Working with older adult patients requires excellent communication skills attuned to their particular concerns. Some considerations are as simple as observing the perhaps-unfamiliar etiquette of their generation. Other considerations are attuned to specific deficits—cognitive, hearing, sight—in each patient. It is important to assume nothing about a new patient but screen for any conditions that might affect communication. Even in a patient with no cognitive impairments and no hearing or vision loss there may be issues related to health literacy.
Health Literacy
Health Literacy is defined in the Institute of Medicine report, Health Literacy: A Prescription to End Confusion, as “the degree to which individuals have the capacity to obtain, process, and understand basic health information and services needed to make appropriate health decisions.”
Health literacy requires a complex group of reading, listening, analytical, and decision-making skills, as well as the ability to apply these skills to health situations. For example, it includes the ability to understand instructions on prescription drug bottles, appointment slips, medical education brochures, doctor's directions and consent forms, and the ability to negotiate complex healthcare systems.
More recent definitions focus on specific skills needed to navigate the healthcare system and the importance of clear communication between healthcare providers and their patients. Both healthcare providers and patients play important roles in health literacy. The number of definitions for health literacy demonstrates how the field has evolved (NNLM, n.d.).
Older adults have documented health literacy problems. The landmark National Assessment of Adult Literacy (2003) contained a component designed specifically to measure health literacy. Data from the survey showed that 75% of adults older than age 60 had difficulty in using print materials, 80% had difficulty using documents such as forms or charts, and 68% had difficulty interpreting numbers and doing calculations (CDC, 2018b). Understanding this is critical for those working directly with older adults in healthcare settings and for those preparing data-gathering forms and health information material intended to help elders manage their care.
Good health literacy includes the ability to:
- Access healthcare services
- Analyze relative risks and benefits
- Calculate dosages
- Communicate with healthcare providers
- Evaluate information for credibility and quality
- Interpret test results
- Locate health information
In order to accomplish these tasks, individuals must be:
- Visually literate (able to understand graphs or other visual information)
- Computer literate (able to operate a computer)
- Information literate (able to obtain and apply relevant information)
- Numerically or computationally literate (able to calculate or reason numerically)
Oral language skills are important as well—patients must be able to articulate their health concerns and describe their symptoms accurately. They need to ask pertinent questions and be able to understand spoken medical advice and treatment directions. In an age of shared responsibility between healthcare provider and patient, patients need strong decision-making skills. Increasingly, health literacy also includes the ability to search the Internet and evaluate healthcare websites.
Anyone might have low health literacy, including people with good literacy skills. Even those who have a medical background can have trouble understanding healthcare information at some point in their lives (NNLM, n.d.).
Obtaining a Medical History
[The following information is taken largely from NIA, 2017a.]
For elder patients, obtaining a good history is crucial; it should include social circumstances, lifestyle, and both medical and family history. If feasible, gather preliminary data before the session by requesting previous medical records or having the patient and family members fill out forms at home. Try to structure questionnaires for easy reading by using large type and providing enough space between items for people to respond.
Try to have patients tell their story only once. For older patients who are ill, re-telling can be tiring. If the patient has trouble with open-ended questions, make greater use of yes-or-no or simple-choice questions. During the interview, sit and face the patient at eye level. Use active listening skills, responding with brief comments such as “I see” and “Okay.” Remember that the interview itself can be beneficial. Giving a patient the chance to express concerns to an interested person can be therapeutic.
Older adults often have sensory impairments that affect communication. Vision and hearing deficits are common. Screen for these so you can check to make sure that hearing aids are in and working or that glasses are available. Be prepared to adjust your delivery if the devices were left at home.
Older patients often have multiple chronic conditions and may have vague complaints or atypical presentations. Thinking in terms of current concerns rather than a chief complaint might be productive. Asking about the patient’s major concern first then allowing them to talk without interruption may help them. But when they finish, probe gently to ask “Is there anything else?” which may help to get all their concerns out on the table before proceeding. If the main concern is a sensitive topic it may not be the first thing the patient brings up. Encouraging patients (or caregivers) to bring a written list of concerns and questions can be useful.
Ask about medications including OTC items, nose sprays and eye drops, supplements, teas, and prescriptions from all the patient’s other providers. Again, asking the patient to bring a list of these items can save time and reduce the chances of overlooking something. This is also a good time to see if a medical alert ID is needed and if the patient has one.
Obtain a thorough family history. This information can provide critical information about family medical conditions; help elicit opinions regarding illness and death, possibly provide an opening to inquire about advance directives; give information about the role relatives play in the patient’s support system, currently or for the future; and identify caregivers the patient relies on, whether paid or unpaid.
Ask question about functional status and ADLs. Inquire about any recent important changes in the patient’s life, including the death of someone close, or a change in living arrangements or financial status.
Social history questions that inquire about where they live and specific living arrangements; access to transportation; eating habits; tobacco, drug, and alcohol use; typical activities, including work; education; and financial situation can all be relevant as you try to devise realistic interventions and understand any problems with treatment adherence.
There are a number of sensitive subjects that can be hard for both providers and patients but it is incumbent on healthcare professionals to find a way to initiate these conversations. These often include when to stop driving, end-of-life plans and advance directives, financial problems, long-term care, abuse, and medical issues such as incontinence, sexuality, substance abuse, and mental health.
Useful conversational techniques include framing questions as common concerns of many people, and using a medication conflict as a way to bring up the issue of driving. Keeping relevant printed materials available in waiting areas is a good practice. Many agencies and organizations—including the National Institute on Aging, CDC, AARP, Alzheimer’s Association, and others—provide printed and online information to train providers and offer materials that can be distributed to patients.
The more complete a life story you can obtain for your patient the better you can understand and care for them. Time constraints may mean that you acquire the information over multiple visits.
Always treat the patient with respect regardless of their mental and physical status. When in doubt, address a patient as Miss, Mrs., or Mr. until you determine if they prefer something else. Speak clearly in a normal voice and avoid endearments such as “Honey” or “Darling.” If the patient’s caregiver is present, do not speak to the caregiver as if the patient were not there. Adjust what is needed to the needs of the patient in that situation.
Give the person the opportunity to ask questions and verify that they understand any diagnosis, treatment, and follow-up instructions. In many offices now, electronic health record systems generate visit summaries and instructions for the patient. If not, older patients many need some information and instructions written out.
Screening Categories
Assessing Sensory Function
One of the challenges of caring for older people is the atypical presentation of symptoms. Deterioration in level of functioning is often the first symptom in an older person with an acute illness. An older adult may evidence only difficulty with ambulation or mentation when they are ill, while a younger person presents with completely different symptoms. Pneumonia in an older person may present with a change in mental status and a UTI may present as a fall. Vomiting may be the only symptom of a heart attack. Changes in vision, hearing, balance and postural control, or sensory loss can affect mobility and should be thoroughly assessed in older patients.
Vision
Approximately 12 million Americans 40 years and older have vision impairment, including 1 million who are blind, 3 million who have vision impairment after correction, and 8 million who have vision impairment due to uncorrected refractive error.
Even though 61 million adults in the United States are at high risk for serious vision loss, only half visited an eye doctor in the past 12 months. National and state data show that more than half of adult Americans who did not seek eye care lacked awareness of the potential problems or were concerned about the costs; concerns often exacerbated by lack of adequate health insurance.
Ninety percent of blindness caused by diabetes is preventable, and while not all vision loss is correctable, early detection and timely treatment of eye conditions such as diabetic retinopathy has been found to be efficacious and cost effective.
Vision loss causes a substantial social and economic toll for millions of people including significant suffering, disability, loss of productivity, and diminished quality of life. More than 70% of survey respondents in a 2005 survey consider vision loss would have the greatest impact on their day-to-day life, yet less than 11% were aware that there are no early warning signs of glaucoma and diabetic retinopathy (CDC, 2017g).
Healthcare providers in many situations will be in a position to do basic screening and/or inform patients and encourage them to make an appointment with an eye care professional.
Hearing
Approximately 1 in 3 people between the ages of 65 and 74 has hearing loss and nearly half of those older than 75 have difficulty hearing. Having trouble hearing can make it hard to understand and follow a doctor's advice, to respond to warnings, and to hear doorbells and alarms. It can also make it hard to enjoy talking with friends and family. All of this can be frustrating, embarrassing, and even dangerous (NIDCD, 2018).
Healthcare providers can screen for and manage diseases, conditions, and medications that may be causing hearing loss. They can be a safe place for patients to discuss hearing loss and how it is affecting their quality of life, and they can provide information about hearing problems and their treatment and offer referrals to hearing aid or other specialists.
Balance and Postural Control
[This section is taken largely from NIA, 2017d.]
Balance problems are among the most common reasons that older adults seek help from a doctor. They are often caused by disturbances of the inner ear. Vertigo, the feeling that you or the things around you are spinning, is a common symptom.
Having good balance means being able to control and maintain body position, whether moving or remaining still. Good balance helps one walk without staggering, get up from a chair without falling, climb stairs without tripping, and bend over without falling. Good balance is important to help people get around, stay independent, and carry out daily activities. Balance disorders are one reason older people fall.
People are more likely to have problems with balance as they get older. But age is not the only reason these problems occur. In some cases, one can reduce the risk for certain balance problems.
Some balance disorders are caused by problems in the inner ear. The part of the inner ear that is responsible for balance is the vestibular system, also known as the labyrinth. A condition called labyrinthitis occurs when the labyrinth becomes infected or swollen. It is typically accompanied by vertigo and imbalance. Upper respiratory infections, other viral infections, and, less commonly, bacterial infections can also lead to labyrinthitis.
Some diseases of the circulatory system, such as stroke, can cause dizziness and other balance problems. Low blood pressure can also cause dizziness. Head injury and many medicines may also lead to balance problems as well. Symptoms of balance disorders can include:
- Staggering when walking
- Teetering or falling when standing up
- Dizziness or vertigo
- Falling or feeling like falling
- Lightheadedness, faintness, or a floating sensation
- Blurred vision
- Confusion or disorientation
Other symptoms might include nausea and vomiting; diarrhea; changes in heart rate and blood pressure; and fear, anxiety, or panic. Symptoms may come and go briefly or last a long time, which can result in fatigue and depression.
Balance disorders can be signs of other health problems, such as an ear infection, stroke, or multiple sclerosis. In some cases, a balance disorder can be treated by seeking medical treatment for the illness that is causing the disorder.
Some exercises help make up for a balance disorder by moving the head and body in certain ways. The exercises are developed especially for a patient by a professional (often a physical therapist) who understands the balance system and its relationship with other systems in the body.
Some balance problems can be managed with lifestyle changes: lowering sodium intake, maintaining a healthy weight, exercising, drinking plenty of fluids, avoiding alcohol, and being cautious regarding body posture and movement. If a balance disorder cannot be fully relieved, referral to a vestibular rehabilitation therapist can help the person cope with dizziness.
Healthcare providers can screen for and manage diseases, conditions, and medications that may be causing or contributing to balance disorders. They can also provide information and referrals to specialists. Additional information about fall risk and prevention appears later in this class.
For more information about older adults and balance problems, click here.
Assessing the Skin
Skin disorders are so common among older people that it is often hard to tell normal changes from those related to a disorder. More than 90% of all older people have some type of skin disorder. Skin disorders can be caused by many medical conditions as well as allergies, climate, clothing, chemical exposure, indoor heating, and sun exposure (MedlinePlus, 2018k).
When assessing skin color, look for cyanosis (bluish color), which may indicate poor oxygenation arising from respiratory or cardiac problems, or may signal low body temperature. Because skin color varies by race and ethnicity, it is important to inspect the ears, lips, inside of mouth, hands, and nail beds for signs of cyanosis.
The skin, sclera of the eyes, and mucous membranes should be inspected for jaundice, which may indicate liver disease. Skin pallor can indicate anemia. Erythema, or redness of the skin, may be due to fever, alcohol intake, or infection.
Skin should also be assessed for swelling, which can be a sign of injury or fluid retention. Bruising or bleeding of the skin should be noted, as it may indicate blood disorders or abuse.
Pressure Ulcers
Pressure ulcers, sometimes called decubitus ulcers, pressure sores or bedsores, are areas of damaged skin caused by staying in one position for too long. They commonly form where bones are close to the skin, such as ankles, back, elbows, heels, and hips. Patients are at risk if they are bedridden, use a wheelchair, or are unable to change their position. Pressure sores can cause serious infections, some of which are life-threatening (MedlinePlus, 2019e,f)
The Institute for Healthcare Improvement notes that “because muscle and subcutaneous tissue are more susceptible to pressure-induced injury than skin, pressure ulcers are often worse than their initial appearance. Pressure ulcers cause considerable harm to patients, hindering functional recovery, frequently causing pain and the development of serious infections. Pressure ulcers have also been associated with an extended length of stay, sepsis, and mortality” (IHI, 2019).
Pressure ulcers are often associated with nursing homes and long-term skilled care facilities, but some 60,000 deaths occur each year from complications due to hospital-acquired pressure ulcers and they are considered a medical error (Sullivan & Schoelles, 2013) Pressure ulcers can also happen in home care situations and at-risk patients should be given information and instruction on prevention and treatment.
Pressure sores have a variety of treatments. Advanced sores are slow to heal, so early treatment is best (MedlinePlus, 2019e,f).
Pressure Ulcer Risk Assessment
The Braden Scale is one of the most often used pressure ulcer risk assessment tools. It assesses six risk factors: mobility, activity, moisture, sensation, nutrition, and shear. The Braden Scale has high validity and reliability. Perform the risk assessment on admission and repeat if there is a change in the patient’s condition. This scale is valid for use with individuals of all skin tones.
Pressure Ulcer Prevention
“Preventing pressure ulcers entails to two major steps: first, identifying patients at risk; and second, reliably implementing prevention strategies for all patients who are identified as being at risk” (IHI, 2019). The IHI How-to Guide: Prevent Pressure Ulcers (IHI, 2011) (recommended through the AHRQ pressure ulcer prevention site) is available at www.ihi.org.
Basic preventions for pressure ulcers involve:
- Keeping skin clean and dry
- Changing position every 2 hours
- Using pillows and products that relieve pressure (MedlinePlus, 2019e,f)
In healthcare settings key changes recommended by the IHI how-to guide include:
- Inspect skin daily
- Manage moisture on skin
- Conduct a pressure ulcer admission assessment for all patients
- Minimize pressure
- Optimize nutrition and hydration
- Reassess risk for all patients daily (IHI, 2019, 2011)
Moles
During a skin assessment, moles need to be assessed for possible skin cancer. A common mole (nevus) is a small growth on the skin that is usually pink, tan, or brown and has a distinct edge. People who have more than fifty common moles have a greater chance than others of developing melanoma. Most common moles do not turn into melanoma and in older people they tend to fade away (NCI, 2018a).
A dysplastic nevus is an unusual mole that is often large and flat and does not have a symmetric round or oval shape. The edge is often indistinct. It may have a mixture of pink, tan, or brown shades. People who have many dysplastic nevi have a greater chance than others of developing melanoma, but most dysplastic nevi do not turn into melanoma (NCI, 2018a).
Photos of Common Moles
Some moles have been circled by the clinician.
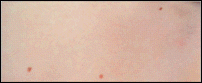
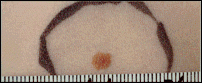
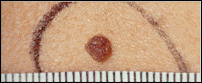
Left: common moles that are evenly tan or brown. Center: a common mole that is round with a distinct edge. Right: A common mole is usually small. This one is less than 5 millimeters (about 1/4 inch).
Photos of Dysplastic Nevi
Some moles have been circled by the clinician.
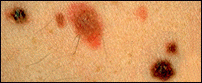
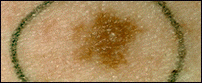
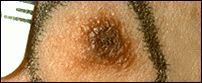
Left: dysplastic nevi that are a mixture of tan, brown, and red/pink. Center: a dysplastic nevus with an irregular edge and the color fading into the skin around it. Right: dysplastic nevus with scaly or pebbly surfaces.


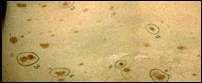
Left: dysplastic nevus with scaly or pebbly surfaces. Center: Dysplastic nevi are often larger than 5 millimeters wide, This one shows a large dysplastic nevus. Right: several large dysplastic nevi circled on a person’s back.
NCI, 2011, https://www.cancer.gov/types/skin/mole-photos.
If the color, size, shape, or height of a mole changes or if it starts to itch, bleed, or ooze, or if a new mole doesn’t look like the client’s other moles, it needs to be checked by a physician. The only way to diagnose melanoma is to remove tissue and check it for cancer cells.
Skin Signs of Elder Abuse
When assessing skin, look for signs of abuse. Healthcare providers are mandated reporters of elder abuse. While one sign does not necessarily indicate abuse, some tell-tale signs that there could be a problem:
- Bruises, pressure marks, broken bones, abrasions, and burns may be an indication of physical abuse, neglect, or mistreatment.
- Bruises around the breasts or genital area may indicate sexual abuse.
- Bedsores, unattended medical needs, poor hygiene, and unusual weight loss are indicators of possible neglect.
Skin Breakdown from Urinary Incontinence
Urinary incontinence can contribute to skin breakdown and infection and also to urinary tract infections (UTIs). It is important that incontinence be managed and that skin be cleansed and dried as soon as possible to prevent these complications.
Assessing Psychosocial Function
Isolation
A 2017 study of adults age 65 and older living in the community found that about 14% of participants could be defined as socially isolated, meaning they have little contact with adult children, other relatives, or friends. This group was more likely to be white male urban dwellers with low income and wealth and more likely to have depression, difficulties with ADLs, and at least five chronic conditions. People who were married were no less likely to be isolated than single people (Gleckman, 2017; AARP, 2017a).
The study found that Medicare spent $1,608 more per year for each socially isolated older adult than it did for adults better connected socially. Socially isolated individuals were 29% more likely to use skilled nursing facilities and incur higher bills. These same individuals were not more likely to use inpatient care (hospitals) but when they did Medicare spent more on them. This may be because socially isolated individuals are sicker when admitted or be unable to transition home as quickly without a support system (AARP, 2017a).
These findings suggest that reducing isolation might improve outcomes for individuals and reduce Medicare spending. The report noted that social isolation is not inevitable with aging (after all, 86% of study participants were not isolated) but “for those older adults who have poor social connections, these findings present an opportunity for state and federal policy makers, along with private-sector actors, to identify promising interventions to alleviate isolation” (AARP, 2017a).
Depression and Suicide
As people age, they tend to go through a lot of changes—death of loved ones, retirement, stressful life events, or medical problems. It’s normal to feel uneasy, stressful, or sad about these changes; but, after adjusting, many older adults feel well again (NIMH, 2016).
Depression is a true and treatable medical condition, not a normal part of aging; however, older adults are at an increased risk for experiencing depression. We know that about 80% of older adults have at least one chronic health condition, and 50% have two or more. Depression is more common in people who also have other illnesses (such as heart disease or cancer) or whose function becomes limited (CDC, 2017i).
Older adults are often misdiagnosed and undertreated. Healthcare providers may mistake an older adult’s symptoms of depression as just a natural reaction to illness or the life changes that may occur as we age, and therefore not see the depression as something to be treated. Older adults themselves often share this belief and do not seek help because they don’t understand that they could feel better with appropriate treatment (CDC, 2017i).
Depression is a medical condition that interferes with daily life and normal functioning. It is not a normal part of aging, a sign of weakness, or a character flaw. Many older adults with depression need treatment to feel better (NIMH, 2016).
Types of Depression
There are several types of depression. The most common include:
- Major depression—severe symptoms that interfere with your ability to work, sleep, concentrate, eat, and enjoy life. Some people may experience only a single episode within their lifetime, but more often, a person may experience multiple episodes.
- Persistent depressive disorder (dysthymia)—depression symptoms that are less severe than those of major depression, but last a long time (at least two years).
- Minor depression—depression symptoms that are less severe than those of major depression and dysthymia, and symptoms do not last long (NIMH, 2016).
Symptoms
Depression may sometimes be undiagnosed or misdiagnosed in some older adults because sadness is not their main symptom. They may have other, less obvious symptoms of depression or they may not be willing to talk about their feelings.
Depression has many symptoms, including physical ones. A person experiencing several of the following symptoms for at least two weeks, may be suffering from depression:
- Persistent sad, anxious, or “empty” mood
- Loss of interest or pleasure in hobbies and activities
- Feelings of hopelessness, pessimism
- Feelings of guilt, worthlessness, helplessness
- Decreased energy, fatigue, being “slowed down”
- Difficulty concentrating, remembering, making decisions
- Difficulty sleeping, early-morning awakening, or oversleeping
- Appetite and/or unintended weight changes
- Thoughts of death or suicide, suicide attempts
- Restlessness, irritability
- Aches or pains, headaches, cramps, or digestive problems without a clear physical cause and/or that do not ease even with treatment (NIMH, 2016)
Risk Factors
Although most cases of depression are diagnosed in young adults, depression can occur at any age. Certain people are at a higher risk for developing depression. Older adults may be at a higher risk if they:
- Are female
- Have a chronic medical illness, such as cancer, diabetes or heart disease
- Have a disability
- Sleep poorly
- Are lonely or socially isolated
They may also be at a higher risk if they:
- Have a personal or family history of depression
- Use certain medications
- Suffer from a brain disease
- Misuse alcohol or drugs
- Have experienced stressful life events such as loss of a spouse, divorce, or taking care of someone with a chronic illness
If other factors are ruled out, a referral can be made to a mental health professional, such as a psychologist, counselor, social worker, or psychiatrist. Some providers are specially trained to treat depression and other emotional problems in older adults and there are sometimes community-based senior mental health wellness programs operated in conjunction with local hospitals or agencies that can be eligible for coverage by Medicare and/or Medicaid (NIMH, 2016; CDC, 2018c; CVMC, 2019).
