lima beans
- Choose a diet rich in fruits and vegetables to decrease cholesterol. Compounds called plant stanols or sterols, work like soluble fiber.
- Fish such as salmon, tuna (canned or fresh), and mackerel are a good source of omega-3 fatty acids and should be eaten twice a week.
- Limit sodium intake. Choose low-salt and “no added salt” foods and seasonings.
- Limit alcohol intake. Too much alcohol raises blood pressure and triglyceride levels, and adds extra calories.
- Men should have no more than two drinks containing alcohol a day.
- Women should have no more than one drink containing alcohol a day. (NHLBI, 2006)
Many patients with COPD have concomitant CAD and heart risk factors. Nutrition for them must be tailored to meet their caloric needs. In the early stages of COPD, a cardiac diet is recommended; however, if a patient loses too much weight and becomes weak and cachectic, foods high in calories that are easy to consume, such as shakes and liquid nutritional supplements, should be offered.
Physical Activity
Regular exercise helps to reduce extra weight, stimulate the circulatory system, improve oxygen flow to the lungs, and promote mental alertness. However, when COPD becomes moderate to severe, simple physical activities such as walking to the door or even getting dressed can create dyspnea. Modifications in an exercise plan must be considered to conserve energy.
Exercise programs may have to be introduced gradually. At first, patients with moderate to severe COPD may be limited by the occurrence of dyspnea and will probably need to adapt even their normal activities. The appearance of chest pain or shortness of breath equivalents indicates that an activity is too strenuous, so patients should revise their normal activities to accommodate to their energy level.
Mass Reduction: Weight Loss
During the past twenty years, there has been a dramatic increase in obesity in the United States and rates remain high. Thirty-five percent of U.S. adults and approximately seventeen percent (12.5 million) of children and adolescents aged 2 to 19 years are obese. Obesity-related conditions include heart disease, stroke, type 2 diabetes, and certain types of cancer, some of the leading causes of preventable death (CDC, 2015, CDC, 2016).
Excess body weight makes the heart and lungs work harder, and excess fat fosters atherosclerosis. A person is considered overweight if their body mass index (BMI, see chart below) is 25 to 29.9 kg/m2, while obesity is defined to be BMI >30 kg/m2.
Calculating BMI is one of the best methods for population assessment of overweight and obesity. Because calculation requires only height and weight, it is inexpensive and easy to use for clinicians and for the general public. The use of BMI allows people to compare their own weight status to that of the general population. The standard weight status categories associated with BMI ranges for adults are shown in the following table (CDC, 2016).
BMI Chart

Source: Courtesy of webmd.com.
Weight management is a key part of the therapeutic lifestyle changes recommended for people with COPD. Patients should be encouraged to maintain a BMI <25 kg/m2. Men should aim for a waist circumference <102 cm (40 in), while women should aim for a waist circumference <89 cm (35 in) (CDC, 2016). To measure waist size correctly, one should stand and place a tape measure around the middle, just above the hipbones and measure the waist just after breathing out.
Low-carbohydrate diets (<130 g carbs/day) seem to be about as effective and safe as low-fat diets. The most effective way to lose weight and to maintain the lower weight is participation in a comprehensive weight-loss program that combines diet, behavior modification, and regular exercise. Healthy weight loss must include a lifestyle of long-term changes in daily eating and exercise habits.
Evidence shows that people who lose weight gradually and steadily (about 1 to 2 pounds per week) are more successful at keeping weight off. In order to lose weight, a person must reduce their daily caloric intake and use up more calories than taken in. Since 1 pound equals 3,500 calories, caloric intake must be reduced by 500 to 1000 calories per day to lose about 1 to 2 pounds per week (CDC, 2015).
Even a modest weight loss—5% to 10% of total body weight—is likely to produce health benefits such as improvements in blood pressure, blood cholesterol, and blood sugars. Long-term success is achieved through healthy eating and physical activity most days of the week (about 60–90 minutes, moderate intensity) (CDC, 2016).
Management of Stress
For those with asthma and COPD, management of stress is needed to decrease the work of breathing. For many people with asthma, a psychological trigger such as a stressful event or even the fearful anticipation of a stressful event can trigger an acute asthmatic attack.
Test Your Knowledge
What are some general lifestyle recommendations for COPD?
- Smoking cessation, nutrition, and weight control.
- High fat diet to provide calories.
- Low fat and calorie diet to lose weight.
- Low salt diet.
Answer: A
Medications
Medications are used to manage all forms of COPD and may be used as monotherapy, dual therapy, or multi-drug therapy per the GOLD Guidelines for COPD control and management. The two main categories of medications that open the airways are the beta-2 bronchodilators, which can be remembered with the pneumonic BAM:
B bronchodilators,
A anticholinergics such as ipratropium, and
M methyl xanthines that stimulate the bronchioles to open, such as theophylline.
The second class of medications are the anti-inflammatories, which can be remembered by the acronym SLM:
S steroids,
L leukotrienes, and
M mast cell stabilizers.
|
Drug class |
Action |
Brand names |
|
Bronchodilators |
||
|---|---|---|
|
Beta 2—Short acting (SABA) |
Dilate bronchi |
Albuterol (rescue inhaler) |
|
Long Acting Beta Agonists (LABAs) |
Act on Beta 2 receptors to bronchodilate |
Advair, Serevent, Foradil, Oxis, Salmeterol, Formoterol |
|
Short Acting Beta Agonists (SABAs) |
Act on Beta 2 receptors to bronchodilate |
Albuterol, Ventolin, Proventil, Spiriva |
|
Anticholinergics/Antimuscarinics (LAMA) |
Increase sympathetic system to open airways |
Ipratropium, tiotropium |
|
Methylxanthines |
Beta 2 stimulation to open bronchioles |
Aminophyllin, Theophyllin, Unidur, Theodur |
|
Anti-inflammatories |
||
|
Steroids (Inhaled Corticosteroids) |
Decrease inflammation in the lower airways |
Fluticasone, Advair, Flovent, Pulmicort, Symbicort, Asmanex, Alvesco, mometasone |
|
Steroid (Nasal) |
Decrease inflammation in the upper airways |
Nasonex, Nasacort, Veramyst |
|
Leukotriene Antagonists (LTRAs) |
Non-steroidal anti-inflammatory |
Singulair, Accolate |
|
Allergy Medications |
Antihistamine |
Xolair, Claritin/Clarinex, Allegra, Zyrtec |
|
Mast Cell Stabilizers |
Decrease release of histamine |
Cromolyn |
|
Phosphodiesterase-4 PDE-4 Inhibitors |
Suppress inflammation |
Roflumilast |
Recall that the physiology of the airways is largely controlled by two main nervous system receptors, the muscarinic and beta receptors, and blocking the muscarinic or stimulating the beta receptors will increase the airways.
A way to remember the different kinds of medication used for COPD is to remember the drug name endings:
- The muscarinic antagonist drugs end in “ium” (ipratropium, tiotropium, and UM clidinium).
- A new drug called glycopyrrolate is a muscarinic, so drugs that ends in “ate” will remind you that the drug “ate” the effects of muscarinic receptors.
- All of the respiratory beta agonist drugs end in “ol” (similar to cardiac beta blockers ending in “ol”). Drugs such as formoterol, salmeterol, and albuterol are beta agonists and increase the airway diameter.
- The inhaled corticosteroids end in “one” (fluticasone, mometasone).
COPD vs. Asthma Protocols
A medication grid can help you remember the progression of adjunct medication for both COPD and asthma.
|
Medication Endings Grid for COPD and Asthma |
||||
|---|---|---|---|---|
|
COPD |
LAMA |
LABA |
ICS |
Asthma |
|
→SABA |
“ium” |
“ol” |
“one” |
←SABA |
Notice in the grid that, whereas treatment for COPD starts on the left (LAMA) and moves toward the right, asthma begins with an ICS and moves to the left in terms of adjunct medications.
Advancement of treatment depends on the frequency of the use of the SABA (rescue inhaler). Someone with COPD who is using a SABA more than 2x/week would advance from a LAMA to adding on a LABA and then later to the third class of medication, the ICS. If the patient with COPD or asthma is not using the rescue inhaler (SABA) more than two times weekly, then they do not need to advance in medication treatment.
In contrast, someone with asthma who is using the SABA (rescue inhaler) more than 2x/week would add only an ICS medication, advance to the LABA, and then last add the LAMA.
To summarize from the grid: For asthma, the first medication to use after the SABA is the ICS. Asthma patients will never use a LABA without using the ICS. The last medication to use for asthma is a LAMA. For COPD, the first class of medication to use after the SABA is the LAMA, with advance to the LABA, and finally to the ICS. Many pharmaceutical companies offer dual combination therapies for ease of use.
Inhaled Medications
Each of the drugs discussed above is available as an inhaled medication—in metered dose, breath-activated, or oral form.
An Asthma Inhaler
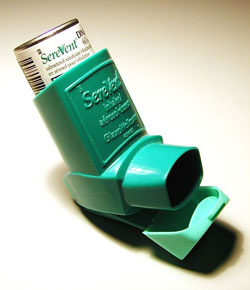
Source: Wikimedia Commons.
Inhaled medications for COPD use different mechanisms to open the airways. Spacers may be used to enhance the drug delivery. Nebulizers can also be used for oxygen, or oxygen can be added through a liquid drug via a face mask. Many of these medications can be given intravenously for critically ill patients. Each class of medications is described below.
Bronchodilators
Inhaled bronchodilators are the key medications to opening the airways because they act on the beta receptors of the bronchiole tubes to cause bronchodilation. Bronchodilators relax the smooth muscles around the bronchioles, which dilates the air tubes, allowing more air to pass through.
Most bronchodilators are taken with inhalers so the medication goes directly to the airway. Both short-acting bronchodilators (SABA) and long-acting bronchodilators (LABA) work directly on opening the airways. The short-acting agonists are for an acute exacerbation when the airway closes suddenly, whereas the long-acting bronchodilator agonists (LABAs) are to be taken daily on a regular schedule to maintain the patency of the airways. Generally, SABAs are more expensive than LABAs. Each has a rapid onset of action and can be used symptomatically or before exercise.
Short-acting beta-2 agonists work within several minutes for a duration of 3 to 5 hours, as compared to long-acting beta-2 agonists, which last 12 hours. Each has side effects similar to drugs that mimic the sympathetic system, including fine tremors, muscle cramps, nervous tension, palpitations, tachycardia, sleep disturbances, hypokalemia, and occasionally paroxysmal bronchospasm.
Anti-Muscarinics/Anti-Cholinergics
This class of medications causes bronchodilation and reduces mucus secretion by blocking muscarinic receptors in the lung. These drugs have a longer action and greater bronchodilator effect than the beta-2 agonists and are used in both COPD and asthma. Side effects include dry mouth, nausea, and constipation, and they can cause urinary retention (so must be used with caution for those patients with bladder problems and also those with glaucoma). Short-acting anti-muscarinics can be inhaled or nebulized and include ipratropium. The long-acting tiotropium can only be given by an inhaler.
Methylxanthines
This class, which includes theophylline, stimulates the beta-2 receptors on the lungs to allow bronchodilation. It can be given orally or intravenously. This class works by inhibiting phosphodiesterase or blocking adenosine. It is often given in acute asthma. Side effects include gastrointestinal upset, cardiac palpitations, tachycardia, arrhythmias, headache, insomnia, and convulsions.
Steroids
Inhaled corticosteroids (ICS) are generally the second adjunct therapy suggested by the GOLD Guidelines. They help reduce inflammation in the airways and lungs. Inhaled steroids should not be used as monotherapy but in combination with a bronchodilator. Because this class is a steroid, it may increase blood sugar levels and complicate control for patients who also have diabetes. This class of medications also may cause oral thrush because the oral inhaler delivers glucocorticoids directly to the mouth. It is recommended that this class of oral inhaler be given last for COPD and then the mouth be rinsed immediately after ingestion. As we have seen, it is often the first class of medications for asthma after short-acting bronchodilators and the same caution applies.
Steroids can be given via various routes including inhalation (beclometasone, budesonide), orally in the form of prednisolone, and IV in the form of hydrocortisone.
Systemic side effects of long-term corticosteroids are numerous and affect every body system. In the endocrine system we see blood sugar levels rise; in the musculoskeletal system, myopathy; neurologically, there can be growth retardation and psychiatric disturbances; in the integument, impaired wound healing, sodium and water retention; finally, glaucoma and central redistribution of fat are other common side effects.
Leukotriene Receptor Antagonists
This class of drugs is used to block the effects of leukotrienes, which would normally stimulate the mast cells to release histamine. When histamines are released, vasodilation and fluid movement to the site are natural reactions of the inflammatory response, which is the cause of many symptoms of COPD. In blocking this reaction, lungs may have less mucus build-up and air can move more easily in ventilation. Omalizumab (Xolair) is given orally; it is an anti-IgE monoclonal medication and is used in severe cases of asthma (but it is very expensive). Side effects include gastrointestinal disturbances, headache, insomnia, arthralgias, myalgias and, rarely, bleeding disorders.
Phosphodiesterase-4 (PDE-4) Inhibitors
If COPD symptoms continue, this class of medication may be added. It is the newest class of medications and suppresses inflammation in the airways.
Pulmonary Rehabilitation
Pulmonary rehabilitation includes the combined efforts of a customized exercise program, nutrition counseling, disease management training, and psychological counseling. The goal is to help reduce symptoms and minimize acute exacerbations.
Surgical Interventions
Lung-volume reduction (LVR) surgery is not used to “cure” COPD but is used to remove damaged lung tissue, which allows better expansion of the remaining lung tissue. Lung transplantation, the replacing of a damaged lung with a donor lung carries additional risks of rejection and infection.
Followup and Evaluation
The followup may be simply a return to clinic if symptoms worsen. COPD patients should be monitored regularly, beginning with every 3 months, then 6 months, and then at least annually. Referrals to a pulmonologist are necessary if symptoms persist or worsen. Monitoring levels of serum theophylline, which has a very narrow therapeutic range, before each visit can help the clinician to modify the medication regimen and avoid adverse effects.
Mark, our 62-year-old patient, was given a medication regimen and referred to a smoking cessation program. Mark wanted to try to quit smoking on his own. If unsuccessful, he was willing to try a nicotine patch. He was also given a short-acting beta agonist and a rescue inhaler and was taught how to use it for episodes of shortness of breath. In addition, Mark was given a long-acting antimuscarinic, ipratropium, in an Atrovent inhaler to be taken daily.
Mark would return to the clinic in 1 month to evaluate his symptoms and progress. He would continue to be followed every 3 months for progress toward smoking cessation and control of symptoms. He is slated be seen annually to review the PFT (pulmonary function test) and assess for any new complications and to provide education, prophylactic antibiotics, and a flu shot.
Online Resource
Video [2:17]: How to Use a Metered Dose Inhaler
https://www.youtube.com/watch?v=fHYTz-ZoRLw
Test Your Knowledge
What are the most common side effects for bronchodilators?
- Fatigue, lack of appetite, and urinary incontinence
- Nausea, vomiting, and diarrhea
- Restlessness, tachycardia, and heart palpitations
- Muscle pain and hypotension
What class of medications decreases inflammation seen in COPD?
- Bronchodilators
- Anticholinergics
- Steroids and leukotriene receptor antagonists
- Methylxanthines
In addition to a short-acting bronchodilator (rescue inhaler), which medication class is generally the first line of therapy for patients with asthma?
- Inhaled corticosteroid
- Long-acting bronchodilator
- Anticholinergic
- Mast cell stabilizer
Answers: C,D,A
