Cognitive decline, as well as sensory changes in vision, hearing, and proprioception* increase the risk of accident and injury in older adults with dementia. Increasingly, technology has become a potential resource for improving safety and supporting independence.
*Proprioception: a sense or understanding of the position and movement of our bodies in space.
Assistive technologies are fast becoming a fundamental pillars of health strategies. They include any product or technology-based service that enables people of all ages with activity limitations in their daily life, education, work, or leisure (Pappadà et al., 2021).
For people with dementia, assistive technologies—such as GPS devices—can increase autonomy and reduce the risks associated with wandering. They can also support and sustain people's cognitive abilities—those required to accomplish necessary daily activities (Pappadà et al., 2021).
Assistive technologies and devices can delay institutionalization or reduce the number of severe clinical cases requiring admission to care homes. Technology can also be useful when a person with dementia is admitted—it can allow for easier communication between residents and relatives and help a person overcome social barriers (Pappadà et al., 2021).
14.1 Prevention
Many caregivers (as well as healthcare providers and workers) fail to recognize the importance of prevention when caring for older adults living with dementia. Creating a safe environment supports person-centered care, encourages independence, and reduces caregiver burden.
Safety is a joint responsibility, which should cover environmental safety, infection prevention, emergency procedures, handling of hazardous materials and chemicals, and creation of a disaster plan. The building’s design should include safety features such as grab bars, ramps, wandering paths with ample seating, standing stations for exercise and stretching, and features that encourage independence while also ensuring safety.
Preventable deaths can be cause by poisonings, falls, choking, drowning, and home fires. For someone with dementia, isolation, decreased mobility, and polypharmacy are also safety concerns. Medication management is often overlooked as a safety issue even though many medications affect balance, cognition, and judgement. Medical issues such as urinary urgency, constipation, skin breakdown, anxiety, and depression can lead to injuries and accidents if not properly managed.
14.2 Elements of a Safe Environment
Safety is the ability to keep a person safe from harm. A safe environment is one in which a person is protected from anything that is likely to cause injury. Caregivers must (1) think prevention, (2) adapt the environment, and (3) minimize dangers.
Specialized adult day care centers must consider the safety needs unique to a clientele experiencing cognitive decline. This means the center must address wandering, falls, aggressive behaviors, swallowing disorders, food preferences, and transportation safety. Centers can also enhance safety by providing caregiver training and information about assistive equipment, transfer techniques, and safety planning in the home.
A day care center can provide a feeling of safety for clients and their family members. In a Norwegian study involving 17 family caregivers of people with dementia who attended an adult day care program, caregivers described the center as a service that represented something safe and routine for the person with dementia. Family caregivers reported feeling a sense of relief and shared responsibility because the day care center addressed social and nutritional needs, while providing physical activity, structure, and variety for the person with dementia. Caregivers reported feeling feel safe because staff knew their loved one’s situation and condition and provided information about other relevant resources in the community (Tretteteig et al., 2017).
14.3 Technologies Related to Safety
Technologies that support a safe environment for people with dementia can be grouped into three overlapping categories:
- Devices used for prompts and reminders.
- Devices that support communication and reminiscence.
- Devices used to monitor activity, movement, and location.
Care homes tend to favor technologies used “on” residents, primarily to enhance safety and help with care. These technologies include systems that incorporate wearable or environmental sensors to detect bed occupancy, falls, entry and exit through doorways, and provide location monitoring, activity, or physiological changes. These items alert staff when assistance is needed and provide data for analysis. There is growing interest in video technology, partly to address fears of malpractice, but also to record unwitnessed incidents such as falls or altercations between residents (Hall et al., 2019).
For people with dementia, technologies related to safety can be something as simple as a grab-bar or a safety razor. In a healthcare center—as well as in the home—safety technologies might include rails, barriers, alarms, gait belts, non-skid surfaces, comfortable seating systems, walkers, canes, and wheelchairs. Global positioning devices, phone tracing devices, text messaging, and wearable electronic devices can be useful.
In care homes, video monitoring—combined with bed sensors—can reduce intrusive nighttime check-ups from healthcare workers by avoiding sudden and unnecessary awakenings. These devices have positive quality of life-related outcomes and high levels of acceptance from people with dementia, their caregivers, and staff members (Pappadà et al., 2021).
Smart phones have a wide variety of applications that can be used to improve safety. Alarm reminders can be set for medications, voice activation can be used for phone calls, and the phone can be used as a personal planner. But smart phones are expensive, complicated, easily misplaced, and useless if a person refuses or is unable to use the device.
A person’s experience and preferences affect the usefulness of any electronic device. For example, most older adults grew up with analog clocks (clocks with hands) and may be most comfortable with this style of clock. TV controls are increasingly complicated—especially for a person with visual impairment.
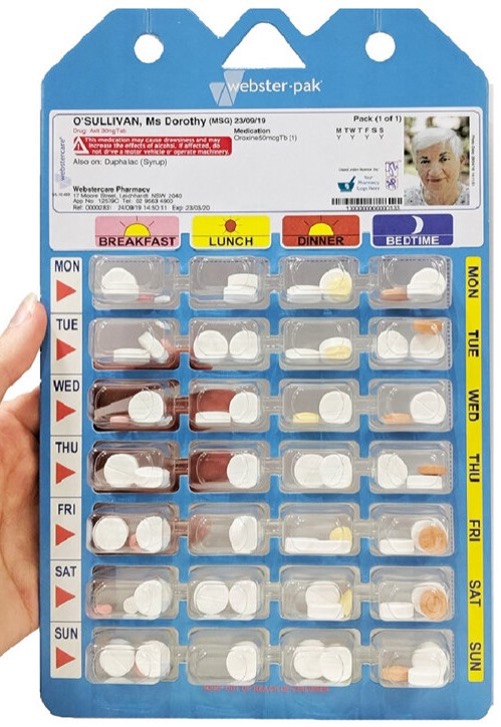
A Webster-Pak®. Used by permission.
For medication management, a pre-packaged medication system and electronic pill reminder may be useful, especially in the early and moderate stages of dementia. Other medication safety devices include (Dementia Australia, 2022):
- boxes with separate flip-top pill compartments labelled with the time and day of the week
- automatic pill dispensers with visual and sound prompts
- Webster-Paks® available from pharmacies
- medication management mobile phone apps
14.3.1 Usability and Acceptance of Safety Technologies
Usability and acceptability are key issues when considering a new technology intended to be used by older adults with dementia. Usability is the level at which a device can assist users without interfering with their normal activities of daily living (Abbate et al., 2014).
In the context of dementia care, acceptability is the degree to which a technology is pleasing and agreeable to the user. Usability and acceptability are related to how easy it is to use the technology and whether a person is willing to use the object. Additionally, usability and acceptance are related to:
- time to accept
- willingness to keep
- number of errors due to incorrect interactions
- level of satisfaction (Abbate et al., 2014)
To be useful, the design of safety devices must consider the users’ needs, fears, mental models, self-learning ability, social behavior, lifestyle, and fashion tastes. Despite this, little effort has been made to assess their usability and acceptability of new technologies before deployment (Abbate et al., 2014).
14.3.2 Monitoring Wandering with a GPS Device
Wandering outside the home can put a person at risk of exploitation and injury and increase caregiver stress and anxiety. Often, however, a person who wanders does not go far from home, may be in familiar territory, can find their way home, and may be at relatively low risk. Locking people inside a home or facility must be balanced against the potential benefits of physical exercise, social contact, informal supervision by neighbors, and the perception of autonomy afforded by “safe walking” (Milne et al., 2014).
The rapid growth of information and communication technologies has created new opportunities for safety interventions. Locator devices using Global Positioning System (GPS) navigation may promote safe walking while simultaneously balancing an individual’s autonomy and safety (Neubauer et al, 2022).
In theory these devices can provide the exact coordinates of a person carrying the GPS device. Safe areas and times can be set up that allow the person to move around through familiar areas but will set off an alert if a geo-temporal limit (or “geo-fence”) is breached. Additional services such as an operator to phone the person and using GPS to guide them home have also been described (Milne et al., 2014).
The adoption rate of these devices is relatively low. Abandonment of the devices is a concern as well as privacy, cost, and device complexity, which can pose barriers to their use among older adults. The legal repercussions of technologies that collect, store, and upload data have not been considered or addressed. Locator devices, for example, place users at risk of their information being publicized, which in turn can put vulnerable users, such as persons with cognitive decline, at greater risk for elder abuse (Neubauer et al, 2022).
14.3.3 Using Technology to Prevent Falls
Technology-based interventions have been deployed in a wide range of falls prevention contexts and include diagnosing and treating fall risks, increasing adherence to interventions, detecting falls, and alerting clinicians in case of falls. Technology also has the potential to play a role in enabling older adults to self-assess, giving them the opportunity to perform self-assessments (Hamm et al., 2016).
Pre-fall prevention interventions are technology applications that focus on supporting patients who have not yet experienced a fall but may be at risk of falling. They take a pro-active approach via the development of applications, which support the delivery of targeted physical activities, exercises, and education programs that increase awareness of fall risks and help develop strategies to identify and overcome environmental fall hazards and the complications that may arise after having a fall (Hamm et al., 2016).
Post-fall prevention interventions are applications of technology which focus on individuals who have already experienced a fall and aim to help assess and deliver interventions to reduce the future risk of repeated falling episodes. Interventions share similarities with the pre-fall program emphasizing applications that support the delivery of exercise and education programs with a view to overcoming intrinsic and extrinsic fall risk factors (Hamm et al., 2016).
Technology that support falls-prevention systems are (Hamm et al., 2016):
- Game consoles: self-contained platforms in which specific game applications are utilized by falls prevention systems to deliver falls prevention related games.
- Nintendo Wii and Microsoft Kinect: for intervention types such as physical activities, game consoles and sensor devices such as are often used.
- Desktop computers.
- Smart phones: with integrated sensors and communication features.
- Tablets: which includes inertia measurement units, sensors (accelerometer, gyroscope, GPS), camera and touchscreen display.
- Virtual reality devices.
