Complementary, alternative, and integrative health approaches are often used to treat or manage disorders or symptoms associated with acute and chronic pain. Common complementary health approaches include mind and body interventions such as meditation, spinal manipulation, yoga, massage, tai chi, and acupuncture. A variety of natural products, including herbs, dietary supplements, and prebiotic or probiotic products are also commonly used (NCCIM, 2016a).
The most current and comprehensive picture of Americans’ use of complementary health approaches has been developed under the National Center for Complementary and Integrative Health (NCCIH) through two National Health Interview Surveys (NHIS) conducted by the National Center for Health Statistics at the CDC in 2002, 2007, and 2012.
The surveys showed:
- Non-vitamin, non-mineral dietary supplements were the most commonly used complementary health approach at each of the three time points.
- Whether used independently or as a part of other approaches, deep-breathing exercises were the second most commonly used complementary health approach.
- The use of yoga, tai chi, and qi gong increased linearly over the three time points, beginning at 5.8% in 2002, 6.7% in 2007, and 10.1% in 2012. Yoga was the most commonly used of these three approaches at all three time points.
- There was a small but significant linear increase in the use of homeopathic treatment, acupuncture, and naturopathy.
- The use of chiropractic care or chiropractic and osteopathic manipulation was the fourth most commonly used approach.
- Meditation was used by 7.6% of adults in 2002, 9.4% in 2007, and 8.0% in 2012, keeping it among the top five most commonly used approaches for each time point.
- Ayurveda, biofeedback, guided imagery hypnosis, and energy healing therapy had a consistently low prevalence and had no significant changes across the three time points (Clarke et al, 2015).
In the United States, more than 30% of adults and about 12% of children use healthcare approaches developed outside of mainstream Western, or conventional, medicine. When describing these approaches, people often use alternative and complementary interchangeably, but the two terms refer to different concepts:
- If a non-mainstream practice is used together with conventional medicine, it is considered complementary.
- If a non-mainstream practice is used in place of conventional medicine, it is considered alternative. True alternative medicine is uncommon. Most people who use non-mainstream approaches use them along with conventional treatments. (NCCIH, 2016b)
Complementary therapies differ from Western medicine in at least four ways:
- They are often not covered by health insurance providers.
- There is limited, but growing, scientific evidence about their safety and effectiveness.
- They view the patient as a whole (holistically).
- They view the body as more than the sum of its parts.
Integrative Pain Management
Integrative healthcare brings conventional and complementary approaches together in a coordinated way. Researchers are currently exploring the potential benefits of integrative health in a variety of situations, including pain management for military personnel and veterans, relief of symptoms in cancer patients and survivors, and programs to promote healthy behaviors (NCCIH, 2016b).
Complementary and integrative medicine provide patient-centered care, addressing physical, emotional, mental, social, spiritual, and environmental influences that affect a person’s health. They use the most appropriate interventions from an array of disciplines to heal illness and help people regain and maintain optimal health. Because integrative medicine is a “whole systems” approach that employs multiple modalities, as opposed to an isolated complementary therapy, studying outcomes is more challenging than evaluating an isolated pharmaceutic or botanic intervention (Abrams et al., 2013).
Integrative medicine is a popular approach to pain management, although for a large, structured healthcare organization, integrating diverse practices can be challenging. Healthcare organizations must balance supply and demand for services as well as combine the integrative medicine program into the established culture of a large hospital (Nate et al., 2015).
In an effort to capture data on patient-reported outcomes in integrative medicine, a number of leading clinics have collaborated to form the first practice-based research network in the field: the Bravewell Integrative Medicine Research Network (BraveNet). BraveNet’s initial project involved 4182 patients seeking care at nine clinical sites. The data confirmed the high utilization of integrative medicine by chronic pain patients and led to a Study on Integrative Medicine Treatment Approaches for Pain (SIMTAP). In this study, researchers reported the impact of a six-month integrative approach on chronic pain and a number of other related patient-reported outcome measures (Abrams et al., 2013).
In the SIMTAP study, practitioners at each of the sites devised treatment plans for participating chronic pain patients. All BraveNet sites include integrative physicians, acupuncturists, mindfulness instructors, and yoga instructors; some also incorporate massage therapists, manual medicine therapists, fitness and movement specialists, dieticians and nutritionists, psychologists, healing touch therapists, and other energy practitioners. The results of this study suggest that the tailored, multimodal approach to treating chronic pain that combined conventional and complementary therapies improves quality of life and reduces pain, stress, and depressive symptoms (Abrams et al., 2013).
How complementary and integrative therapies affect the nervous system and other physiologic systems such as organs and tissues, remains understudied. Such studies are challenging for both the complementary and integrative health and the research communities. Nevertheless, recent advances in genomics, neuroscience, stem cells, systems biology, neuroimaging, and computational modeling offer excellent resources and opportunities for innovative studies of complementary health approaches (NCCIH, 2016a).
For the treatment of chronic pain among active-duty military personnel and veterans, the National Center on Complementary and Integrative Health (NCCIH), the U.S. Department of Veterans Affairs and other agencies are sponsoring research to see whether integrative approaches can help patients with chronic pain. NCCIH-funded studies are testing the effects of adding mindfulness meditation, self-hypnosis, or other complementary approaches to pain management programs for veterans. The goal is to help patients feel and function better and reduce their need for pain medicines that can have serious side effects (NCCIH, 2016b).
Some cancer treatment centers are using integrative healthcare programs such as acupuncture and meditation to help manage symptoms and side effects for patients who are receiving conventional cancer treatment. Although research on the potential value of these integrative programs is in its early stages, some NCCIH-funded studies have had promising results:
- Cancer patients who receive integrative therapies while in the hospital have less pain and anxiety.
- Massage therapy may lead to short-term improvements in pain and mood in patients with advanced cancer.
- Yoga may relieve the persistent fatigue that some women experience after breast cancer treatment. (NCCIH, 2016b)
- A growing body of evidence supports the efficacy and safety of non-drug and complementary health approaches to reduce pain and increase patients’ coping ability and general well-being. Many of these techniques have the potential to reduce the need for costly pain medications with harmful side effects. At a minimum, providers should have a basic understanding of the scientific evidence on complementary health approaches so that patients will not be reluctant to disclose their use.
- Non-drug interventions for pain management introduced early in the course of an illness are more likely to succeed because they can be learned and practiced by patients while they have sufficient strength and energy. Patients and their families should be given information about and encouraged to try several strategies, and to select one or more mind-body techniques for regular use.
Mind and Body Practices
Mind-body techniques(also called cognitive/behavioral techniques) focus on the interactions among the brain, mind, body, and behavior, with the intent of using the mind to affect physical function and promote health. The concept that the mind is important in the treatment of illness is integral to the healing approaches of traditional Chinese medicine (TCM) and Ayurvedic medicine,* which are both more than two thousand years old (NCCIH, 2016b).
*Ayurvedic medicine is a healing system from India emphasizing balance among body, mind, and spirit.
Mind-body techniques require that patients understand the information and instructions involved; therefore, these techniques are not appropriate for patients with significant cognitive impairment. Cognitive therapies require cooperation and practice and are thus contraindicated for use with patients who are uncooperative, unable, or unwilling to practice the necessary behaviors.
Mind and body practices include a large and diverse group of procedures and techniques administered or taught by a trained practitioner or teacher. The 2012 National Health Interview Survey showed that yoga, chiropractic and osteopathic manipulation, meditation, and massage therapy are among the most popular mind and body practices used by adults. The popularity of yoga has grown dramatically in recent years, with almost twice as many U.S. adults practicing yoga in 2012 as in 2002 (NCCIH, 2016b).
Other mind and body practices include acupuncture, relaxation techniques (eg, breathing exercises, guided imagery, progressive muscle relaxation), tai chi, qi gong, healing touch, hypnotherapy, and movement therapies (eg, Feldenkrais method, Alexander technique, Pilates, Rolfing Structural Integration, Trager psychophysical integration) (NCCIH, 2016b).
The amount of research on mind and body approaches varies widely depending on the practice. For example, researchers have done many studies on acupuncture, yoga, spinal manipulation, and meditation, but there have been fewer studies on some other practices (NCCIH, 2016b).
The amount of research on mind and body approaches varies widely depending on the practice. For example, researchers have done many studies on acupuncture, yoga, spinal manipulation, and meditation, but there have been fewer studies on other practices (NCCIH, 2016b).
Chiropractic Medicine
Chiropractic Treatment

A chiropractor demonstrating an adjustment on the patient’s thoracic spine. Source: Michael Dorausch, Wikimedia Commons.
Chiropractic is a healthcare profession that focuses on the relationship between the body’s structure—mainly the spine—and its functioning. Although practitioners may use a variety of treatment approaches, they primarily perform adjustments (manipulations) to the spine or other parts of the body with the goal of correcting alignment problems, alleviating pain, improving function, and supporting the body’s natural ability to heal itself (NCCIH, 2012).
In the United States, chiropractic is often considered a complementary health approach. According to the 2007 National Health Interview Survey (NHIS), which included a comprehensive survey of the use of complementary health approaches by Americans, about 8% of adults and nearly 3% of children had received chiropractic or osteopathic manipulation in the past 12 months (NCCIH, 2012).
Massage Therapy
Massage is a centuries-old healing art, practiced in ancient China, Japan, India, the Arabic nations, Egypt, Greece, and Rome. Massage is sometimes considered a relaxation therapy because that is one of its major effects.
Massage therapy, one of the complementary and alternative treatments, is defined as a therapeutic manipulation using the hands or a mechanical device that includes numerous specific and general techniques often used in sequence, such as effleurage (stroking), petrissage (kneading), and percussion. It may be the earliest and most primitive tool used to improve pain. The most ancient references to the use of massage come from China (circa 2700 B.C.). Common types of massage therapy include Swedish massage, Shiatsu, Rolfing, reflexology, myofascial release, and craniosacral therapy (Kong et al., 2013).
In general, massage therapists press, rub, and otherwise manipulate the muscles and soft tissues of the body. They use massage not only to relieve pain but also to rehabilitate sports injuries; reduce stress, anxiety, and depression; increase relaxation; and aid general well-being.
Massage is effective in general pain management because it mechanically assists in venous and lymphatic flow, improves skin integrity and mobility, desensitizes tissue, and provides comfort and psychological support. Massage may be used to stretch muscles and is generally used in combination with other treatments.
Massage can also be helpful for older adults. Nurse researchers who reviewed 21 studies on massage in elders found that slow-stroke back massage and hand massage significantly increased relaxation across all care settings (Harris & Richards, 2010).
Massage has proved effective in reducing pain, anxiety, and tension after cardiovascular surgery. In a study at Mayo Clinic, patients were randomized either to receive a massage or to have quiet relaxation time following surgery. Those who received massage therapy had significantly less pain, anxiety, and tension than the control group (Braun et al., 2012).
Burn victims suffer some of the most severe physical and psychological pain imaginable. Turkish researchers found that massage therapy reduced pain, itching, and anxiety levels in adolescents in the burn unit of a large university hospital. Massage therapy reduced all three symptoms from the first day of the study until the last (Parlak et al., 2010).
Researchers in Spain studied the effects of massage combined with myofascial release therapy* on patients diagnosed with fibromyalgia. Patients were randomized to receive either the massage-myofascial release therapy or a sham treatment during 20 weekly sessions. Immediately after treatment and 1 month later, the researchers found that anxiety levels, quality of sleep, pain, and quality of life were improved in the experimental group (Castro-Sánchez et al., 2011).
*Myofascial release therapy is a type of physiotherapy requiring special training that aims to release myofascial restrictions at the sites of certain painful points called trigger points.
A 2010 AHRQ evidence report—which summarized, critically appraised, and compared the evidence on clinical benefits, costs, and harms associated with use of complementary and integrative medicine and other therapies for the treatment of adults with low back, neck, and thoracic pain—found that massage was superior to placebo or no treatment in reducing pain and disability immediately post treatment only in subjects with acute/subacute but not in subjects with chronic low back pain (AHRQ, 2014).
Massage was:
- Significantly better than relaxation or physical therapy in reducing chronic nonspecific low back pain intensity but not range of motion, immediately after the treatment
- Better than no treatment in reducing immediate-term post treatment pain intensity in subjects with chronic or unknown duration of nonspecific pain
- Better than placebo in reducing neck pain intensity immediately after the treatment in subjects with acute/subacute or unknown duration of nonspecific pain
- Not different from placebo in improving well-being or range of motion in subjects with chronic pain (AHRQ, 2014)
Meditation
Monastic Practitioner of Meditation


Phra Ajan Jerapunyo, Abbot of Watkungtaphao meditating in Sirikit Dam, Thailand. Source: Wikimedia Commons.
Meditation refers to a group of techniques rooted in ancient religious and spiritual traditions. It is used to increase calm, promote relaxation, improve psychological balance, cope with illness, or enhance overall health and well-being. People also use meditation for various health problems, including anxiety, pain, depression, stress, insomnia, and physical or emotional symptoms associated with chronic illness and their treatment.
Mindfulness meditation is one of the most studied and practiced forms of meditation in America. Pioneered at the University of Massachusetts Medical School’s Stress Reduction Clinic in 1979 by Jon Kabat-Zinn, mindfulness-based stress reduction (MBSR) meditation has been shown to be effective in reducing depression and anxiety, both known to influence pain.
Previous research has shown that mindfulness meditation helps relieve pain, but researchers have been unclear about how the practice induces pain relief—specifically, if meditation is associated with the release of naturally occurring opiates. Results from a new study, funded in part by the NCCIH, demonstrate that mindfulness meditation does not rely on the endogenous opioid activity to reduce pain, which is an important consideration for using meditation to treat chronic pain.
In this study, conducted by researchers at Wake Forest School of Medicine and Cincinnati Children’s Hospital Medical Center, researchers recorded pain reports in 78 healthy adults during meditation or a non-meditation control in response to painful heat stimuli and intravenous administration of the opioid antagonist naloxone (a drug that blocks the transmission of opioid activity) or placebo saline. Participants were randomized to one of four treatment groups: (1) meditation plus naloxone; (2) control plus naloxone; (3) meditation plus saline; or (4) control plus saline. People in the control groups were instructed to “close your eyes and relax until the end of the experiment” (NCCIH, 2016c).
Researchers found that participants who meditated during saline administration had significantly lower pain intensity and unpleasantness ratings compared to those who did not meditate while receiving saline. Importantly, data from the meditation plus naloxone group showed that naloxone did not block meditation’s pain-relieving effects. No significant differences in reductions of pain intensity or pain unpleasantness were seen between the meditation plus naloxone and the meditation plus saline groups. Participants who meditated during naloxone administration also had significantly greater reductions in pain intensity and unpleasantness than the control groups (NCCIH, 2016c).
These findings demonstrate that mindfulness meditation reduces pain independent of opioid neurotransmitter mechanisms. The researchers noted that because opioid and non-opioid mechanisms of pain relief interact synergistically, the results of this study suggest that combining mindfulness-based and pharmacologic/non-pharmacologic pain-relieving approaches that rely on opioid signaling may be particularly effective in treating pain (NCCIH, 2016c).
Hypnotherapy
In hypnotherapy a patient attempts to enter into a trance-like state in order to cope better with complaints such as pain, anxiety, and stress by actively diverting their attention towards relaxing thoughts.
Katja Boehm, Markus Horneber
and the CAM-Cancer Consortium
Hypnotherapy involves the power of suggestion by a hypnotherapist or by the patients themselves. Hypnotic techniques have proven to be useful for different kind of pain—especially pain associated with burns, cancer, invasive medical procedures, headaches, musculoskeletal conditions, irritable bowel syndrome, and fibromyalgia (Ardigo et al., 2016). Hypnotherapy may help reduce pain, decrease anxiety, and improve immune function. It overlaps with guided imagery and visualization, creating an altered state of awareness. Hypnosis enhances the ability to focus attention to the exclusion of other stimuli. It may take seconds to minutes to achieve entrance to a hypnotic state.
The practice of self-hypnosis has been shown in studies to be an important element in the long-term control of chronic pain. Self-hypnosis can be taught to the patient as a tool to modify behavior regarding nociceptive perception. It allows patients to take an active part in their own pain management using personal resources and experiences (Ardigo et al., 2016).
Hypnosis is thought to be beneficial for:
- Decreasing perioperative pain
- Reducing analgesic and sedative requirements
- Decreasing post operative anxiety
- Improving patient satisfaction and mood (Ardigo et al., 2016)
Hypnosis usually requires a trained professional, but even then it may not work for all patients, perhaps because of the social stigma associated with its use. However, the efficacy of hypnosis in relieving pain has been shown in cancer patients (Boehm & Horneber, 2016), burned children (Bayat et al., 2010), in adults with chronic and acute pain, and in older hospitalized adults (Ardigo et al., 2016).
Biofeedback
Biofeedback-assisted relaxation uses an external device to help the patient learn to relax specific muscle groups. Applying biofeedback requires special equipment and clinical training. Relaxation techniques may prove beneficial by reducing muscular arousal and distracting the patient from painful sensations. These techniques also reduce anxiety and increase the patient’s sense of control.
Biofeedback is a popular intervention alone or within cognitive-behavioral or multidisciplinary pain treatments. Biofeedback is a procedure in which patients’ bodily responses, such as muscle tension, heart rate, or skin temperature, are monitored and reported to the patient through an auditory or visual modality. In electromyographic feedback (EMG-FB), one of the most common types of feedback, patients learn to control and to alleviate their muscle tension (Glombiewski et al., 2013).
Biofeedback is often called a “psychophysiologic intervention,” although its mechanisms are more psychological than physiologic. The effectiveness of EMG biofeedback is mediated by cognitive changes, such as increases in self-efficacy and coping strategies induced through biofeedback training, rather than primarily by learned physiologic control (Glombiewski et al., 2013).
Electroencephalographic feedback (EEG-FB) is often referred to as “neurofeedback” or “EEG biofeedback.” EEG-FB records and reports back EEG waves. Patients are able to learn to influence evoked potentials and event-related potentials, and slow cortical potentials and EEG frequencies (Glombiewski et al., 2013).
Biofeedback has been found to be beneficial in the rehabilitation of headache and, in some studies, of chronic back pain and several other pain disorders (eg, temporomandibular or TMJ disorders). Findings on low back pain, however, show little to no improvement. A meta-analysis of the efficacy of biofeedback in fibromyalgia found that EMG-BFB was effective for the short-term reduction of pain intensity in fibromyalgia patients (Glombiewski et al., 2013).
Music Therapy
Music therapy dates back to Aristotle and Plato. In 1944 in the United States, Michigan State University offered the first music-therapy degree program worldwide (Schmid & Ostermann, 2010). Sedating or soothing music is instrumental, rhythmic, and 60 to 80 beats per minute. In much of the research, musical pieces are selected from five types of music: synthesizer, harp, piano, orchestra, or slow jazz.
Two types of music interventions are distinguished: live music therapy and recorded music. In live music therapy a trained music therapist plays music and applies various therapeutic techniques to reach a therapeutic goal. One of these techniques is known as music entrainment, in which the music therapist first uses music to match the patient’s physiologic and emotional states and then gradually changes the music to modify the patient’s state. Recorded music, on the other hand, implies listening to prerecorded music selected by a music therapist or by patients themselves, provided they are old enough to do so (van der Heijden et al., 2015).
Research indicates that music therapy can be effective in reducing both chronic and acute pain in children and adults. A review of randomized clinical trials found that music therapy significantly reduced pain, anxiety, and distress in children undergoing orthopedic, cardiac, and day surgery procedures (van der Heijden et al., 2015). Music also reduced pain, anxiety, and muscle tension in children during burn dressing changes (Tan et al., 2010).
Effective music therapy requires a professional music therapist who can tailor the intervention to the individual patient. Music may accompany other mind-body techniques such as guided imagery, gentle massage, or bodywork. Home-based music programs are gaining importance for severely impaired or older adults who are unable to attend daycare centers where music is provided (Schmid & Ostermann, 2010).
Traditional Chinese Medicine
Traditional Chinese medicine (TCM) is a holistic medical system for diagnosis, prevention, and treatment of diseases. It has been an integral part of Asian cultures for thousands of years. TCM uses therapies such as acupuncture, massage, and herbal medicine and is characterized by its underpinning theoretical guide—the philosophy of yin-yang balance (Xu et al., 2013).
Traditional Chinese medicine views the body as a system of channels through which energy flows. The Chinese call this energy qi or chi. Disease or illness is caused when the energy gets blocked or stagnates and doesn’t flow freely through the body. Herbs, acupuncture, qi gong, tai chi, and Chinese massage are mind-body techniques to help unblock the flow of chi through normal channels and thereby restore health. Practitioners of traditional Chinese medicine devise individualized treatment plans based on each patient’s unique diagnosis rather than following a standard intervention based on the complaint (Abrams et al., 2013).
In a seminal randomized controlled trial of Chinese herbal medicine for treatment of irritable bowel syndrome, investigators compared a standard and an individualized Chinese herbal formulation to a placebo. Results showed that, compared with patients in the placebo group, patients in the two active treatment groups had improvements in bowel symptoms as rated by both the patients and their gastroenterologists at the end of the 16-week intervention. However, at follow-up 14 weeks after completion of the treatment, only the individualized herbal medicine treatment group maintained improvement (Abrams et al., 2013).
In China traditional medicine is one of the conservative treatments for lumbar disc herniation, and several studies have confirmed that it has certain effects on low back pain caused by lumbar disc herniation. Treatments include acupuncture, oral administration of Chinese medicine, external application of Chinese medicine, Chinese tuina (massage), and TCM-characteristic functional exercise. Clinically, these therapeutic methods are not used alone but in combination (Yuan et al., 2013).
In the treatment of pain due to lumbar disc herniation, different traditional Chinese medicine therapies have different advantages. Pain is the main symptom in the acute stage and acupuncture has good analgesic effect. Lumbar dysfunction is the main symptom in the remission stage and Chinese massage has good effect on improving dysfunction. Oral Chinese herbal formulae, external use of Chinese medicine, and Chinese herbal injection also showed good effect in relieving pain and improving dysfunction caused by lumbar disc herniation (Yuan et al., 2013).
Acupuncture
The term acupuncture describes a family of procedures involving the stimulation of anatomic points on the body using a variety of techniques. The acupuncture technique most often studied scientifically involves penetrating the skin with hair-thin metallic needles that are inserted a few millimeters into the skin.
According to The Yellow Emperor’s Inner Canon, compiled between 206 B.C.E. and 220 C.E., there are meridians and collaterals in the human body comprising a network of channels through which chi and blood flow. Diseases, or pain, are caused by chi stagnation or blood stasis in the channels. Acupuncture treats this by inserting a fine needle into the skin at designated points (acupuncture points) (Zhang et al., 2013). An appropriate choice of the 361 classic acupuncture points is believed to restore balance in the body. Modern acupuncturists use not only traditional meridian acupuncture points, but also non-meridian or extra-meridian acupuncture points (AHRQ, 2010). Acupuncture promotes the circulation of chi and blood and harmonizes healthy and pathogenic chi in the channels (Zhang et al., 2013).
Acupuncture is not a single standardized intervention. In routine clinical practice, the same patient may receive acupuncture with different characteristics from different practitioners. These differences include specific characteristics of treatment—such as the number and frequency of sessions or the additional use of electrical stimulation—as well as the overall “style” of acupuncture. A distinction is often made between traditional Chinese acupuncture—in which diagnosis and treatment are based on a theoretical framework involving patterns of symptoms and concepts such as yin, yang, and the strength of chi—and westernized approaches, involving a neuro-anatomical basis for diagnosis and treatment (MacPherson et al., 2013).
Application of Acupuncture Needle
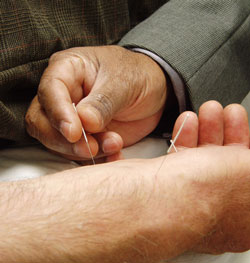
Basic acupuncture. Photo by Kyle Hunter, public domain.
Researchers from the Acupuncture Trialists’ Collaboration, a group that was established to synthesize data from high-quality randomized trials on acupuncture for chronic pain, conducted an analysis of individual patient data from 29 high-quality randomized controlled trials, including a total of 17,922 people. These trials investigated the use of acupuncture for back and neck pain, osteoarthritis, shoulder pain, or chronic headache (Vickers, 2012).
For all pain types studied, the researchers found modest but statistically significant differences between acupuncture and simulated acupuncture approaches, and larger differences between acupuncture and no-acupuncture controls. (In traditional acupuncture, needles are inserted at specific points on the body. Simulated acupuncture includes a variety of approaches that mimic this procedure; some approaches do not pierce the skin or use specific points on the body.) The sizes of the effects were generally similar across all pain conditions studied (Vickers, 2012).
These findings suggest that the total effects of acupuncture, as experienced by patients in clinical practice, are clinically relevant. They also noted that their study provides the most robust evidence to date that acupuncture is more than just placebo and a reasonable referral option for patients with chronic pain (Vickers, 2012).
How acupuncture works to relieve pain and other symptoms is still incompletely understood, although functional MRI (fMRI) studies are beginning to provide some answers. Acupuncture seems to change the way the brain perceives and processes pain. Using fMRI in 18 volunteers, German researchers viewed pain centers in the brain while applying an electrical pain stimulus to subjects’ ankles before and after acupuncture treatment. They reported that “activation of brain areas involved in pain perception was significantly reduced or modulated under acupuncture” (Theysohn et al., 2010).
Chinese Tuina (Massage)
Tuina is a form of bodywork or massage therapy that is generally used in conjunction with other types of traditional Chinese medicine. Among non-drug therapies, Chinese tuina is widely used in China for pain management. Tuina is thought to relieve pain by harmonizing the yin and yang of the organs. Tuina is considered gentle on the body and, as such, patients often prefer tuina over pharmaceutical drugs (Zhang et al., 2015).
Tuina involves a wide range of technical manipulations conducted by a practitioner’s finger, hand, elbow, knee, or foot applied to muscle or soft tissue at specific body locations. It incorporates many of the principles of acupuncture, including the use of acupoints. For instance, tuina often uses manual techniques such as pushing, rubbing, kneading, or high-intensity, high-frequency patting to clear energy blocks along specific meridians associated with particular conditions (Yang et al., 2014).
According to traditional Chinese medicine, a state of health reflects an underlying state of balance in the chi and blood of the human body. Pain is usually caused by obstruction of chi and consequently of blood circulation in the affected body region. Pathogenic factors such as blood stasis, chi stagnation, phlegm, dampness, and others can be identified as causative factors in the blockage. The central therapeutic goal of tuina is to remove energetic blocks which lead to chi stagnation. This leads to increased circulation and reduction of localized edema, which helps to reduce associated pain (Yang et al., 2014).
The A-Shi point in acupuncture theory is the tender, local dermal or muscular area or site on the body surface which reproduces the specific pain being treated when it is gently pressed. Its location indicates the precise place where chi and blood are blocked. Manipulation at the A-Shi point is done with the intention of removing the energetic block there to promote the free movement of chi and improve blood circulation in the region. Studies have demonstrated that one mechanism by which this type of massage therapy appears to be clinically beneficial is by reducing inflammation and promoting mitochondrial biogenesis for repair of damaged skeletal muscle (Yang et al., 2014).
Cupping
Cupping therapy (CT) is a traditional Chinese medical treatment which has been practiced for thousands of years. The World Health Organization’s defines cupping as a therapeutic method involving the application of suction by creating a vacuum. This is typically done using fire in a cup or jar on the dermis of the affected part of the body (Chi et al., 2016). Many Americans became aware of cupping when they noticed the characteristic marks on the bodies of the Olympic swim team.
Cupping Procedure Showing Resultant Markings
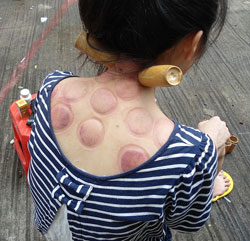
A woman receiving fire cupping in Haikou, Hainan, China. Anna Frodesiak, Public domain.
Cupping, as done by acupuncturists or other therapists, utilizes a glass or bamboo cup to create suction on the skin over a painful area or acupuncture point. It is mostly used in Asian and Middle Eastern countries and has been claimed to reduce pain as well as a host of other symptoms. There are two types of cupping. Dry cupping pulls the skin into the cup without drawing blood. In wet cupping the skin is lacerated so that blood is drawn into the cup (Kim et al., 2011).
Dry cupping creates a vacuum on the skin, with the ensuing negative pressure resulting in capillary rupture. The skin of the localized area becomes flushed and may show petechiae and ecchymosis or bruising, in which the duration is therapeutically beneficial. Cupping has multiple therapeutic functions which include (1) warming the channels to remove cold, (2) promoting chi and blood circulation, (3) relieving swelling, (4) accelerating healing, (5) adjusting body temperature, (6) treating fibromyalgia, (7) for stroke rehabilitation, hypertension, musculoskeletal pain, herpes zoster, (8) treatment of facial paralysis, acne, and cervical spondylosis, and (9) alleviating pain, including chronic neck, shoulder pain, and low back pain (Chi et al., 2016).
Movement-Based Therapies
Movement therapies can include, among others, tai chi, qi dong, yoga, Feldenkrais Method, and Pilates.
Qi Gong and Tai Chi
Tai chi and qi gong are centuries-old, related mind and body practices. They involve certain postures and gentle movements with mental focus, breathing, and relaxation. The movements can be adapted or practiced while walking, standing, or sitting. In contrast to qi gong, tai chi movements, if practiced quickly, can be a form of combat or self-defense (NCCIH, 2015).
Qi gong means, roughly, to cultivate or enhance the inherent functional (energetic) essence of the human being (Jahnke et al., 2010). Qi gong practice includes movement, body posture, mind exercises, concentration, relaxation, and breathing exercises. It is less demanding, both physically and cognitively, than tai chi. Researchers reported that 8 weeks of qi gong training significantly reduced pain for people with osteoarthritis of the knee compared with the control group (Selfe & Innes, 2009).
Tai chi involves slow movements emphasizing balanced postures, regular breathing, and concentration, integrating mind and body. The gentle, slow movements make it particularly useful for those with limited physical strength. Tai chi is used to help manage stress and anger; to improve strength, flexibility, and coordination; to improve lung function; to improve balance; and to reduce pain. Like qi gong, tai chi has been shown to relieve pain and improve function in people with osteoarthritis of the knee (Selfe & Innes, 2009).
For patients with painful knee osteoarthritis, tai chi was as helpful as physical therapy in reducing pain and improving physical functioning, according to a new study partly funded by the NCCIH. In this study, 204 patients age 40 or older who had knee pain and proven osteoarthritis of the knee were randomly assigned to standardized group tai chi training (two 1-hour sessions each week for 12 weeks) or standard one-on-one physical therapy (two 30-minute sessions per week for 6 weeks followed by 6 additional weeks of home-based exercises monitored by the research staff). Both groups were then encouraged to continue their tai chi practice or home exercises for a total of 52 weeks. Patients in the two groups had similar decreases in pain and improvements in physical functioning after 12 weeks, and the benefits of treatment were maintained for the full 52 weeks of the study. Patients in the tai chi group had more improvement in depression symptoms and quality of life than those in the physical therapy group (NCCIH, 2016d).
Yoga
Yoga is a mind and body practice with origins in ancient Indian philosophy. The various styles of yoga typically combine physical postures, breathing techniques, and meditation or relaxation. There are numerous schools of yoga. Hatha yoga, the most commonly practiced in the United States and Europe, emphasizes postures (asanas) and breathing exercises (pranayama). Some of the major styles of hatha yoga are Iyengar, Ashtanga, Vini, Kundalini, and Bikram (NCCIH, 2016e).
Yoga typically combines a series of stretching exercises, breathing techniques, and progressive deep relaxation.
A study involving ninety-five people aged 18 to 64 from six health centers in a low-income, predominantly minority area of Boston found that once- or twice-weekly yoga classes relieved pain, improved function, and reduced the need for pain medication in minority and low-income populations with chronic low back pain. The participants had moderate to severe chronic low back pain and significant related impairment. Most were non-white, unemployed or disabled, with annual household incomes of $40,000 or less. The program also included home practice, keeping a log, meditation, and information on yoga philosophy. Participants were allowed to continue with their usual back care (Saper et al., 2013).
Researchers found statistically significant and clinically meaningful improvements in pain and back-related function in both the once per week and twice per week groups. The most benefit was experienced within the first 6 weeks, which may be of interest to clinicians who wonder how much yoga to recommend to patients. Adverse events, mostly musculoskeletal pain, were common; they generally resolved on their own and were not serious (Saper et al., 2013).
In another study, regular and long-term practice of yoga was shown to improve pain tolerance. Findings from the study also showed that yoga practitioners have more gray matter in multiple brain regions compared with individually matched people who did not practice yoga. The study involved 14 experienced yoga practitioners as well as 14 people who did not practice any mind-body techniques. Participants underwent a cold pain tolerance test by immersing a hand in cold water until they could no longer tolerate the pain. Researchers then asked participants about strategies they used to tolerate the pain. The researchers also conducted brain imaging scans to examine the structural differences in gray matter and white matter between the yoga practitioner group and the control group (Villemure et al., 2013).
Researchers found that yoga practitioners tolerated cold pain more than twice as long as the controls. They found no significant difference in total gray matter volume between groups, but yoga practitioners had greater gray matter volume in brain regions related to pain processing, pain regulation, and attention. Across participants, only the increased gray matter in the mid-insular cortex (a portion of the brain believed to play a role in autonomic integration) correlated with the higher pain tolerance (Villemure et al., 2013).
The volume of insular gray matter in yoga practitioners also positively correlated with the duration of yoga practice, suggesting that yoga experience contributed to these structural differences in the brain. In addition, yoga practitioners had increased white matter integrity within the left insula. Finally, the researchers observed that, to tolerate pain, yoga practitioners used cognitive strategies that are integral parts of yoga practice, such as observing the sensation without reacting, accepting the sensation, using the breath, and relaxation while most control participants did not (Villemure et al., 2013).
Other studies suggest that a carefully adapted set of yoga poses may reduce low-back pain and improve function. One NCCIH-funded study of 90 people with chronic low-back pain found that participants who practiced Iyengar yoga had significantly less disability, pain, and depression after 6 months (NCCIH, 2016e).
In a 2011 study, also funded by NCCIH, researchers compared yoga with conventional stretching exercises or a self-care book in 228 adults with chronic low-back pain. The results showed that both yoga and stretching were more effective than a self-care book for improving function and reducing symptoms due to chronic low-back pain (NCCIH, 2016e).
Conclusions from another 2011 study of 313 adults with chronic or recurring low-back pain suggested that 12 weekly yoga classes resulted in better function than usual medical care (NCCIH, 2016e).
Feldenkrais Method
The Feldenkrais Method (FM) is a type of exercise therapy that was developed over a period of decades in the last century by physician Moshe Feldenkrais. The basis of the approach was founded in the human potential for learning how to learn. Feldenkrais developed an experiential process, or set of processes, whereby an individual or a group could be guided through a series of movement- and sensation-based explorations (Hillier & Worley, 2015).
The purpose of the explorations is to learn to sense the difference between two or more movement options and discern which feels easier and is performed with less effort. This is compared with experiencing less favorable feedback such as pain, strain, or discomfort. Participants are encouraged to try many alternative movements to increase their awareness of distinctions and improvements. Thus the process of intention, action, gaining feedback, making decisions, and re-enacting with adaptations constitutes the learning framework in a somatic context (Hillier & Worley, 2015).
Because it promotes gentle movement within a comfortable range of motion, the Feldenkrais Method is particularly effective for older adults experiencing pain and stiffness from arthritis. It is taught in two parallel forms, Awareness Through Movement (conducted as a group exercise) and Functional Integration (one-on-one approach) (Webb et al., 2013).
Awareness Through Movement lessons are verbally guided explorations of movement that are about 30–60 minutes long. Each lesson explores movement related to a particular function such as walking, rolling, or sitting to enhance awareness of how movements are performed and invite the participant to investigate how they might expand their action and ability to function. The lessons address habitual patterns of movement and expand a person’s self-image. By exploring novel movement sequences, attention is drawn to parts of the self which the person may not be aware of and may have excluded from their functioning. The method aims for a heightened self-awareness, an expansion of a person’s repertoire of movement, and improved functioning where the whole body cooperates in movement and where maximum efficiency is achieved with minimum effort. Dr. Feldenkrais described the aim of the method as “a person who is organized to move with minimum effort and maximum efficiency, not through muscular effort, but through increased consciousness of how movement works” (Webb et al., 2013).
Feldenkrais for Everyday Life [3:33]
https://www.youtube.com/watch?v=uCM_C0Ly0Dc&index=4&list=PLx83c-HVFBfA5quYOUCc3F0z4ox3K054-
Single, randomized controlled studies of Feldenkrais exercises have reported statistically significant, positive benefits compared to control interventions and include the following improvements:
- Improved neck flexion and less perceived effort after a single Feldenkrais lesson for neck comfort
- Reduced prevalence of neck pain and disability in symptomatic women after Feldenkrais (individual and group sessions compared to conventional care or home exercises) and
- Reduced perceived effort in Feldenkrais group for people with upper torso/limb discomfort (Hillier and Worley, 2015)
The Moving with Ease program is a selection of Awareness Through Movement lessons from the Feldenkrais Method. Because the lessons are gentle and enjoyable, they may enable people with osteoarthritis to move more easily and better manage their pain. The self-exploratory nature of the classes provides an opportunity for participants to become aware of how they move, thus learning to minimize their functional limitations. The lessons become a form of self-management that addresses a significant aspect of the process of disablement in people with osteoarthritis (Webb et al., 2013).
In a small Australian study seeking to understand if participation in a Moving with Ease program improved mobility and decreased pain in participants with osteoarthritis, feedback was positive. When asked to describe what they had learned by participating in the program, comments included:
- “How exercise/movement is crucial to managing pain.”
- “To exercise where it is comfortable, not to force it.”
- “To walk with a more fluid, gentle motion.”
- “I learnt to incorporate some of the exercises into my daily life.”
- Participants were asked to comment on their experience of pain and, in particular, the pain associated with their osteoarthritis, after participating in the program. Ten of the fifteen participants said their pain level had improved, three were unsure and two said they had not noticed any difference. Comments included “The pain is continual, but I manage it better,” “At the end of the session I was free from pain and felt energized,” “I can experience less pain in the knees, which is where the osteoarthritis appears for my body,” “The lessons…eased the pain in my lower back,” “No pain in the knees when going up stairs,” and “It is not a cure, however it is the best ‘exercise’ I have experienced for managing my osteoarthritis” (Webb et al., 2013).
Pilates Exercise
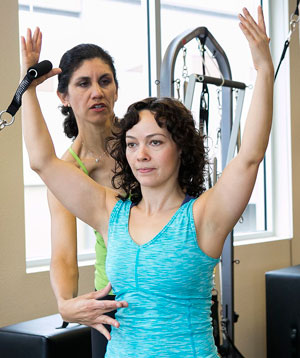
Pilates teacher using verbal and tactile feedback to ensure proper form. Courtesy of Anne Kohler. Source: Wikimedia Commons.
Pilates exercise is named after its founder, Joseph Pilates, who developed a series of exercises in the 1920s to encourage physical and mental conditioning. Core stability, strength, and flexibility are emphasized in Pilates exercise, as is control of movement, posture, and breathing. All of these aspects of Pilates exercise may benefit people with chronic low back pain, as exercises with similar features have been successful in reducing pain and improving functional ability (Wells et al., 2014).
