The International Association for the Study of Pain (IASP) describes pain as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage.” Pain can be acute or chronic and if left untreated chronic pain can develop into what is referred to as a chronic pain syndrome.
Acute Pain
Acute pain comes on quickly and, although it can be severe, lasts a relatively short time (IOM, 2011). Its location is usually well-defined and there is usually an identifiable painful stimulus related to an injury, brief disease process, surgical procedure, or dysfunction of muscle or viscera. Acute pain is often successfully treated with patient education, mild pain medications, environmental changes, and stress reduction.
The Institute of Medicine (IOM) has targeted improved treatment of acute pain as an area of significant healthcare savings. Better treatment of acute pain, through education about self-management and better clinical treatment, can avoid its progression to chronic pain, which is more difficult and more expensive to treat (IOM, 2011).
Chronic Pain
Chronic pain refers to pain that exists for three or more months and does not resolve with treatment. The three-month time frame is not absolute and some conditions may become chronic in as little as a month. When pain becomes chronic, sensory pathways continue to transmit the sensation of pain even though the underlying condition or injury that originally caused the pain has healed. In such situations, the pain itself may need to be managed separately from the underlying condition.
Chronic pain is a symptom of many diseases. Up to 70% of cancer patients suffer from chronic pain and, among individuals living with HIV/AIDS, pain has been reported at all stages of infection (Lohman et al., 2010). Chronic pain is a silent epidemic that reduces quality of life, negatively impacts relationships and jobs, and increases rates of depression (Sessle, 2012).
Chronic pain affects 1 in 5 adults, is more prevalent among women and older adults, and is associated with physically demanding work and lower level of education (King & Fraser, 2013). A 2011 report from IOM places this cost at more than $500 billion per year in the United States, creating an economic burden that is higher than the healthcare costs for heart disease, cancer, and diabetes combined (Sessle, 2012).
Chronic pain can be difficult to distinguish from acute pain and can be difficult to treat. Chronic pain does not resolve quickly and opioids or sedatives are often needed for treatment. Because medical practitioners frequently approach chronic pain management from a medication perspective, other modalities are sometimes overlooked.
Prevention, assessment, and treatment of chronic pain are challenges for health providers and systems. Pain might go unrecognized, and patients—particularly members of racial and ethnic minority groups, women, elders, people with cognitive impairment, and those with cancer and at the end of life—can be at risk for inadequate pain treatment. Patients can experience persistent pain that is not well controlled (CDC, 2016a).
There are clinical, psychological, and social consequences associated with chronic pain including activity limitations, lost work productivity, reduced quality of life, and stigma, emphasizing the importance of appropriate and compassionate patient care. Patients should receive appropriate pain treatment based on a careful consideration of the benefits and risks of treatment options (CDC, 2016a).
Musculoskeletal pain, especially joint and back pain, is the most common type of chronic pain (IOM, 2011). Although musculoskeletal pain may not correspond exactly to the area of injury, it is nevertheless commonly classified according to pain location. However, most people with chronic pain have pain at multiple sites (Lillie et al., 2013).
Classifying Chronic Pain According to Pathophysiology
When classified according to pathophysiology, three types of chronic pain have been described by the International Association for the Study of Pain (IASP):
- Nociceptive pain: caused by stimulation or sensitization of peripheral nociceptors. Nociceptors have a high threshold for activation and increase their output as the stimulus increases.
- Neuropathic pain: “pain arising as a direct consequence of a lesion or disease affecting the somatosensory system” (IASP, 2012).
- Central neuropathic pain: originates from damage to the brain or spinal cord.
- Peripheral neuropathic pain: originates from damage to the peripheral nerves or nerve plexuses, dorsal root ganglion, or nerve roots (IASP, 2012).
- Psychogenic pain*: pain that persists despite the lack of any identified underlying physical cause.
*The term psychogenic pain is no longer considered an official diagnostic term. A more correct diagnostic term is persistent somatoform pain disorder (PSPD), which is defined in the ICD-10 Version 2016 as persistent, severe, and distressing pain, which cannot be explained fully by a physiological process or a physical disorder, and which occurs in association with emotional conflict or psychosocial problems that are sufficient to allow the conclusion that they are the main causative influences. The result is usually a marked increase in support and attention, either personal or medical (ICD-10, Version 2016).
Chronic Pain Syndromes
A chronic pain syndrome differs from chronic pain in that over time people with a syndrome develop a number of related life problems beyond the sensation of pain itself. Most individuals with chronic pain do not develop the more complicated and distressful chronic pain syndrome. Although they may experience the pain for the remainder of their lives, little change occurs in their daily activities, family relationships, work, or other life components. Many of these individuals never seek treatment for pain and those who do often require less intensive, single-modality interventions (VHA, 2015).
Those who develop chronic pain syndromes tend to experience increasing physical, emotional, and social deterioration over time. They may abuse pain medications and typically require more intensive, multimodal treatment to stop the cycle of increasing dysfunction (VHA, 2015).
Complex regional pain syndrome (CRPS) describes a chronic neuropathic pain condition that, in the past, was referred to by several other names including causalgia and reflex sympathetic dystrophy. The IASP has endorsed the term complex regional pain syndrome, intended to be descriptive, general, and not imply etiology. The term has been divided into “CRPS 1” and “CRPS 2” (Dutton & Littlejohn, 2015). CRPS I is characterized by intractable pain that is out of proportion to the trauma, while CRPS II is characterized by unrelenting pain that occurs subsequent to a nerve injury.
The pain in CRPS is regional, not in a specific nerve territory or dermatome, and it usually affects the hands or feet, with pain that is disproportionate in severity to any known trauma or underlying injury. It involves a variety of sensory and motor symptoms including swelling and edema, discoloration, joint stiffness, weakness, tremor, dystonia, sensory disturbances, abnormal patterns of sweating, and changes to the skin (O’Connell et al., 2013).
Complex Regional Pain Syndrome (CRPS) in Hand and Wrist
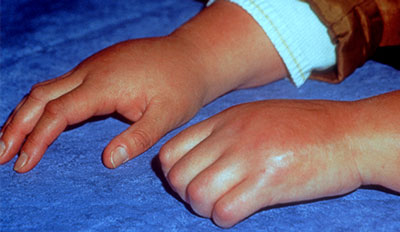
Source: Wikimedia Commons. Used by permission.
It has been common to explain the etiology of complex regional pain syndrome using the psychogenic model. Now however, neurocognitive deficits, neuroanatomic abnormalities, and distortions in cognitive mapping are known to be features of CRPS pathology (Hill et al., 2012).
What Is Chronic Pain? [2:31]
https://www.youtube.com/watch?v=GTmE5X8NcXM
