Despite low-quality evidence supporting practice change, use of chronic opioid therapy for chronic non-cancer pain increased dramatically over the past two decades. Concurrently, opioid analgesic overdose deaths, addiction, misuse, and diversion have increased markedly.
Physicians for Responsible Opioid Prescribing, 2012
Opioids are chemicals that produce morphine-like effects in the body; they are commonly prescribed for the treatment of both acute and chronic pain and for pain associated with cancer. Opioids have a narcotic effect, that is, they induce sedation and are effective for the management of many types of pain.
An estimated 20% of patients presenting to physician offices with noncancer pain symptoms or pain-related diagnoses (including acute and chronic pain) receive an opioid prescription. In 2012 healthcare providers wrote 259 million prescriptions for opioid pain medication, enough for every adult in the United States to have a bottle of pills (CDC, 2016a).
Dozens of compounds fall within this class of opioid analgesics, including hydrocodone, oxycodone, morphine, fentanyl, codeine, propoxyphene (recalled in 2010), hydromorphone (Dilaudid), and meperidine (Demerol). In addition to their effective pain-relieving properties, some of these medications are used to relieve severe diarrhea (eg, Lomotil, or diphenoxylate) or severe coughs (codeine).
Opioids act by attaching opioid receptors, which are found throughout the nervous system as well as in vascular, gut, lung airway, cardiac, and some immune system cells. There are three types of opioid receptors: mu, delta, and kappa.
Mu opioid receptors are thought to give most of their analgesic effects in the CNS, as well as many side effects including sedation, respiratory depression, euphoria, and dependence. Most analgesic opioids are agonists on mu opioid receptors. Of all the analgesics used in pain control, the most safety issues arise with the use of mu opioids, or morphine-like drugs such as morphine, etorphine, methadone, hydromorphone (Dilaudid), sufentanil, and fentanyl.
The delta opioid receptors are more prevalent for analgesia in the peripheral nervous system. The kappa opioid receptors contribute to analgesia in the spine and may cause dysphoria and sedation, but do not generally lead to dependence.
In 2016 the CDC issued Guideline for Prescribing Opioids for Chronic Pain. The guideline calls for a drastic reduction in the use of opioids for the treatment of chronic, noncancer pain. Dosage recommendations for exercising caution are lower than older opioid prescribing guidelines and recognize that even relatively low doses (20–50 morphine milligram equivalents per day) increase risk (CDC, 2016b).
In addition, the CDC Guideline cautions that opioids pose risk to all patients, and currently tools cannot rule out risk for abuse or other serious harm. The Guideline encourages use of recent technological advances, such as state prescription drug monitoring programs, and provides more specific recommendations than previous guidelines on monitoring and discontinuing opioids when risks and harms outweigh benefits (CDC, 2016b).
Benefits and Harms of Opioid Therapy
Balance between benefits and harm is a critical factor influencing the strength of clinical recommendations. The CDC has considered what is known about benefits and harms related to specific opioids and formulations, high-dose therapy, co-prescription with other controlled substances, duration of use, special populations, and risk stratification and mitigation approaches (CDC, 2016a):
- Serious risks have been associated with the use of extended release/long-acting (ER/LA) opioid formulations.
- Serious risks have been associated with time-scheduled opioid use, specifically substantially higher average daily opioid dosage than as-needed opioid use.
- Overdose risk is dose-dependent, with higher opioid dosages associated with increased overdose risk.
- Concurrent use of benzodiazepines and opioids might put patients at greater risk for potentially fatal overdose.
- Patients with sleep apnea, sleep-disordered breathing, renal or hepatic insufficiency, older adults, pregnant women, patients with depression or other mental health conditions, and patients with alcohol or other substance use disorders have been found to have an increased risk for harm from opioids.
- Reduced renal or hepatic function can lead to a greater peak effect and longer duration of action and reduce the dose at which respiratory depression and overdose occurs.
- Age-related changes in patients aged ≥65 years, such as reduced renal function and medication clearance, even in the absence of renal disease, result in a smaller therapeutic window for safe dosages.
- Opioids used during pregnancy can be associated with additional risks to both mother and fetus.
- Patients with mental health comorbidities and patients with a history of substance use disorders might be at higher risk than other patients for opioid use disorder.
- Prescription drug monitoring programs and urine drug testing provide potential benefits, including the ability to identify patients who might be at higher risk for opioid overdose or opioid use disorder.
- Dose reduction might be associated with unintended negative consequences, such as patients seeking heroin or other illicitly obtained opioids or interference with appropriate pain treatment.
- For the treatment of opioid use disorder, methadone and buprenorphine have been found to increase retention in treatment and to decrease illicit opioid use among patients with opioid use disorder involving heroin. (CDC, 2016a)
Paradoxically, despite an enormous rise in spending and prescription, there is limited evidence to support the efficacy of opioids in chronic noncancer pain management. In a European survey on chronic pain, 15% of respondents felt that their medications were not very, or not at all, effective (Xu & Johnson, 2013).
A systematic review by Chou and colleagues suggested limited efficacy of long-term opioid therapy over short-term treatment or placebo, while an evidence review by the Institute of Medicine concluded that the effectiveness of opioids as pain relievers, especially over the long term, is somewhat unclear (Xu & Johnson, 2013).
Opioid-Induced Hyperalgesia
Apart from potential side effects, tolerance, and addiction, opioid use can be associated with opioid-induced hyperalgesia, which is defined as a state of nociceptive sensitization caused by exposure to opioids. It is characterized by a paradoxical response whereby a patient receiving opioids for the treatment of pain actually becomes more sensitive to pain (Suzan et al., 2013).
Opioid-induced hyperalgesia in the post operative period has been reported following the administration of short-acting opioids during surgery. Additional evidence comes from opioid addicts on methadone maintenance therapy, in whom decreased tolerance to cold pain has been reported. Mixed results are found regarding hyperalgesia in patients with chronic pain who receive intermediate-term opioid treatment (Suzan et al., 2013).
Tolerance, Dependence, and Addiction
Thirty years ago, I attended medical school in New York. In the key lecture on pain management, the professor told us confidently that patients who received prescription narcotics for pain would not become addicted.
While pain management remains an essential patient right, a generation of healthcare professionals, patients, and families have learned the hard way how deeply misguided that assertion was. Narcotics—both illegal and legal—are dangerous drugs that can destroy lives and communities.
Thomas Frieden, MD
Director, CDC
A number of terms and definitions are regularly used to define behaviors that are associated with the misuse and abuse of drugs. These terms are imprecise and at times confusing and can reflect societal attitudes and beliefs about drug abuse. To address this issue and to clarify the terms dependence and addiction, particularly in opioid-treated patients, new definitions for drug addiction have been included in the 2013 DSM-V update. The term “substance dependence”—used in DSM-III and DSM-IV—has been replaced by the terms “substance use disorder” and “opioid use disorder” (IASP, 2013).
Opioid use disorder is a problematic pattern of opioid use leading to clinically significant impairment or distress. It is manifested by specific criteria such as unsuccessful efforts to cut down or control use and use resulting in social problems and a failure to fulfill major role obligations at work, school, or home. This diagnosis has also been referred to as “abuse or dependence” and “addiction” in the literature, and is different from tolerance (diminished response to a drug with repeated use) and physical dependence (adaptation to a drug that produces symptoms of withdrawal when the drug is stopped), both of which can exist without a diagnosed disorder (CDC, 2016b).
Changes in the DSM-V state that two items (not including tolerance and withdrawal) are needed from a list of behaviors suggesting compulsive use to meet the criteria for substance use disorder (SUD). Tolerance and withdrawal are not counted for those taking prescribed medications under medical supervision such as analgesics, antidepressants, anti-anxiety medications, or beta-blockers (IASP, 2013).
Tolerance
The Brain’s Reward Circuit
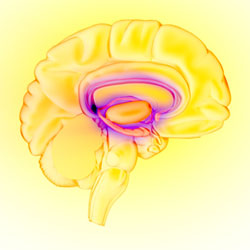
The limbic system—the brain’s reward circuit. Source: National Institute on Drug Abuse.
Tolerance is a state of adaptation in which a drug becomes less effective over time, which means a larger dose is needed to achieve the same effect. Tolerance occurs because some drugs cause the brain to release 2 to 10 times the amount of dopamine than natural rewards do. In some cases, this occurs almost immediately—especially when drugs are smoked or injected—and the effects can last much longer than those produced by natural means. The resulting effects on the brain’s pleasure circuit dwarfs those produced by naturally rewarding behaviors.
The brain adapts to these overwhelming surges in dopamine by producing less dopamine or by reducing the number of dopamine receptors in the reward circuit. This reduces the user’s ability to enjoy not only the drugs but also other things in life that previously brought pleasure. This decrease compels the person to keep abusing drugs in an attempt to bring the dopamine function back to normal, but now larger amounts of the drug are required to achieve the same dopamine high (NIDA, 2016a).
Dependence
Dependence is a state of adaptation characterized by symptoms of withdrawal when a medication is abruptly stopped, the dose is rapidly reduced, or an antagonist is administered. The seriousness of the withdrawal symptoms depends upon the drug being used and the extent of its use. It is a term often misused as a synonym for addiction, but the two terms are not synonymous. For some drugs, such as alcohol or benzodiazepines, withdrawal symptoms can be serious and life-threatening.
An example of dependence is a patient who is on morphine for several months for chronic back pain. If the morphine is discontinued all at once, a flu-like syndrome will quickly develop, accompanied by nausea, stomach pains, and malaise. These symptoms of physical dependence will disappear if the morphine is resumed. Once a person has been on opioids for a period of time, the medication must be tapered off to avoid withdrawal symptoms.
Addiction
It is often said that addiction is easy to recognize, that it rarely arises during the treatment of pain with addictive drugs, and that cases of addiction during pain treatment can be managed in much the same way as other addictions, but such generalizations grossly oversimplify the real situation.
International Association for the Study of Pain
Addiction is defined as a chronic, relapsing disease that is characterized by compulsive drug seeking and use, despite the known, harmful consequences. Addiction involves a psychological craving and is considered a brain disease because drugs change the brain’s structure and function. Brain changes can be long lasting and can lead to the harmful behaviors seen in people who abuse drugs. Although taking drugs at any age can lead to addiction, research shows that the earlier a person begins to use drugs the more likely they are to progress to more serious abuse (NIDA, 2014a).
Addiction
The term addiction may be regarded as equivalent to a severe substance use disorder as defined by the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5, 2013) (NIDA, 2014a).
Opioids are highly addictive and rates of addiction among patients receiving opioids for the management of pain vary from 1% to 50%, which suggests uncertainty about what addiction really is and how often it occurs (IASP, 2013). Savage and colleagues introduced the four “Cs” criteria for identifying opioid addiction in chronic pain population:
- Impaired Control over drug use
- Compulsive use
- Continued use despite harm
- Unmanageable drug Craving (Chang & Compton, 2013).
Opioids in Patients with a History of Substance Abuse
Treating chronic pain with chronic opioid therapy in individuals with a history of a substance use disorder (SUD), whether active or in remission, presents a challenge to pain clinicians. This is, in part, due to concerns about the patient relapsing to active substance abuse. In addition, clinicians may confuse “drug-seeking” behaviors with addictive disease (Chang & Compton, 2013).
The goal of chronic pain treatment in patients with SUD is the same as that for patients without SUD: specifically, to maximize functionality while providing pain relief. However, reluctance to prescribe opioids and poor understanding of the complex relationship between pain and addiction often results in undertreated pain in this population (Chang & Compton, 2013).
When estimating the presence of substance use disorder in chronic pain patients, terminology is important. It is increasingly understood that SUD cannot be defined by physical dependence and tolerance, as these are predictable physiologic consequences of chronic opioid use. Reflecting this, in the DSM-V, tolerance and withdrawal are not counted as criteria for the substance use and addictive disorder diagnosis if a patient is taking an opioid analgesic under medical supervision (Chang & Compton, 2013).
The overall prevalence of substance use disorders in chronic pain patients ranges from 3% to 48% depending on the population sampled. It has been reported that 3% to 11% of chronic pain patients with a history of substance use disorder may develop opioid addiction or abuse, whereas only less than 1% of those without a prior or current history of SUD develop the same (Chang & Compton, 2013).
When screening patients for a history of substance abuse, one of the easiest tools to use is the National Institute on Drug Abuse (NIDA) Drug Use Screening Tool. It begins with a Quick Screen, which recommends that clinicians ask one question:
“In the past year, how often have you used alcohol, tobacco products, prescription drugs for nonmedical reasons, or illegal drugs?”
Patients are asked to respond on a 5-point continuum: never, once or twice, monthly, weekly, or daily/almost daily. A response of “at least 1 time” when asked about frequency of prescription or illegal drug use is considered a positive result. Recent research has identified that this single-question screening test is highly sensitive and specific for identifying drug use and drug use disorders (NIDA, 2014a).
For those who screen positive for illicit or nonmedical prescription drug use, clinicians can administer the full NIDA-modified Alcohol, Smoking, and Substance Involvement Screening Test (NM-ASSIST). The NM-ASSIST automatically generates a risk level to indicate the level of intervention needed and provides additional resources, such as scripts, on how to discuss drug use with patients, plus resources to link patients to specialty care (NIDA, 2016b).
Untreated Addiction
Patients with an active substance use disorder should be referred to formal addiction treatment. The prescribing clinician should maintain a referral network of substance abuse treatment providers willing to collaborate on providing care to patients with co-morbid pain and substance use disorder. After referral, a pain clinician should continue to work closely with the SUD treatment provider to monitor use behaviors and pain outcomes (Chang & Compton, 2013).
Addiction in Remission
Exposure to psychoactive medications can lead to relapse in patients with a recently or poorly treated substance use disorder. Although concerns of relapse may contribute to clinicians’ reluctance to prescribe chronic opioid therapy for patients whose addiction is in remission, there is evidence that patients with successfully treated addiction can be effectively treated with opioids for chronic pain (Chang & Compton, 2013).
For individuals with addiction in remission, the goal of treatment is the same as that as for all chronic pain patients: to improve pain and maintain functionality. Indicators of successful pain management include:
- The patient’s ability to comply with regimens
- The ability to engage in cognitive-behavioral pain management strategies
- Utilization of positive coping skills to manage stress and
- The ability to establish better social support systems (Chang & Compton, 2013)
The ability to manage a relapse episode is a necessary skill of any chronic opioid therapy prescriber. To assess risk of relapse, a series of questions should be asked at each visit to allow for early identification of high-risk situations and potential coping responses to these stressors (Chang & Compton, 2013):
- How long you been in recovery?
- How engaged are you in addiction recovery efforts and treatment?
- What types of drugs have you abused?
- What are current stressors that might precipitate relapse?
- What are your current protective factors against relapse, including improved coping responses and a social support system?
- How stable you feel in recovery? (Chang & Compton, 2013)
A relapse contract can be developed early in treatment, which is individualized to the patient and specifies steps or actions that will be taken by both the patient and clinician if relapse occurs. The patient’s behaviors with respect to the opioid analgesic regimen provide the best evidence for the presence of active addiction (Chang & Compton, 2013)
Seeking a higher dose of a prescribed medication does not necessarily mean that the patient is drug-seeking. However, losing or forging prescriptions, stealing or having others steal for you, visiting multiple providers for duplicate prescriptions, and injecting oral formulations are signs that the patient is not using the medication appropriately.
Management of pain requires a great degree of trust on both sides. Being consistent, open, and fair are important attributes for the provider. Providing positive feedback, reducing harm through education, and attempting to understand individual circumstances are helpful to the patient. When managing patients with complex chronic pain on long-term opioid therapy, a multi-disciplinary team approach is recommended.
In some instances, a program called opioid reassessment has had success in assessing, monitoring, and treating patients with complex chronic pain on long-term opioid therapy. The Opioid Reassessment Clinic (ORC) at VA Connecticut Healthcare System is an example. Located in the primary care setting, the clinic is staffed by an addiction psychiatrist, an internist with addiction and pain training, a behavioral health advanced practice nurse, and a clinical health psychologist. The clinic has served as a learning opportunity for management of complex chronic pain and opioids over the past several years (Becker et al., 2016).
Using Opioids to Treat Pain in Children
Thankfully, not many children experience the types of cancer pain, extensive trauma, or surgeries that require long-term pain management. However, few pain management products have specific information on their label about their safety and effectiveness in pediatric patients. This even includes several new pain medications that have been approved for use in adults.
To manage pain in pediatric patients, physicians often have to rely on their own experience to interpret and translate adult data into dosing information for pediatric patients.
Sharon Hertz, MD, Director
FDA, Office of New Drugs
Center for Drug Evaluation and Research,
Division of Anesthesia, Analgesia, and Addiction Products
The use of opioids to treat pain in infants and children presents challenges. With rare exceptions, opioids have not been labeled for use in individuals under 18 years of age. There is a dearth of quality studies on pharmacokinetics, pharmacodynamics, safety, and clinical effectiveness. Although acute pain problems in children have many characteristics in common with adults, persistent, recurrent, and chronic pain in infants, children, and adolescents are often qualitatively different from chronic pain problems in adults (Oregon Pain Guidance, 2016).
As with adults, this vulnerable population also appears to be at high risk for opioid toxicity. A study of 960 randomly selected medical records from 12 children’s hospitals in the United States identified 107 adverse drug events with more than half attributable to opioid analgesics. Deaths have been reported in young children related to therapeutic use of codeine and hydrocodone in doses within or moderately exceeding recommended pediatric limits (Chung et al., 2015).
Despite their potential for serious adverse events, opioids are increasingly prescribed for adolescents. Opioid prescriptions for patients between 15 and 19 years of age doubled from 1994 to 2007, with estimates that opioids are prescribed in nearly 6% of ambulatory and emergency department visits made by adolescents in the United States (Chung et al., 2015).
Given the large number of pediatric patients receiving prescribed opioids, there is an urgent need for fundamental epidemiologic studies to inform the risk–benefit decisions of prescribers and families. An essential component of these studies is the identification of serious adverse reactions related to opioids. Epidemiologic studies in adults have developed procedures to identify hospitalizations and deaths related to opioid use. However, similar studies in children are lacking (Chung et al., 2015).
Clinical recommendations for chronic non-malignant pain in children and adolescents include (Walco, 2015):
- Prescribe opioids for acute pain in infants and children only if knowledgeable in pediatric medicine, developmental elements of pain systems, and differences in pharmacokinetics and pharmacodynamics in young children.
- Avoid opioids in the vast majority of chronic nonmalignant pain problems in children and adolescents, as evidence shows no indication.
- Consult or refer to a pediatric pain specialist when chronic pain problems in children and adolescents are complicated or persistent.
Opioids are indicated for a small number of persistent painful conditions, including those with clear pathophysiology and when an endpoint to usage may be defined.
Back Next