Viruses are constantly changing, and this includes SARS-CoV-2, the virus that causes COVID-19. These genetic mutations occur over time and can lead to the emergence of new variants that may have different characteristics than the original virus.
If you think about a virus like a tree growing and branching out; each branch on the tree is slightly different than the others. By comparing the branches, scientists can label them according to the differences. These small differences, or variants, have been studied and identified since the beginning of the pandemic. Multiple variants of the virus that causes COVID-19 have been documented in the U.S. and globally during this pandemic. Sometimes new variants emerge and disappear. Other times, variants emerge and persist.
Although most mutations have little to no effect, in a large population of infected people—as in the current pandemic—some mutations give the virus an evolutionary edge, one that benefits its spread.
Test Your Knowledge
Mutations in the COVID-19 virus:
- Rarely occur.
- Have only been seen in Britain.
- Occur over time and can lead to the emergence of new variants.
- Have not yet been seen in the United States.
Answer: C
Mutations, Variants and Strains
Mutations are changes in the genetic code of a virus that naturally occur over time when a virus makes copies of itself in an infected animal or person. These changes continue to occur as long as the virus spreads through populations. “What we are going to see is a cat-and-mouse game between the virus changing and the vaccine manufacturers having to quickly change their vaccines,” said Devi Sridhar, professor of global public health at the University of Edinburgh (NBC News, 2021).
The terms variant and strain are often used interchangeably, but they have different meanings. If a coronavirus specimen contains one or more mutations that another specimen lacks, but there is no detectable functional difference, it is called a variant. Many mutations do not affect the virus’s ability to spread or cause disease because they do not alter the major proteins involved in infection. However, eventually these are outmatched by variants with mutations that are more beneficial for the virus (CDC, 2021, April 2). If the mutations in a particular variant make the virus “demonstrably different”—more lethal, more able to evade a vaccine or easier to transmit—then it is a distinct strain (Kaplan, 2021).
If a viral mutation makes it more difficult for a virus to spread, it will eventually die out. If a mutation makes it easier for the virus to spread, it will have an advantage over existing strains and will likely become the dominant one (Kaplan, 2021).
Test Your Knowledge
A strain is:
- The same thing as a variant.
- The same as a mutation.
- A virus that has mutations but no functional difference from the original virus.
- A variant that has developed mutations than that make it “demonstrably different” from the original virus.
Answer: D
Genetic Sequencing
Genes in the SARS-CoV-2 genome that contain instructions to build parts of the virus are shown in different colors. For example, the brown section in the picture has genetic instructions to build the Spike protein, which then allows the virus to attach to human cells during infection. This section of the genome serves as a key region for monitoring mutations (CDC, 2021, April 2).

Genes in the SARS-CoV-2 genome that contain instructions to build parts of the virus are shown in different colors. For example, the brown section in the picture has genetic instructions to build the Spike protein, which then allows the virus to attach to human cells during infection. This section of the genome serves as a key region for monitoring mutations (CDC, 2021, April 2).
The SARS-CoV-2 genome encodes instructions organized into sections, called genes, to build the virus. A process called genomic sequencing is used to decode the genes and learn more about the virus. Genomic sequencing allows scientists to identify SARS-CoV-2 and monitor how it changes over time into new variants, understand how these changes affect the characteristics of the virus, and use this information to predict how it might impact health (CDC, 2021, April 2).
Potential Consequences of Emerging Variants
Some potential consequences of emerging variants are the following (CDC, 2021, January 28):
- Ability to spread more quickly in people. There is already evidence that some of the variants spread faster than the original COVID-19 virus.
- Ability to cause either milder or more severe disease in people. In January 2021, experts in the UK reported that the B.1.1.7 variant may be associated with an increased risk of death compared to other variants. More studies are needed to confirm this finding.
- Ability to evade detection by specific viral diagnostic tests. Most commercial reverse-transcription polymerase chain reaction (RT-PCR)–based tests have multiple targets to detect the virus, so that even if a mutation impacts one of the targets, the other RT-PCR targets will still work.
- Decreased susceptibility to therapeutic agents such as monoclonal antibodies.
- Ability to evade natural or vaccine-induced immunity. Both vaccination against and natural infection with SARS-CoV-2 produce a polyclonal response that targets several parts of the spike protein. The virus would likely need to accumulate multiple mutations in the spike protein to evade immunity induced by vaccines or by natural infection.
Among these possibilities, the last—the ability to evade vaccine-induced immunity—is the most concerning. Once a large proportion of the population is vaccinated, there will be immune pressure to favor and accelerate emergence of “escape mutants” with the ability to avoid vaccine antibodies. There is no evidence that this is occurring, and most experts believe escape mutants are unlikely to emerge because of the nature of the virus (CDC, 2021, January 28).
Test Your Knowledge
The most concerning consequence of emerging variants is:
- The ability to evade vaccine-induced immunity.
- Decreased susceptibility to therapeutic agents.
- Ability to evade detection by viral diagnostic tests.
- The ability to spread more quickly in people.
Answer: A
COVID-19 Variants
Coronaviruses are named for the crown-like spikes on their surfaces. Changes in the virus, including changes to its spikes, can affect how it spreads and what happens to people who are infected with it (CDC, 2021, December 13).
Multiple variants of the virus that causes COVID-19 are circulating globally. Currently, The B.1.1.7 (Alpha), B.1.351 (Beta), B.1.617.2 (Delta), and P.1 (Gamma), and Omicron variants circulating in the U.S. Delta and Omicron are currently classified as variants of concern.
Coronavirus Genome
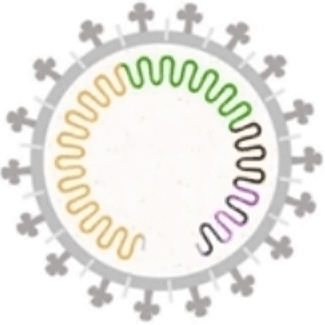
The virus genome is packed inside an envelope that contains proteins, including the spike protein. Source: CDC.
- The United Kingdom (UK) identified a variant called B.1.1.7, (now called the Alpha variant) with a large number of mutations, in the fall of 2020. This variant spread more easily and quickly than other variants and within 3 months, it was the dominant strain in Britain. It is up to 75% more contagious and has a higher viral load than previous strains. In January 2021, experts in the UK reported that Alpha may be associated with an increased risk of death compared to other variant viruses. Alpha has since been detected in many countries around the world and was first detected in the U.S. at the end of December 2020 (CDC, 2021, December 13).
- In South Africa, a variant called B.1.351 (the Beta variant) emerged independently of Alpha. Originally detected in early October 2020, Beta shares some mutations with the Alpha variant. Cases caused by this variant have been reported in the U.S. since January, 2021 (CDC, 2021, December 13).
- In Brazil, a variant called P.1 (the Gamma variant) was first identified in travelers from Brazil in early January. This variant has 17 unique mutations, including 3 in the receptor binding domain of the spike protein that may affect its ability to be recognized by antibodies. It was first detected in the U.S. in January, 2021 (CDC, 2021, December 13).
- A highly infectious Delta variant emerged in the summer of 2021 and quickly became the dominant strain of the virus in the United States. Delta causes more infections, spreads faster, and is nearly twice as contagious as earlier strains. It may cause more severe illness, especially in unvaccinated people. Unvaccinated people are more likely to spread Delta although fully vaccinated people breakthrough infections can also spread the virus. However, vaccinated people appear to be infectious for a shorter period.
In November 2021, a highly transmissible variant called Omicron was identified in South Africa. In the U.S., Omicron has been found in the majority of states. The rapid growth rate in Omicron infections is believed to result from a combination of increased transmissibility and its ability to evade immunity conferred by past infection or vaccination (immune evasion). Immune evasion may play a larger role than increased transmissibility; immunity conferred by prior infection or vaccination is likely to be reduced compared with Delta. Vaccinated people who either receive a booster dose or who were also previously infected are likely to have stronger protection against Omicron (CDC, 2021, December 20). Omicron infections are exponentially increasing in multiple countries with cases doubling every 2-3 days. Recent reports from South Africa and Great Britain suggest that, although highly transmissible, Omicron causes milder illness than other strains.
Variants Can Be Minimized
“Viruses are constantly mutating—or making “typos” in their genetic code—as they spread and make copies of themselves” (AP, 2021). Most of the mutations are not concerning and some may even weaken a virus; however, some mutations make a virus more contagious, deadlier, and/or able to get around vaccine antibodies. Genetic sequencing is used to identify the worrisome variants that may need new treatments and vaccines.
As long as this virus continues to spread, there will be mutations, new variants and strains. Limiting the spread of COVID-19 through measures such as social distancing, mask wearing, and vaccinations gives it less opportunity to mutate and gives us time to get ahead of the virus.
